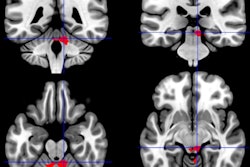
Using various MR imaging techniques, researchers have pinpointed structural abnormalities in the brains of people with chronic fatigue syndrome (CFS), which could potentially help in diagnosing the condition, according to a study published online October 29 in Radiology.
Researchers from Stanford University School of Medicine found abnormally high levels of fractional anisotropy in the right arcuate fasciculus in those with CFS compared to control subjects. The increase in fractional anisotropy also corresponded with the severity of CFS.
Given that correlation, fractional anisotropy, which measures water flow in the brain through diffusion-tensor MRI (DTI-MRI), could serve as a biomarker to track the disease. In addition, volumetric T1-weighted MRI found that CFS patients have slightly less overall white matter in the brain than control subjects (Radiology, October 29, 2014).
Challenging diagnosis
According to the U.S. Centers for Disease Control and Prevention, more than 1 million adults and children in the U.S. have CFS, which includes bouts of deep fatigue that can last as long as six months. Diagnosing CFS can be difficult because there is no definitive test to confirm the condition.
 Dr. Michael Zeineh from Stanford University.
Dr. Michael Zeineh from Stanford University."It is difficult for patients because they know something is wrong with them, but we can't find the culprit," lead author Dr. Michael Zeineh, assistant professor of radiology, told AuntMinnie.com. "Sometimes some treatments work, sometimes they don't, and we don't know why. It is a challenging disease on all fronts."
This study was the brainchild of Zeineh and Dr. Jose Montoya, an infectious disease and CFS specialist at Stanford. The trial was later expanded to include other specialists.
"One of the questions we had is: Can we see any abnormalities in the brains of patients with chronic fatigue syndrome? Until now, research has not found anything conclusive in brain MRI abnormalities," Zeineh said. "So we wanted to see if we would see anything interesting or different with an advanced study."
The research began in June 2011, with follow-up completed in November 2013. Fifteen patients who had experienced CFS for six months or longer -- defined as having at least four of the eight symptoms of the condition -- were matched with 14 control subjects according to age and gender.
All participants were imaged on one of two identical 3-tesla MRI scanners (GE Healthcare) using an eight-channel phased-array head coil and body-transmit coil.
MRI's contributions
The researchers utilized three MRI techniques to investigate potential brain abnormalities among the participants. Volumetric analysis was used to measure the size of different compartments of the brain, DTI assessed the integrity of the signal-carrying white-matter tracts of the brain, and arterial spin labeling (ASL) measured blood flow.
Of the three MRI techniques, volumetric analysis and DTI were the most helpful, Zeineh said.
"The volumetric analysis showed that all the white matter in the brain was smaller, on average, in chronic fatigue syndrome patients compared with age- and gender-matched control subjects," he said.
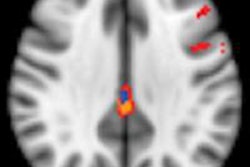
With DTI, Zeineh and colleagues found that two cortical regions -- the right middle temporal and precentral gyri -- connected with the arcuate fasciculus showed increased thickness. In addition, CFS patients with a more abnormal arcuate fasciculus experienced more fatigue.
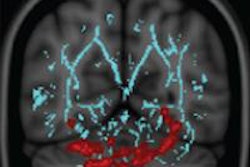
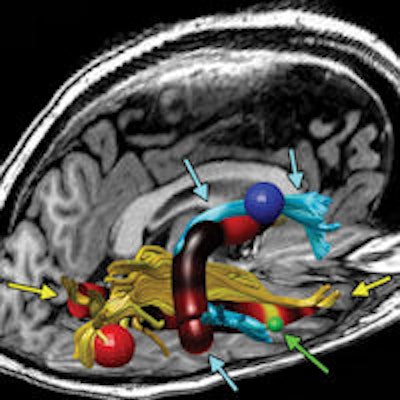
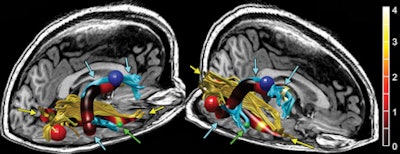 Reconstructed MR image shows the right arcuate (blue tracks and arrows) and inferior longitudinal fasciculus (ILF) (yellow tracks and arrows) in a representative subject. The track profile is colored according to fractional anisotropy, showing that the maximal increase in fractional anisotropy is in the anterior arcuate and ILF. The red, blue, and green spheres correspond to size and locations of increased cortical thickness in the right occipital, precentral, and middle temporal regions, respectively. The green arrows also point to the middle temporal region of increased thickness. Image courtesy of RSNA.
Reconstructed MR image shows the right arcuate (blue tracks and arrows) and inferior longitudinal fasciculus (ILF) (yellow tracks and arrows) in a representative subject. The track profile is colored according to fractional anisotropy, showing that the maximal increase in fractional anisotropy is in the anterior arcuate and ILF. The red, blue, and green spheres correspond to size and locations of increased cortical thickness in the right occipital, precentral, and middle temporal regions, respectively. The green arrows also point to the middle temporal region of increased thickness. Image courtesy of RSNA."Finding that the white-matter tract had abnormal fractional anisotropy and finding that those two end points of the tract had abnormal thickness suggest that something is going on in the right hemisphere [of the brain] in these chronic fatigue syndrome patients," Zeineh said.
ASL-MRI was less helpful, but it did confirm that there was no significant difference in perfusion in the cortex, supratentorial white matter, basal ganglia, thalami, or hippocampus, he said. The negative findings with ASL-MRI suggest that perfusion is not affected in CFS cases, the group concluded.
Causes and treatment
Zeineh said this was the first study to look at white-matter tracts in CFS patients and correlate them with cortical findings. Although the study included only 15 CFS patients, the technique shows promise as a diagnostic tool for identifying people with CFS. The findings need to be validated and explored in a larger study, he noted.
As for identifying possible causes of CFS or potential treatments, it is too soon to speculate on either topic, Zeineh said.
"It does motivate us to think about what to do for the next study to figure out what exactly this means ... and it can be helpful to look at patients across time and do a larger study to see if this could potentially be useful as a biomarker for fatigue," he added.
In fact, Zeineh and colleagues currently are designing "the next bigger study to explore and expand upon the findings in this study," he said.