A thyroid ultrasound imaging database could spur the development of more effective diagnostic and treatment models for related diseases, according to research published January 23 in Ultrasound in Medicine & Biology.
A team led by Xiang Li from Northeastern University in Shenyang highlighted that its imaging database can make way for developing more accurate computer-aided detection (CAD) systems to analyze thyroid nodule-related lesions found on ultrasound. It also introduced a marker mask inpainting (MMI) method to erase artificial markers and improve image quality.
“This database collects a wide variety of nodule images, including different brightness levels, positions, numbers, and cuts, which is as consistent as possible with real-world application scenarios and helps to train more robust models,” the Li team wrote.
Ultrasound is a first-line method in the screening and diagnosing of thyroid nodules. It’s also used to guide fine-needle aspiration biopsy and subsequent treatment. However, it is physician-dependent, with clinicians having to contend with ultrasound’s low contrast, high noise, and the diverse appearance of nodules on imaging.
CAD methods have been implemented to aid radiologists, but the researchers noted that it can be difficult to obtain a high-quality and annotated thyroid data set. One reason is that radiologists place markers on images to outline where the lesions are to inform other clinicians. These markers can impact the performance of CAD models developed to assist radiologists.
To address these issues, Li and colleagues built their thyroid ultrasound imaging database. The database’s goal is to support CAD systems in accurate diagnosing and prognostic modeling of thyroid disorders. They also introduced an MMI method to erase artificial markers and improve image quality.
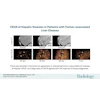
Here’s how the team did it: They collected thyroid ultrasound images and designed two modules in MMI, one for marker detection and the other for marker erasure. The detection module detects all markers in an image and stores them in a binary mask. From there, the erasure module erases the markers and generates an unmarked image.
The team noted that the database is annotated and statistically analyzed by physicians to ensure accuracy and consistency. Additionally, normal thyroid gland images and ancillary information on benign and malignant nodules are also provided for the database. For the detection module, the MMI achieved perfect accuracy in hitting the markers and an intersection over union of 98%. The erasure module meanwhile was tested on 1,017 images and achieved a structural similarity of 99.7%.
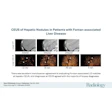
The researchers tested the database on 10 different segmentation models. They found that on unmarked data, the models achieved accuracies ranging from 45.7% to 90.3%. On reorganized data, the models achieved accuracies ranging from 23.3% to 84.7%.
Finally, on reorganized data with and without initial weights trained on unmarked data, the segmentation models achieved Dice coefficients ranging from 66.7 to 78.55.
The study authors that there is “still great room for improvement” in the available segmentation models. They also plan to use marked images to constrain the model, force it to discover essential nodule features, and automatically ignore artificial markers.
“We believe that these efforts can contribute to the future development of CAD systems for thyroid nodule disease,” the authors wrote. “In the future, we plan to integrate our algorithm with ultrasound equipment.”
The full study can be found here.