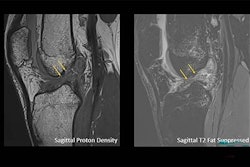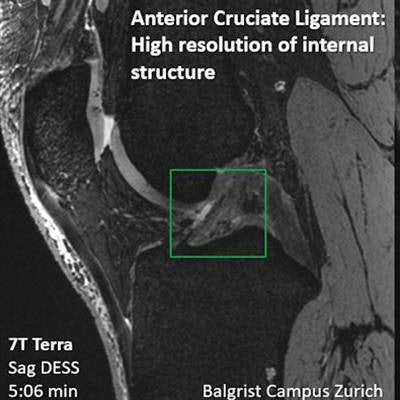
Lower field-strength MRI is adequate for most injured athletes, but some benefit from the higher spatial resolution 7-tesla MRI offers, according to a talk given May 15 at the International Society for Magnetic Resonance in Medicine (ISMRM) 2021 virtual annual meeting.
 Dr. Reto Sutter.
Dr. Reto Sutter.And although there are some technical challenges that come with using MRI at ultrahigh field strengths, these can be successfully addressed, presenter Dr. Reto Sutter of Balgrist University Hospital in Zürich, Switzerland, told session attendees. Sutter is chief of radiology at Balgrist and specializes in sports injuries of the musculoskeletal system and orthopedic and rheumatological imaging.
"7T MRI isn't easy 'out-of-the-box' imaging, but if you use the right protocol, it can be very effective for sports imaging," he said.
Sutter offered an overview of using 7-tesla MRI for musculoskeletal applications, as well as tips for optimizing images and an outline of clinical implementation directions the technology could take in the future.
7T and lower extremities
Radiology is on the verge of a new paradigm for musculoskeletal imaging with ultrahigh-resolution MRI, Sutter said. Standard MRI is currently used for meniscus injuries, but it can't necessarily distinguish individual components of the cartilage; 7-tesla MRI offers more detail.
"We want to have diagnostic imaging tools that are better than standard MRI and that can move us towards the resolution we obtain from histology," he said. "7T is a big step toward that goal, [since it can visualize] nicely the meniscus anatomy."
Possible uses for 7-tesla MRI in lower-extremity musculoskeletal imaging include the following, according to Sutter:
- Commonly missed meniscal tears, such as posterior horn, lateral, and displaced. "If we can develop 7-tesla technology to help us diagnose meniscal tears with higher accuracy, there's additional benefit for both referring physicians and patients," he said.
- Menscopopliteal fascicles. "To diagnose this, we need very good resolution," he said. "It's another possible use case for 7T."
- Cartilage delamination in the hip. Current best practice for visualizing this condition is direct MRI arthrography with traction, Sutter said. Using 7 tesla instead would benefit patients.
- Osteochondral defects in the ankle. "Standard MRI can nicely see bone marrow edema [in these cases] but there's limited spatial resolution," Sutter noted. "CT arthrogram shows surface of the cartilage overlaying defect, but soft tissue/edema isn't visible. 7T MRI has a possible benefit here with increased spatial resolution and also [visualization of] soft tissues."
Image optimization
Sutter offered tips for optimizing 7-tesla MRI images, including the following:
- T1-weighted nonfat-suppressed sequences for bone marrow imaging and fat-suppressed sequences for soft tissues.
- Matching bandwidth radiofrequency pulses to improve the geometric consistency of the 7-tesla image.
- Reducing chemical shift artifacts by matching increased bandwidth.
- Improving 7-tesla image homogeneity with software.
- Using a proton-density-weighted fat-suppressed turbo spin-echo protocol.
7T in the clinic
Finally, Sutter reviewed a number of possible clinical implementation directions for 7-tesla MRI, describing how it improved treatment planning in a 52-year-old woman involved in a skiing accident: 1.5-tesla MRI showed an anterior cruciate ligament (ACL) tear and a nondisplaced fracture of the tibial head, and she was referred for conservative treatment. However, 7-tesla MRI revealed a more complex tear and a meniscal ramp lesion, which directed her to surgery. In another case, 7-tesla MRI identified delamination of femoral cartilage in a 41-year-old male snowboarder that 1.5-tesla MRI missed.
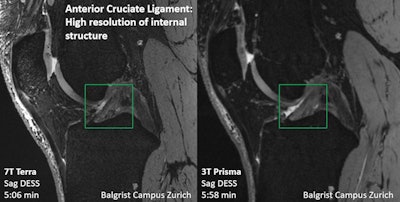 Direct comparison of the ACL with 7T and 3T. Image courtesy of Dr. Reto Sutter.
Direct comparison of the ACL with 7T and 3T. Image courtesy of Dr. Reto Sutter."[Studies have shown] that 7T MRI has higher diagnostic accuracy when it comes to visualizing low-grade meniscus and cartilage damage, and that [the technology] can be superior to 3T MRI for detecting small calcifications in articular cartilage and menisci," he said.
Not all athletes need 7-tesla MRI, but for those who could benefit from higher resolution images, it shows promise, according to Sutter. Yet implementation of the technology will take time.
"Our initial experience [implementing 7T MRI at Balgrist] has been challenging -- it's a marathon, rather than a sprint," he told AuntMinnie.com via email. "But the marathon is worthwhile, and I'm very positive about the future role of 7T MRI in sports imaging."