Betanin (beetroot) and betanin-based contrast agents (BBCAs) show promise for use in contrast-enhanced abdominal MR imaging, a group of Turkish researchers has reported.
Gadolinium-based contrast agents (GBCAs) are commonly used with MR imaging, but concerns remain regarding gadolinium retention in tissue, adverse events -- especially in people with kidney disease -- and negative environmental impact, wrote a group led by Yelda Özsunar, MD, of Adnan Menderes University in Aydın, Turkey. The team noted that researchers have explored the development of GBCA substitutes, including those made from plant-based extracts. The findings were published November 4 in the Journal of Magnetic Resonance Imaging.
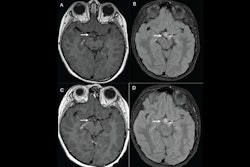
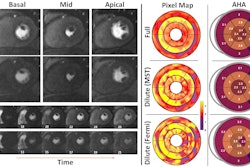
Özsunar and colleagues conducted a preclinical, experimental study that investigated the potential of Betanin and BBCAs as alternatives to GBCAs, assessing both their in vitro and in vivo performance when administered intravenously and abdominally and comparing performance to the GBCA gadobutrol. The study included in vitro tests on human and mouse fibroblast cells and in vivo tests on 15 male Wistar albino rats and two male New Zealand albino rabbits. The MRI protocol was 3-tesla field strength with spin echo and gradient echo sequences, and the group analyzed quantitative data with Microsoft Excel and GraphPad Prism 9.0.
The team characterized the Betanin and BBCA compounds via mass spectrometry, and assessed their safety by cytotoxicity, flow cytometry, histology, and blood biochemistry tests. They evaluated the BBCA's effect on the animals' organs after administering it orally, intraperitoneally, and intravenously.
The researchers reported the following:
- Betanin had greater molecular binding efficiency and therapeutic capability.
- BBCA was less toxic than gadobutrol.
- Both showed contrast enhancements in the gastrointestinal lumen as well as in parenchymal organs and in the vascular structure, with "lower toxicity and antioxidative benefits."
The study suggests that "Betanin and BBCA may be considered as viable options for contrast-enhanced abdominal MRI," the team concluded.
The complete work can be found here.