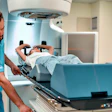
Hospitals and cancer treatment centers may want to offer the newest state-of-the-art technology, diagnostic imaging tests, and radiation therapy treatments to patients. But before they do, they must make sure they have the appropriate staff resources and detailed quality assurance programs in place.
Some do ... some don't. And for those that don't, the consequences to unwitting patients can be dire. That's the conclusion of an article published in the New York Times on January 27, the third story in a series on mistakes in radiology and radiation oncology by investigative reporter Walt Bogdanich.
Acknowledging that serious radiation errors are infrequent, and that new imaging and radiation therapy modalities are "undeniably successful" in their diagnostic and cancer treatment capabilities, Bogdanich wrote that "the technology introduces its own risks: it has created new avenues for error in software and operation, and those mistakes can be more difficult to detect. As a result, a single error that becomes embedded in a treatment plan can be repeated in multiple radiation sessions."
With rapid advances in technology, safety procedures become outdated rapidly. Quality assurance programs may not be comprehensive enough, and they may not be adhered to on a consistent basis due to a lack of appropriately trained clinical staff, lack of enough staff, lack or lapses of oversight, or a badly run department, according to the New York Times article.
Eight states, not identified in the article, do not require proof of any educational training or requirements to operate diagnostic imaging equipment, with the exception of mammography equipment. At least 16 states and the District of Columbia do not require licensing of medical physicists.
Most state and federal regulations overseeing the use of radiation for medicine, if they exist, lack strength, the story claimed. Reporting adverse events is the responsibility of the healthcare facility where the event occurred, which may or may not choose to report the incident. Due to the sophistication and complexity of the equipment, clinical specialists, such as radiologic technologists, radiation therapists, and medical physicists, may not even be aware that adverse events are occurring, Bogdanich reported.
As an example, the article referenced the recent radiation overdoses of patients receiving CT scans of the brain at Cedars-Sinai Medical Center in Los Angeles. It also noted that even hospitals seeking admission to participate in clinical trials make radiation dose errors.
In 2008, nearly 30% of these hospitals failed to accurately irradiate a head and neck phantom using intensity-modulated radiation therapy, according to Geoffrey Ibbott, Ph.D., director of the Radiological Physics Center in Houston, a federally financed testing service retained to conduct independent testing of clinical trial applicants.
Another set of tests conducted from 2000 to 2008 by the center found that 15% to 20% of hospitals using linear accelerators in clinical trials had at least one radiation beam outside the acceptable range.
Fragmented authority within both state and federal governments in the U.S. enables serious accidents to go unnoticed and undisciplined. The article references the case of a patient who was treated in 2004 for prostate cancer at Christus Spohn Hospital in Corpus Christi, TX. He received external-beam radiation therapy followed by prostate brachytherapy treatment. This combination represented a serious radiation overdose, resulting in major debilitating, acute toxicities, the story claimed.
The patient did not learn of his overdose until a year following treatment. The New York Times wrote that neither the state government agency overseeing radiology in Texas nor the U.S. Nuclear Regulatory Commission were aware of the incident until they were notified by the newspaper. In mid-January 2010, state radiology officials notified the New York Times that its investigation had identified no violations of state radiation regulations. The hospital settled privately with the patient.
The article, available at www.nytimes.com, was accompanied by two videos: one, a computer-graphics simulation showing the operation of a linear accelerator, and the second, the chronology of the death of a 40-year-old cancer patient from a massive radiation overdose, described in detail in the first article of the series.
By Cynthia E. Keen
AuntMinnie.com staff writer
January 29, 2010
Related Reading
NY Times article details radiation therapy errors, January 26, 2010
FDA finds new cases of CT radiation overexposure, December 7, 2009
NY Times story claims treatment errors at VA brachytherapy unit, June 23, 2009
Copyright © 2010 AuntMinnie.com