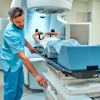
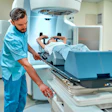
Given their proximity to the target tumor, why not make more use of these devices? That's the question being posed by researchers from the Dana-Farber Cancer Institute, Brigham and Women's Hospital, Harvard Medical School, and Northeastern University in Boston.
Their suggestion is to use the fiducials and spacers to deliver radiosensitizing drugs or cytotoxic agents in situ. Such a strategy could potentially increase treatment efficacy without increasing the radiation dose or subjecting patients to additional invasive procedures, according to an article published online in the International Journal of Radiation Oncology, Biology, Physics (October 30, 2009).
Biologically active drugs used in tandem with radiotherapy are typically delivered via intravenous injection. This approach is minimally invasive, well-established, and allows relatively uniform and predictable drug distribution. The downside to intravenous administration is the risk of toxicity to other organs, given the systemic nature of delivery.
One way of upping the drug dose safely is to inject the agent straight into the tumor. However, most radiosensitizers disperse rapidly, and will have left the tumor within a few days at the most. Courses of radiotherapy typically last several weeks, so patients would need repeated re-injections to maximize benefit from the combined drug/radiation treatment.
The alternative is to use drug-loaded implants that will release their therapeutic payload steadily and over a much longer period of time. Because this method is more invasive than injection, it may not be clinically acceptable. Such objections might be dropped, though, if the delivery devices were actually drug-coated radiotherapy markers already earmarked for insertion.
"The potential biological advantage of the in situ slow release of the radiosensitizer comes at no additional inconvenience to patients, and without substantial modification of current radiation therapy procedures," said senior author G. Mike Makrigiorgos, Ph.D., director of medical physics and biophysics in radiation oncology at the Dana-Farber Cancer Institute.
Feasibility study
The viability of this idea has now been assessed in a modeling study. Team members considered the drug distribution likely to be produced by dual-action fiducials and brachytherapy spacers placed in the lung and prostate, respectively. In each case, the position and number of the drug "eluters" simulated typical clinical scenarios and patient geometry.
A generalized approach was adopted to show how parameters such as drug diffusion, elimination, and eluter size would need to be varied to cover the target volume. In the lung, for example, researchers found that the efficacy of small drug-eluting fiducials would depend critically on the diffusion distance and retention time of the specific radiosensitizing agent used. These constraints were removed and tumor coverage increased when larger eluters were used.
The researchers also showed how, in the prostate, drug-eluting spacers could boost the dose to a target subvolume, while sparing adjacent critical structures. This technique may be preferable to dose-painting with radiation alone.
"This was a feasibility study to discover if we should pursue this avenue further. The findings provide guidance to the design of the drugs and carriers," said lead author Robert Cormack, Ph.D., medical physicist at the Dana-Farber Cancer Institute.
The next step will be to test the method in animal models, Makrigiorgos said. A series of drug-loaded fiducials has been developed for this purpose, in collaboration with nanomedicine experts at Northeastern University. Investigators will look at the time-release properties of these devices and their total drug capacity. The effect of variables such as tissue vascularity, dose rate, fraction size, and degree of fibrosis will also have to be considered prior to clinical implementation.
By Paula Gould
Medicalphysicsweb contributing editor
January 25, 2010
© IOP Publishing Limited. Republished with permission from medicalphysicsweb, a community Web site covering fundamental research and emerging technologies in medical imaging and radiation therapy.