Wednesday, November 30 | 10:50 a.m.-11:00 a.m. | SSK05-03 | Room S404CD
Regional lung perfusion imaging with noncontrast arterial spin labeling (ASL) at 3-tesla MRI is feasible and may provide new quantitative biomarkers for evaluating pulmonary vascular disease, according to this study from U.S. researchers.Dr. Christopher Maroules from UT Southwestern Medical Center in Dallas is scheduled to present results from a study that evaluated 10 healthy volunteers and 10 patients with pulmonary arterial hypertension.
The MRI protocol included 2D flow alternating inversion recovery with an extra radiofrequency pulse (2D ASL-FAIRER) along with 2D phase-contrast imaging of the pulmonary arteries to measure pulmonary artery flow. In addition, 10 subjects underwent a second 2D ASL-FAIRER scan to help determine reproducibility.
Two-dimensional ASL-FAIRER achieved high interobserver reproducibility and moderate test-retest reproducibility for regional lung perfusion. Maroules and colleagues also found good correlation between perfusion in the right lower lobe and pulmonary artery flow, but weaker correlation between perfusion in the right upper lobe and pulmonary artery flow.
In addition, the relative dispersion of lung perfusion was greater among patients with pulmonary arterial hypertension (1.25 ± 0.41), compared with the healthy volunteers (0.93 ± 0.32, p = 0.06), but the difference was deemed not statistically significant.
Noncontrast 2D ASL-FAIRER measurement of regional lung perfusion at 3 tesla is "feasible and demonstrates good reproducibility," the group concluded. "ASL-derived regional lung perfusion correlates with phase contrast pulmonary artery flow."



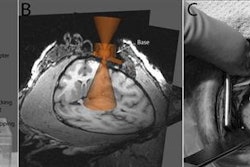
![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=100&q=70&w=100)






![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)








