It's no secret that radiology is facing fiscal trials. As reimbursement amounts contract and practice budgets get squeezed, radiologists -- particularly breast imagers -- are challenged to provide the best patient care possible at the most efficient cost.
It might seem that there wouldn't be much room for innovation in this type of economic environment. But at the 2008 RSNA meeting in Chicago, researchers from around the world presented findings on three up-and-coming breast imaging applications that could help clinicians make diagnoses with greater accuracy -- good news not only for patient care, but also for a practice's bottom line.
DBT distinguishes between malignant and benign
Dr. Mark Helvie and colleagues from the University of Michigan Comprehensive Cancer Center in Ann Arbor compared characterization of benign and malignant breast masses by digital breast tomosynthesis (DBT) mammography using a prototype system developed by GE Global Research.
Their study included 174 women with breast masses documented by mammography, sonography, or physical exam who had been scheduled for biopsy, for a total of 382 DBT views of masses in 177 breasts. The DBT images were reconstructed to 1-mm slice spacing, and each case was assessed for the likelihood of a mass being present, mass visibility, and probability of malignancy on a 10-point scale.
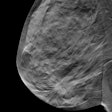
The researchers found that DBT helped distinguish between benign and malignant masses, and that cancers in particular appeared as irregularly shaped masses with spiculated margins in the DBT views (81% of the cancers showed both these characteristics, compared to 11% of the benign lesions).
Mammographic density was 43% fatty/scattered and 57% heterogeneous/extremely dense. Of the 382 views, 81 were malignant, of which 98% were invasive. Mean size was 16.3 mm for benign lesions and 14.7 mm for cancers.
"With DBT, cancers look more malignant," Helvie said. "They're more likely to be spiculated or irregular in shape, and because of this, we feel that DBT shows promise for characterization of benign and malignant cancers."
CEDM shows higher diagnostic accuracy
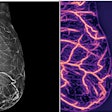
French researchers evaluated the diagnostic accuracy of dual-energy contrast-enhanced digital mammography (CEDM) as an adjunct to mammography, compared to the accuracy of mammography alone.
Dr. Clarisse Dromain from the Institut Gustave Roussy in Villejuif, France, gave 107 women with 133 suspicious mammography findings CEDM exams between March 2007 and March 2008, with the gold standard being the pathology reports for all cases; pathology results identified 80 benign and 53 malignant lesions. Patients were injected with 1.5 mL/kg of contrast. A mediolateral oblique view (MLO) was taken at two minutes, followed by a craniocaudal view (CC) at four minutes.
The radiologist reader first interpreted the mammography images alone, then the mammography images with the CEDM images. The reader evaluated each lesion for confidence of presence (5-level scale), probability of malignancy (7-level scale), and BI-RADS assessment.
|
The researchers found no significant differences between the specificities for mammography alone and mammography with CEDM.
"Our results show a significantly higher diagnostic accuracy of two-view dual-energy contrast-enhanced digital mammography versus mammography alone," Dromain said.
Photon-counting detectors reduce motion artifacts
Dr. Felix Diekmann and colleagues from Charité Medical University in Berlin investigated whether slot-scan dual-energy mammography with a photon-counting detector could be used for clinical mammography.
Diekmann's team used a plexiglass phantom to simulate tumors ranging in thickness from 2.5 mm to 10 mm, and also used iodine concentrations of Ultravist 370 contrast agent (Bayer HealthCare Pharmaceuticals, Wayne, NJ) ranging from 0 mg/mL to 8 mg/mL to simulate tumor enhancement. Contrast-to-noise ratios were calculated as well.
Minimum iodine concentrations needed were 1 mg/mL to visualize the 10-mm tumor and 4 mg/mL for the 2.5-mm tumor. Contrast-to-noise ratios for tumors relative to water are shown below:
|
"Based on previous observations that breast tumors take up about 3-4 mg/mL of iodine, we found that this technique shows that tumors as small as 2.5 mm can be detected," Diekmann said. "And the contrast-to-noise ratios are acceptable for diagnostic purposes and at least equal to the results found in earlier studies with flat-panel detectors."
By Kate Madden Yee
AuntMinnie.com staff writer
January 20, 2009
Related Reading
FFDM performs well versus analog for screening, studies show, January 6, 2009
Siemens highlights new dual-source CT, breast MRI, DBT systems, December 1, 2008
Molecular breast imaging offers promise as mammography adjunct, September 15, 2008
Pilot study: DBT's role needs further research, April 18, 2008
ECR sessions examine DBT's effectiveness, March 7, 2008
Copyright © 2009 AuntMinnie.com