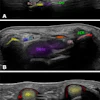
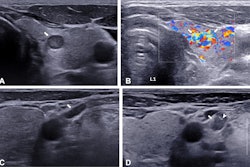
Reducing ultrasound referrals for nonpalpable nodules could help address thyroid cancer overdiagnosis, according to research published February 24 in JAMA Network Open.
Thyroid cancer overdiagnosis remained high despite accounting for a true increase in incidence in a modeling study led by David Francis, MD, from the University of Wisconsin in Madison, and colleagues.
“Our findings suggest that the detection of these cancers and their treatment yielded no benefit to population mortality,” the Francis team wrote.
Data from the Surveillance, Epidemiology, and End Results (SEER) database suggests that thyroid cancer incidence in the U.S. more than tripled between 1980 and 2016. This trend can be partly attributed to ultrasound detecting small, early-stage papillary thyroid cancer.
However, the researchers highlighted that no studies have quantified the magnitude of thyroid cancer overdiagnosis in the U.S. using data that account for current clinical practice and epidemiological patterns.
Francis and colleagues estimated U.S. population-level rates of papillary thyroid cancer (PTC) overdiagnosis in their modeling study. They also identified the implications of reducing ultrasound use for thyroid cancer incidence and overall mortality.
The team developed the Papillary Thyroid Carcinoma Microsimulation Model in 2024 and used it to examine contemporary papillary thyroid cancer incidence between 1991 and 2019. The simulation included all U.S. adults.
During the study period, the model estimated that between 72% and 94% of papillary thyroid cancer cases were overdiagnosed.
It also estimated that men had a slightly higher proportion of overdiagnosis compared with women, though women had a higher absolute rate of overdiagnosis.
Comparison of papillary thyroid cancer overdiagnosis among men, women during study period | ||
Measure | Men | Women |
| Proportion of overdiagnosis | 75% to 95% | 63% to 90% |
| Absolute rate of overdiagnosis (per 100,000 individuals) | 3 to 5 | 13 to 17 |
Finally, the team reported that reducing the use of thyroid ultrasound for nonpalpable nodules by 33% and 67%, respectively, would have decreased cancer incidence by 17% (from 18 to 15 per 100,000 individuals) and 41% (from 18 to 11 per 100,000 individuals) in 2019. This resulted in a less than 0.1% change in overall mortality, the group added.
The study authors wrote that the concept of overdiagnosis does not account for the need for practicing clinicians to “tolerate some degree of overdiagnosis.”
“For any given patient, the ultimate clinical trajectory cannot be known in advance, and thyroid cancers can substantially affect quality of life if allowed to grow unchecked,” they wrote. “Nevertheless, the rate of overdiagnosis estimated by our model was high enough to suggest that many more patients are receiving thyroid cancer diagnoses and undergoing surgeries than is necessary, considering the potential harms of diagnosis and surgery relative to the oncologic benefit.”
The researchers suggested that reducing ultrasound referrals could help drive down overdiagnosis rates, especially for women. However, they cautioned that the study results “should not be interpreted as guidance for the management of a specific thyroid nodule or patient.”
Less intervention and watchful observation may be an undervalued approach for clinicians, according to an accompanying editorial by Erik Alexander, MD, from Mass General Brigham in Boston, Massachusetts.
However, Alexander added that prospective, randomized trials comparing nonoperative monitoring with immediate surgical resection “are desperately needed and should be prioritized.”
“From such data, shared decisions will then be even better informed, and no doubt lead to a healthier population,” he wrote.
Read the full study here.