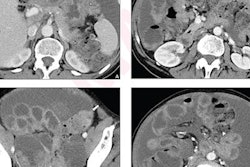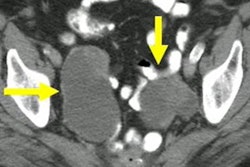
Ovarian cancer surveillance is a viable option for women with BRCA gene variants who delay removal of the fallopian tubes and ovaries, according to research published November 1 in the Journal of Medical Genetics.
A team led by Sue Philpott from the North Central London Cancer Alliance found that such surveillance, which uses a predictive algorithm that involves transvaginal ultrasound (TVUS), could be a suitable bridge for women in this subgroup who want to keep an eye on risk developments but also delay surgery. Some of the benefits the investigators noted included downstaging of ovarian cancer, higher complete cytoreduction rate, and cost savings.
"We feel that this form of surveillance can be offered to [women with the BRCA-heterozygote mutation] aged 35 years and older following informed consent, until they are prepared [to undergo removal of fallopian tubes and ovaries]," Philpott and co-authors wrote.
Previous studies have suggested that women with germline pathogenic variants in BRCA1 and BRCA2 genes account for between 9% and 18% of all epithelial ovarian cancers. They are at increased risk of developing cancer and are advised to undergo surgery to remove the fallopian tubes and ovaries, otherwise known as risk-reducing bilateral salpingo-oophorectomy (RRSO).
But many women delay or decline RRSO for a variety of reasons, prompting the need for ovarian cancer surveillance.
Philpott and colleagues explored whether such surveillance could demonstrate high sensitivity for asymptomatic disease and earlier-stage detection, as well as whether it could be cost-effective. For the study, they used Abcodia's Risk of Ovarian Cancer Algorithm (ROCA) test, a tool that calculates the probability of a woman having epithelial ovarian or fallopian tube cancer with an algorithm that analyzes the rate of change in tumor markers.
The study included 767 women. Of these, BRCA variant status was confirmed in 755 (99%), with BRCA1 variants in 339, BRCA2 in 410, and both in six. Eight ovarian cancers were identified, and out of these, two were occult at RRSO (both stage 1a) and six were screen-detected.
Philpott and colleagues assessed the sensitivity, specificity, and positive and negative predictive values of the surveillance regimen.
| Effectiveness of surveillance program for ovarian cancer in women with BRCA variants | |
| Sensitivity | 87.5% |
| Specificity | 99.9% |
| Positive predictive value | 75% |
| Negative predictive value | 99.9% |
The team also reported that the surveillance program improved women's quality of life and was cost-effective: The predicted number of quality-adjusted life years (QALY) gained by surveillance was 0.179, and its incremental cost-effectiveness ratio (ICER) was 102,496 pounds ($117,864) saved per QALY.
Although this form of surveillance is effective, the researchers cautioned that it should be seen as a short-term option only.
"Women undergoing such surveillance should be counseled extensively about its limitations, and that delaying RRSO indefinitely could result in diagnosis of an incurable ovarian cancer," they urged.
Disclosure: This project was funded by Abcodia and the North Central London Cancer Alliance.