Researchers have developed a perfluorocarbon (PFC) tracing agent and used it to track therapeutic cells injected into colon cancer patients with MRI, according to a new report in Magnetic Resonance in Medicine.
The study describes the first human tests of a PFC tracer with MRI to track therapeutic immune cells injected into patients with colorectal cancer. The authors hoped to assess the ability to detect labeled cells and monitor what happened to patients, the study team reported.
Cellular therapeutics is a promising new frontier for the treatment of serious diseases, but researchers lack a cell-imaging technique that can encompass a broad range of cell types and diseases, wrote Eric Ahrens, PhD, from the University of California, San Diego, and colleagues (Magn Reson Med, September 19, 2014).
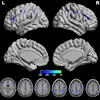
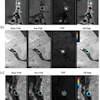
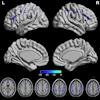
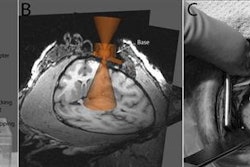
The PFC tracer was used to detect immunotherapeutic dendritic cells (DCs), which are potent immune stimulators. The DCs had been introduced in patients with stage IV metastatic colorectal cancer to stimulate an anticancer T-cell immune response. They were assessed with spin-density-weighted fluorine-19 (F-19) MRI on a 3-tesla scanner, which acquired images in 19 minutes.
MRI displayed the DCs as hot-spot images without a background. Dendritic cell numbers could be quantified in two patients from the F-19 hot spots and were found to decrease by about 50% at the injection site within 24 hours. Phantom studies previously showed that the limit for DC detection would be about 105 cells per voxel for this study, the authors reported.
Perhaps more important, the technology can be used to tag any cell type of interest, Ahrens said in a statement. The platform can be applied to wide range of diseases and applications, and it may speed development of important therapies, he added.
Noninvasive cell tracking can help lower regulatory barriers, according to Ahrens. Previously, it has been difficult to verify the survival and location of transplanted cells, and the high cost of treatment per patient has also slowed regulatory approval of new stem cell therapies. Tools such as these, which help glean better data, may require the use of fewer patients in a trial, reducing total costs.