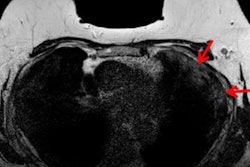
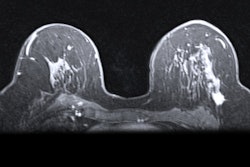
More women who are at high risk of developing breast cancer are getting regular screening with MRI. But a particular subpopulation -- those with BRCA mutations -- continue to be underscreened, according to a study published September 28 in the journal Cancer.
The results highlight a gap in screening efforts that must be addressed, wrote a team led by Karen Wernli, PhD, of Kaiser Permanente Washington Health Research Institute in Seattle.
"The steady and increasing rate of the use of screening breast MRI in women with BRCA mutations indicates improving adherence to [established] guidelines," the group wrote. "However, [our study shows that] nearly four out of five observed screening breast MRI examinations were performed in the two nonrecommended risk subgroups ... [and] screening breast MRI rates were found to be lowest in younger women compared with women aged 50 to 64 years with BRCA mutations, even though younger women may benefit the most from breast MRI."
Many professional organizations, including the American College of Radiology, recommend that women at high risk of breast cancer undergo regular breast cancer screening with MRI as a supplement to mammography. But whether these women are actually getting this adjunct screening remains unclear, Wernli and colleagues noted.
To investigate the issue, the researchers used claims data from a large U.S. insurer for 10 million women between the ages of 20 and 64 from 2006 to 2016 in order to calculate screening breast MRI rates. The group identified 25,617 women who underwent 37,447 screening breast MRI exams; these women were subcategorized by BRCA mutation status, family history of the disease, prior breast cancer history, and age.
The team found that over the study time frame, uptake of screening breast MRI increased, but not among all age groups of women with BRCA mutations.
| MRI use trends in women at higher risk for breast cancer | ||
| Rate per 10,000 women in 2006 | Rate per 10,000 women in 2016 | |
| Breast MRI screening | 2.9 | 12.1 |
| Breast MRI due to BRCA mutations | ||
| Overall | 210.8 | 1,562 |
| Ages 20-29 | 89.2 | 1,198.4 |
| Ages 30-39 | 175 | 1,519.1 |
| Ages 40-49 | 216.7 | 1,567.2 |
| Ages 50-64 | 256.7 | 1,669.6 |
| Breast MRI due to family history of breast cancer | 62.3 | 131 |
| Breast MRI due to history of breast cancer | 191.8 | 355.3 |
The study shows that referrals for breast MRI must be better matched to screening guidelines, according to Wernli's team.
"Clinical practice should continue to mitigate the use of breast MRI in women in whom it is not currently recommended due to breast cancer risk or subsequent cancer risk," the group wrote. "Furthermore, women with BRCA mutations remain underscreened, particularly younger women, thereby identifying a clear gap with which to enhance access to screening breast MRI."