Overdiagnosis has emerged as a major flash point in the debate over breast screening. But breast imagers can defuse the overdiagnosis argument with five steps that use the power of advanced imaging to make screening more precise and less invasive, according to a new investigation published online March 23 in Academic Radiology.
How? Corresponding author Dr. Christoph Lee of the University of Washington in Seattle and colleagues offered ideas that range from adjusting biopsy protocols and exploring new screening technologies to tapping into the power of radiomics, or assessing quantitative features in images. Other steps include using imaging biomarkers to track malignancy and tailoring treatment to individual patients.
 Dr. Christoph Lee from the University of Washington.
Dr. Christoph Lee from the University of Washington."As members of multidisciplinary breast care teams with imaging expertise, it is imperative that radiologists engage in this issue by examining how current or emerging advanced breast imaging technologies can lessen the potential harms of overdiagnosis," the group wrote.
Guidelines spark debate
Recent recommendations on breast screening from the U.S. Preventive Services Task Force (USPSTF) and the American Cancer Society (ACS) have once again sparked debate about the benefits and harms of breast cancer screening. Much emphasized among the list of potential harms is overdiagnosis and overtreatment, which remain difficult to quantify, according to Lee and colleagues (Aca Rad, March 23, 2016).
Some critics claim that breast imagers are a major contributor to the problem of overdiagnosis, defined as the detection of conditions that may never develop into a threat to an individual's health. But finding a malignancy at screening doesn't necessarily affect the patient -- it's the subsequent intervention and treatment that do, the authors wrote. And because eliminating screening mammography is not only unrealistic but also unethical, radiologists need to consider how advanced imaging could address the issue of overdiagnosis.
5 areas to consider
Lee's team highlighted five areas for further investigation in an effort to encourage breast imagers to take the lead in reducing breast cancer overdiagnosis and overtreatment.
Adjust biopsy thresholds. The American College of Radiology's BI-RADS 4 category ("suspicious abnormality") prompts breast imagers to order a biopsy to rule out breast cancer. But could low-risk findings, such as microcalcifications that may be ductal carcinoma in situ (DCIS), be tracked with imaging instead? It's possible, according to the authors, and such adjustments could include different biopsy thresholds based on individualized risk. "It makes a lot of sense to adjust biopsy protocols," Lee told AuntMinnie.com. "Overall, the concept of 'less is more' is a good one."
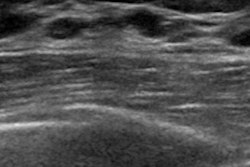
Explore newer image-based screening technologies. Digital breast tomosynthesis (DBT), supplemental screening ultrasound, and breast MRI all show promise, Lee and colleagues wrote. Research on DBT suggests that it decreases false positives and finds cancers that are clinically significant. Ultrasound appears to increase cancer detection in women with dense breast tissue. And breast MR -- particularly when performed with an abbreviated acquisition protocol -- appears to rule out malignancy, with a negative predictive value of 99.8%.
Investigate the potential of radiomics. Radiomics takes quantitative features from medical images to create prognostic models that connect these features with phenotypes or genotypes. The field could help clinicians personalize screening for their patients, according to Lee. "We need to develop functional imaging techniques that get at tumor biology," he said.
Use imaging biomarkers to track malignancy. DCIS lesions account for one in five new cancer diagnoses in the U.S., but how to pathologically diagnose DCIS remains controversial, in part because it's poorly understood how DCIS progresses, Lee's group wrote. Pathologic characterization tends to be difficult to reproduce and prone to interobserver variability. However, technology such as breast MR with dynamic contrast enhancement or diffusion-weighted imaging could help radiologists better assess lesions' biological features. In fact, an ongoing trial (ECOG-ACRIN 4112) is exploring whether MR, along with Oncotype DX DCIS scores, could help patients with low-risk DCIS lesions avoid radiation therapy. "This research is exciting because it's combining advanced imaging and biomarkers to try to do less harm and avoid overtreatment," Lee said.
Tailor treatment protocols. As well as DCIS, there are small invasive cancers that may never threaten a woman and can contribute to overdiagnosis and overtreatment. What's needed is a shift from disease-specific treatment to tumor-specific treatment that is tailored to each patient, according to Lee and colleagues. Radiologists can take an active role in developing decision-making tools that will characterize the aggressiveness of newly identified cancers, and offer both predictive and prognostic information, they wrote.
Leading the charge
What's the bottom line? Breast imagers can guide the effort toward avoiding harms associated with screening, Lee's group concluded. Newer technologies such as DBT can help decrease the number of false positives generated by screening; radiologists can help shape the conversation about screening frequency and biopsy thresholds; and radiomic approaches can help identify and quantify imaging features associated with tumor physiology and biology.
"All five of these suggestions are in the domain of radiologists -- even radiomics is based on MR procedures," Lee said. "We can and should lead the charge toward steering breast cancer screening away from harms and toward benefits."