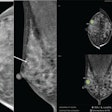
For women who carry the heredity risk of breast cancer, conventional mammography is simply not enough to detect developing disease. On the other hand, risk-reducing surgery, such as prophylactic mastectomy, may be too drastic a response to the presence of BRCA1 and BRCA2 mutations.
A new study in the Journal of the American Medical Association promotes MRI surveillance due to its higher sensitivity in these women who are younger, have denser breasts, and tend to present with cancer between screening rounds.
Dr. Ellen Warner and colleagues conducted a surveillance study on 236 Canadian women, ages 25-65, with BRCA1 and BRCA2 mutations. The authors, including breast imaging specialists Drs. Petrina Causer and Roberta Jong, hailed from Sunnybrook and Women's College Health Sciences Centre, the University of Toronto, and North York General Hospital, all in Toronto.
"The sensitivity of mammography is inversely related to breast density ... furthermore, BRCA1-related cancers tend to be cellular with round pushing margins ... resulting in a more benign mammographic appearance," they wrote (JAMA, September 15, 2004, Vol. 292:11, pp. 1317-1325).
The patients had one to three annual screening exams with four modalities. A clinical breast evaluation (CBE) was performed at six-month intervals. Four-view film-screen mammograms were taken and scored according to BI-RADS. Screening ultrasound was done with a 7.5-MHz transducer, and the results were categorized by the BI-RADS ultrasound lexicon.
The women underwent simultaneous bilateral, gadolinium-enhanced MRI on a 1.5-tesla scanner (Signa, GE Healthcare, Waukesha, WI). The imaging protocol included 3D SPGR in the coronal plane, fat-suppressed T2-weighted FSE, and dual 3D sagittal TR-interleaved SPGR sequences. If a suspicious area of enhancement was detected, a diagnostic MR scan was performed.
Core and excisional biopsies, under ultrasound or stereotactic guidance, were performed on all lesions with a BI-RADS score of 4 or 5. Differences in the relative sensitivity of each modality were compared using a Fischer exact test. For each modality, the positive predictive value (PPV) was defined as the number of biopsy-proven cancers as a proportion of the number of suspicious studies that required biopsy.
According to the results, a total of 22 cancers were detected, 16 of which were invasive, and six of which were ductal carcinoma in situ (DCIS). Of these, 17 (77%) were found by MRI. Mammography detected eight (36%), ultrasound pinpointed seven (33%), and two were found by CBE (9.1%).
MRI's sensitivity was 77% compared to 36% for mammography, 33% for ultrasound, and 9.1% for CBE. The specificity for MRI was 95.4%, 99.8% for mammography, 96% for ultrasound, and 99.3% for CBE. All modalities combined had a sensitivity of 95% versus 45% for mammography and CBE together.
With regard to false-positive results, 14% of the 236 patients in the study had a biopsy for what was ultimately benign disease. The authors reported that this benign biopsy rate was significantly higher (11%) at the first screening round compared to 6.6% during the second, and 4.7% during the third.
"The PPV of MRI is consistently higher than that of ultrasound," they said. "The specificity of MRI is relatively low in the first year of screening." Over the course of three screening rounds, the PPV of MRI was 42%, 56%, and 50% versus ultrasound at 23%, 44%, and 0%.
In an accompanying editorial, Drs. Mark Offit and Mark Robson praised the study for illustrating the value of MRI in these patients, but they cautioned that "a number of fundamental questions remain."
Issues that still need to be addressed are when MRI screening should be done, and whether MRI results would translate to a reduction in breast cancer-related mortality, said Offit and Robson, who are from the Memorial Sloan-Kettering Cancer Center in New York City.
"Women and physicians must ... be aware that both sensitivity and specificity of screening MRI may be substantially less than described if different imaging protocols are followed or if experienced radiologists and suitable technology, including the capability to perform magnetic resonance-guided biopsies, are not available," they wrote (JAMA, September 15, 2004, Vol. 292:11, pp. 1368-1370).
Warner's group acknowledged that experience does play an important part in the success rate of breast MRI. One unexpected finding of their study was that the prevalence of cancer on the second screening round was not markedly lower than on the first round.
"Subtle MRI changes on the first screen could have been missed ... because of relative lack of experience performing or reading MRI at the beginning of the study," they said. However, they pointed out that "the MRI recall rates in our study decreased substantially from 26% on the first round of screening to 13% on the second round, and 10% on the third round."
With screening mammography only able to detect 50% of breast tumors in BRCA carriers, the group reiterated that MRI-based screening is still the front-runner modality for surveillance in this patient population.
By Shalmali Pal
AuntMinnie.com staff writer
September 14, 2004
Related Reading
MRI breast cancer test benefits high-risk women, July 29, 2004
MRI shows strength in breast tumor detection and quantification, June 7, 2004
Annual breast cancer screening may not suffice for BRCA-positive women, April 12, 2004
Women with genetic history of breast cancer benefit from MR screening, November 30, 2003
Copyright © 2004 AuntMinnie.com