A new MRI-based 3D software technique is able to capture and quantify changes to the prostate after focal laser ablation therapy, researchers reported April 18 in PLOS One. The software could provide better management of prostate cancer patients after laser ablation therapy.
Researchers from Case Western Reserve University in Cleveland used their MRI technique to capture laser-induced changes to prostate morphology in eight patients about eight months following treatment. The results revealed reductions in prostate volume, as well as changes in organ shape, primarily near the ablation site (PLOS One, April 18, 2016).
"We found that there are specific changes that take place in the prostate as captured on MRI following laser ablation," said Anant Madabhushi, PhD, in an interview with AuntMinnie.com.
Less invasive treatment
Focal laser ablation is a promising new prostate cancer treatment because it combines the ability to eradicate cancer cells with a precision that minimizes side effects, explained Madabhushi and co-authors Robert Toth, PhD, and Dr. Dan Sperling. Madabhushi is a professor and director of the Center for Computational Imaging and Personalized Diagnostics at Case Western.
 Anant Madabhushi, PhD, from Case Western Reserve University.
Anant Madabhushi, PhD, from Case Western Reserve University.Laser ablation causes thermal destruction of tissue. However, the technology is new enough that few studies have looked at the long-term effects of the prostate cancer treatment. There is no system to quantitatively evaluate the post-treatment effects on prostate morphology and structure via MRI, they wrote. Moreover, shape-based changes in the treated areas may be correlated with treatment efficacy.
Studying early treatment changes on imaging may help identify markers associated with longer-term prognosis.
"A quantitative method for systematically and quantitatively tracking treatment-related changes over time could potentially be used to predict longer-term outcomes," they wrote.
Their study sought to quantify changes in prostate volume post-treatment, as well as changes in patient alignment, changes due to surrounding organs, and changes due to the prostate cancer treatment itself. They developed a technique they call a finite element model (FEM) that uses physical parameters related to the amount of pressure the bladder exerts on the prostate and adjoining structures, Madabhushi said.
"We were able to gauge how much pressure adjoining structures induce on the prostate, so that gives us a measure -- not perfect, but a pretty good estimation -- of how much adjoining motion or deformation of the surrounding structures we're inducing," he said. "Using this estimation we were able to subtract out the approximate motional deformation due to the surrounding adjacent structures. That left us with changes that must have been exclusively due to the treatment procedure."
Understanding changes in gross volume, as well as localized treatment-induced morphology changes, will provide an understanding of how laser treatment affects gland morphology, shape, and size, according to the authors.
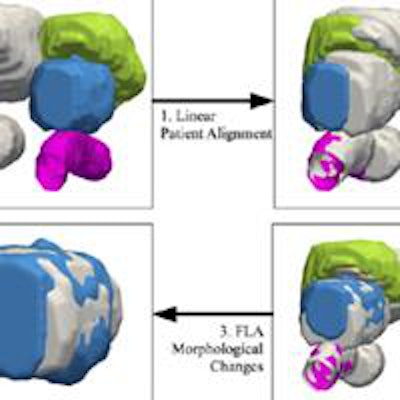
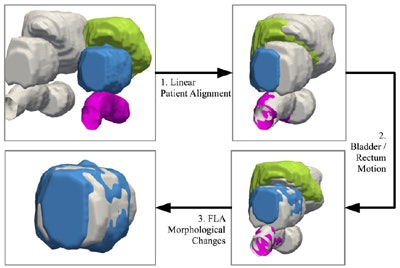 Overview of the registration techniques used in FEM. The post-treatment bladder, prostate, and rectum are shown in green, blue, and pink, respectively. Pretreatment surfaces are shown in gray. Quantitative measurements reflecting changes can be used to track treatment response over time. Image republished with permission of PLOS One, from Robert Toth, Dan Sperling, Anant Madabhushi: http://dx.doi.org/10.1371/journal.pone.0150016.
Overview of the registration techniques used in FEM. The post-treatment bladder, prostate, and rectum are shown in green, blue, and pink, respectively. Pretreatment surfaces are shown in gray. Quantitative measurements reflecting changes can be used to track treatment response over time. Image republished with permission of PLOS One, from Robert Toth, Dan Sperling, Anant Madabhushi: http://dx.doi.org/10.1371/journal.pone.0150016.Before and after
The study retrospectively examined eight prostate cancer patients scheduled for laser ablation, all of whom underwent T2-weighted MRI scans before and after the procedure. The time between MRI scans ranged from four to seven months.
T2-weighted MRI was acquired without an endorectal coil, at image sizes of approximately 140 x 140 x 140 mm, and voxel sizes ranging from 27 x 0.27 x 2.2 mm per voxel to 0.54 x 0.54 x 3.0 mm per voxel.
The FEM technique appeared to accurately assess the bladder and rectum deformations, the authors wrote. The results also suggest that laser treatment causes a decrease in prostate volume, which appears to manifest predominantly at the site of ablation.
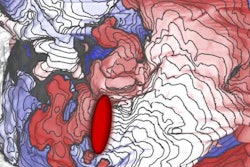
After aligning the images spatially, changes to MRI intensity values can be seen clearly at the ablation site.
"Our results suggest that our new methodology is able to capture and quantify the degree of laser-induced changes to the prostate," Madabhushi and colleagues wrote.
The quantitative measurements reflecting the deformation changes can potentially be used to track treatment response over time, they added.
How do changes affect outcomes?
What's next for the research? Clinical outcomes are one area.
"What is going to be very interesting in future work is to be looking at correlative associations between the changes in shape that the laser is causing to the subsequent outcomes," Madabhushi said. "Are the induced shape changes somehow contributing to better or worse outcomes?"
Because prostate cancers tend to be slow-growing or often indolent, definitive answers to that question will likely take several years, he said.
In related work, the study team compared prostate shapes in patients with cancer versus those without, and prostate shapes in patients who had a biochemical recurrence of cancer versus those who did not. This work revealed that there are statistically significant differences in the shapes of prostate capsules between these populations.
"I think that is a pretty good indicator that if there are differences in outcomes, the changes in shape might actually provide us with clues about the overall prognosis for the patient," Madabhushi said. "It's still very early days [for the discipline] so we don't have information. Prostate cancer by nature tends to be more indolent and less aggressive, so you need to look at a longer time frame in order to assess outcomes."