An automated whole-breast ultrasound scanner isn't ready to replace conventional handheld ultrasonography as an adjunct to diagnostic mammography, according to a recent study by researchers at the University of Southern California (USC) in Los Angeles.
"As a concept, automated breast ultrasound is magnificent," lead author Dr. Linda Hovanessian Larsen told AuntMinnie.com. "But we found that the unit we used in the study is not ready for prime time yet at all. It is able to pick up some of cancers, but it's not yet comparable to a physician performing a handheld ultrasound exam."
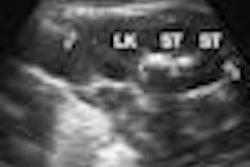
In a study Hovanessian Larsen presented at the 2008 RSNA meeting in Chicago, USC researchers used both techniques on 87 women presenting for breast ultrasound as part of their diagnostic imaging workup at the Los Angeles County and USC University Hospital. Each woman was imaged on a conventional ultrasound scanner with a handheld transducer (ATL 5000, Philips Healthcare, Andover, MA) and an automated breast ultrasound device (SomoVu, U-Systems, San Jose, CA). A total of 101 breasts were scanned using both systems.
One of three dedicated mammographers interpreted each automated study, along with the clinical history and mammography, while being blinded to the results of the handheld exam. Another of the three interpreters read the handheld exams with the clinical history and mammogram, but was blinded to the results of the automated exam. Hovanessian Larsen then compared results of the two techniques, noting any additional lesions discovered by either system. Lesions that were found only with automated breast US were re-evaluated with handheld US.
Of the 78 lesions seen on handheld US, 71 (91%) were also seen with the automated exam. Of the seven (9%) lesions seen only with handheld US, four were given a BI-RADS 4 rating and were biopsied. Pathology showed two high-risk and two benign lesions. Automated US identified 19 additional lesions not found with the handheld exam; 11 of those were given a BI-RADS 4 or 5 rating. Upon re-evaluation with handheld US, nine (81%) of these 11 lesions were not reproducible and two were biopsied and shown to be benign.
The BI-RADS assessment derived from mammography plus automated breast US was in agreement with the BI-RADS assessment derived from mammography plus handheld US in 70% of the lesions analyzed. Of the lesions seen with both systems, 8% were upgraded to a higher BI-RADS score based on the automated exam, with 80% of those requiring biopsy, while 11% were downgraded.
The study results demonstrate that it isn't yet feasible for automated breast US to replace handheld US in a diagnostic breast center, according to Hovanessian Larsen: automated breast US did not identify 9% of the lesions seen on handheld US, two of which were high-risk lesions, and nine of the 11 lesions seen only on automated US with a BI-RADS 4 or 5 rating were not reproducible on follow-up handheld US.
"The suspicious lesions the automated breast ultrasound system we used found that turned out not to be cancer were due to shadowing from Cooper's ligament," Hovanessian Larsen said.
By Kate Madden Yee
AuntMinnie.com staff writer
March 16, 2009
Related Reading
Ultrasound, MRI perform well in dense breasts, March 8, 2009
3D Doppler evaluation helps identify malignant breast lesions, November 6, 2008
Breast ultrasound CAD helps doctors find smaller lesions, October 10, 2008
Breast ultrasound CAD performance varies in ethnic populations
Screening US boosts cancer detection rate in high-risk women
Copyright © 2009 AuntMinnie.com