MRI has revealed that consumption of ultra-processed foods (UPFs) is associated with higher amounts of intramuscular fat, potentially increasing the risk of knee osteoarthritis (OA), according to research published April 14 in Radiology.
In a study involving over 600 overweight patients at risk of developing knee osteoarthritis, researchers found that this association with ultra-processed food consumption and higher thigh muscle fat infiltration held regardless of factors such as calorie consumption, physical activity, or sociodemographic factors.
“This research underscores the vital role of nutrition in muscle quality in the context of knee osteoarthritis,” lead author Zehra Akkaya, MD, of the University of California, San Francisco, said in a statement from the RSNA. “Addressing obesity is a primary objective and frontline treatment for knee osteoarthritis, yet the findings from this research emphasize that dietary quality warrants greater attention, and weight loss regimens should take into account diet quality beyond caloric restriction and exercise.”
Although consumption of ultra-processed foods has been linked with greater knee pain, thinner knee cartilage as well as lower skeletal muscle mass and higher body fat percentage, the relationship between poor diet quality and skeletal muscle quality has been underexplored.
“Investigating this relationship in an early osteoarthritis or osteoarthritis-free but at-risk population is essential before exploring complex interactions in patients with established disease,” the authors wrote.
In their study, the researchers analyzed baseline data from 615 participants in the Osteoarthritis Initiative nationwide research study who were not yet affected by osteoarthritis. There were 275 men and 340 women in the study with an average age of 60. The patients had a mean body mass index (BMI) of 27 and an average of approximately 41% of the food they consumed over the prior year were ultra-processed.
“In addition to investigating the quality of our modern diet in relationship to thigh muscle composition, in this study, we used widely available, non-enhanced MRI, making our approach accessible and practical for routine clinical use and future studies,” Akkaya said.
Significant relationship
The researchers found that Goutallier grading on axial T1-weighted spin-echo thigh MRI exams were tied to diet quality, regardless of sex. They then performed linear regression analysis to adjust for sociodemographic factors, daily calorie consumption, smoking, physical activity, depression, and either BMI or abdominal circumference.
A statistically significant relationship was found between consumption of ultra-processed food and Goutallier grade for all muscles on both models adjusting for BMI (β = 0.108, p = 0.07) and models adjusting for abdominal circumference (β = 0.134, p = 0.001). These results indicated an increase in Goutallier grade of greater than 0.1 standard deviation (SD) for each 1-SD greater ultra-processed food proportion in the daily diet, according to the researchers.
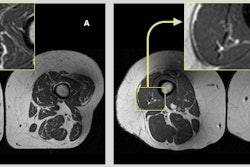
 Representative axial T1-weighted spin-echo thigh MRI scans in (A) a 61-year-old female participant and (B) a 62-year-old female participant. Both participants were of similar age and body mass index (BMI, calculated as weight in kilograms divided by height in meters squared). Both had Physical Activity Scale for the Elderly scores above the mean score in the study. According to the World Health Organization definition, the participant in B qualified as having abdominal obesity (abdominal circumference ≥ 88 cm). Abdominal circumference is a measure of central obesity that captures fat distribution and serves as an indicator of cardiometabolic health. Compared with the participant in A, the participant in B had a higher proportion of ultra-processed food (UPF) in their diet (87.1% vs 29.5%) and exhibited fattier thigh muscles bilaterally, with Goutallier grade (GG) for all thigh muscles summing to 25 for the participant in A and 38 for the participant in B.RSNA
Representative axial T1-weighted spin-echo thigh MRI scans in (A) a 61-year-old female participant and (B) a 62-year-old female participant. Both participants were of similar age and body mass index (BMI, calculated as weight in kilograms divided by height in meters squared). Both had Physical Activity Scale for the Elderly scores above the mean score in the study. According to the World Health Organization definition, the participant in B qualified as having abdominal obesity (abdominal circumference ≥ 88 cm). Abdominal circumference is a measure of central obesity that captures fat distribution and serves as an indicator of cardiometabolic health. Compared with the participant in A, the participant in B had a higher proportion of ultra-processed food (UPF) in their diet (87.1% vs 29.5%) and exhibited fattier thigh muscles bilaterally, with Goutallier grade (GG) for all thigh muscles summing to 25 for the participant in A and 38 for the participant in B.RSNA
“This is the first study assessing ultra-processed food’s impact on thigh muscle composition using MRI," Akkaya said. “By exploring how ultra-processed food consumption impacts muscle composition, this study provides valuable insights into dietary influences on muscle health.”
Compelling evidence
In an accompanying editorial, Miriam Bredella, MD, of NYU Langone Health, said that the research provides “compelling evidence that higher consumption of UPFs is associated with greater thigh muscle fat infiltration on MRI scans in adults at risk for knee osteoarthritis.”
“For radiologists, this work underscores the expanding field of identifying systemic health patterns that are embedded within musculoskeletal imaging studies,” Bredella wrote. “Abnormal muscle composition is not just a side effect of joint disease. It may be an early and potentially reversible sign of broader metabolic risk. As diet-related chronic diseases continue to rise, MRI may help reveal subtle tissue changes arising from modern eating habits, long before permanent joint damage occurs."
The full study and accompanying editorial can be found here and here.