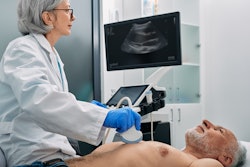
Transesophageal echocardiography (TEE) may not improve outcomes for CPR patients, but it may still have some benefits, according to research published March 23 in JAMA Internal Medicine.
A team led by Sheng-En Chu, MD, from Far Eastern Memorial Hospital in New Taipei City, Taiwan, found that TEE-guided CPR with an adjusted compression site after arrival did not significantly improve clinical outcomes. However, it did improve hemodynamic efficacy without adding more harm.
“Given that the trial was underpowered due to optimistic effect size assumptions, these neutral findings should be interpreted with caution,” the Chu team wrote.
CPR guidelines recommend chest compressions at the lower half of the sternum. However, this may lead to aortic valve compression and poor outcomes.
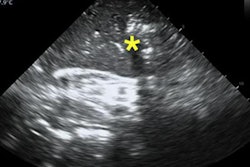
Prior studies in both animals and humans suggest that avoiding the aortic valve and instead targeting the left ventricle could improve CPR quality. TEE allows for real-time identification of the area of maximal compression without interrupting chest compressions.
Chu and colleagues studied whether TEE-guided CPR that avoids aortic valve compression and targets the left ventricle could improve outcomes in patients with nontraumatic out-of-hospital cardiac arrest.
The cluster-randomized clinical trial took place at one center and included 132 patients. Of these, 66 underwent TEE-guided CPR while the remaining 66 underwent conventional CPR.
Both groups had similar rates of sustained return of spontaneous circulation (primary outcome), as well as similar secondary outcomes, such as return of spontaneous circulation, survival, and intensive care unit (ICU) admission.
Comparison between conventional, TEE-guided CPR groups | ||
Measure | Conventional CPR | TEE-guided CPR |
Sustained return of spontaneous circulation | 26 patients | 29 patients |
Return of spontaneous circulation | 33 patients | 33 patients |
Survival to ICU admission | 20 patients | 20 patients |
For the primary outcome, TEE achieved a cluster-adjusted odds ratio of 1.21. No patient in the TEE-guided group survived to discharge.
The researchers also analyzed data on end-tidal carbon dioxide (ETCO2), the level of carbon dioxide that is released at the end of an exhaled breath. While these data were missing in 59 patients, the researchers found that the proportion of patients achieving ETCO2 greater than 20 mm Hg did not differ statistically between the TEE-guided and conventional groups.
However, temporal analysis showed that the TEE-guided group had significantly higher ETCO2 values during the 11- to 20-minute interval after arrival in the emergency department. This included an estimated average difference of 8.61 mm Hg between the two groups.
The study being underpowered is due to “overly optimistic assumptions regarding the anticipated difference” in sustained return of spontaneous circulation rates between the two groups, the study authors wrote.
They called for “larger, adequately powered” trials to find out the true clinical impact of TEE-guided compressions.
While the study did not show significant improvements with TEE guidance, the results could help guide subsequent interventions and investigations, according to an accompanying editorial written by Teva Brender, MD, from the University of California, San Francisco.
Brender highlighted that one important takeaway from the study is that TEE-guided CPR may be most appropriate in the inpatient setting.
“Future research will help clarify the utility, feasibility, and safety of TEE-guided CPR, including which settings and patient populations have a sufficiently high likelihood of functional recovery to justify the addition of this resource-intensive intervention,” he wrote.
Read the full study here.