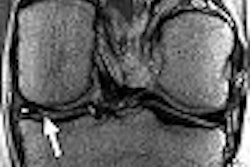
As breast cancer continues as a major health concern for women, MRI is playing an increasingly important role in detecting the disease in certain subgroups.
With many studies gauging the sensitivity of breast MRI in the range of 95%, the modality's rate of specificity, by comparison, is more moderate. The relatively lower specificity rate has given cause to some researchers to search for ways to enhance the technology's efficacy in the breast.
The "improvement of specificity is clinically relevant, because it could potentially reduce the number of unnecessary biopsies by increasing the positive predictive value of this MRI technique," said Dr. Maurice van den Bosch of Stanford University Medical Center in Stanford, CA.
Recent studies have found a correlation between increased ipsilateral breast vascularization and breast cancer. The issue is whether accurate assessment of breast vascularity can help increase specificity.
With that as a starting point, van den Bosch presented the results of a study on the use of high-resolution 3-tesla MRI with vascular mapping for detecting invasive breast cancer at the American Roentgen Ray Society (ARRS) annual meeting, held last week in Orlando, FL.
Improving specificity
The purpose of the study was to assess the diagnostic accuracy of contrast-enhanced breast MRI at 3 tesla, and to determine if the associated findings of increased ipsilateral breast vascularization would increase the overall sensitivity and specificity of the technique.
The scan protocol included fat-saturated T1-weighted high-resolution contrast-enhanced images to obtain maximum intensity projections (MIPs). The vascular scores ranged from S0 (no or low breast vascularity) to S3 (high breast vascularity).
In all, 56 lesions were included in the study, with a mean size of 12 mm, ranging in size from 3 mm to 45 mm. Pathology revealed 25 malignancies and 31 benign lesions. The breast malignancies were associated with increased ipsilateral breast vascularity.
Because researchers were looking to evaluate the positive predictive value (PPV) of vascularity scores, 23 BI-RADS 2 lesions were excluded, because all were benign. Of the remaining 33 lesions, 25 were malignant and eight were benign, resulting in a PPV of 76%. The vascularity score was positive in 24 lesions (of which 23 were malignant) and negative in nine lesions, of which two were malignant. The results showed an increased PPV of 96% and increased specificity of 88%.
Two false-negative recommendations occurred when MRI and the vascularity score were combined.
Clinical relevance
The results indicate that breast vascularity score can be an indicator of breast disease, but shouldn't be used alone as the definitive answer, according to van den Bosch.
"In accordance with previous studies, we found increased ipsilateral breast vascularity in malignant cases, and vascularity score did increase specificity to 88% and PPV to 96%," he said. "However, it did result in two false-negative recommendations. As a consequence, breast vascularity score, based on the preliminary results, cannot be used in clinical practice to replace biopsy."
But breast vascularity score can be powerful when used in combination with other established breast MRI methods for cancer detection. "Lesion morphology and enhancement kinetics, together with vascular mapping of the breast, ultimately improved the specificity of breast MR imaging to 86%, without affecting sensitivity, which was 100%," the study concluded.
Incidental lesions
In another ARRS presentation, a study from researchers at the University of Chicago Medical Center in Illinois sought to determine how often incidental lesions are detected by MR, how they can be characterized, and what is the proper management of the lesions.
"Because of the high sensitivity of breast MR, a considerable number of incidental lesions are detected by MR," said co-author Dr. Hiroyuki Abe, an assistant professor of radiology at the university. "For those incidental lesions, there are options to mark up, but the process is not always straightforward."
In the study, the researchers reviewed 1,304 consecutive breast MR studies performed at the medical center from July 1, 2003, through July 31, 2005. Lesions visualized on prior studies by way of mammography, ultrasound, and MR were excluded, as were palpable lesions.
The lesions were characterized according to the American College of Radiology (ACR) Lexicon. The 1.5-tesla MR protocol included an axial T2-weighted FSE and dynamic contrast study, including one pre- and four postcontrast, coronal T1-weighted spoiled gradient-recalled (SPGR) sequences.
Researchers found 252 unexpected enhancing mass lesions in 198 cases (15%) on the MR images. Sizes of the lesions ranged from 5 mm or less for 91 lesions, 6 to 10 mm in 111 lesions, and 11 mm to 20 mm in 43 lesions, while seven lesions were larger than 20 mm.
Second looks
Second-look ultrasound was performed on 214 lesions, and 124 (58%) were correlated successfully. "The majority of malignant lesions were found in second-look process," Abe said. "Most of the other malignant lesions were also found by using other criteria, such as lesion location and suspicious MR features."
Malignant lesions were found in the 19 cases with known cancer and six high-risk screening cases. Six cases were pathologically suspicious for breast primary cancer.
The location of the incidental lesions, relative to known cancer, also proved noteworthy. "Lesions found in the same quadrant of known cancer are likely malignant compared to a lesion in another quadrant," Abe noted.
Follow-up MR was performed in 56 cases in three to 24 months. In those cases, 21 lesions disappeared or had significantly decreased in size; eight lesions were normal parenchymal enhancement.
MR-enhancing mass lesions "should be worked up with ultrasound, as many of them can be correlated and better characterization is possible," the researchers concluded. MR-guided biopsy becomes an option if and when lesions are not sonographically correlated. The decision to use MR-guided biopsy also is dependent on MR findings and a patient's risk, they added, "because malignant lesions are likely to be detected in patients with known cancer and high-risk patients."
By Wayne Forrest
AuntMinnie.com staff writer
May 18, 2007
Related Reading
MRI useful for detecting cancer in contralateral breast, March 28, 2007
Spiral MRI technique picks up what mammo misses in DCIS, March 15, 2007
Breast pathology lacks standardization, particularly in DCIS, March 13, 2007
Breast MR shows exceptional sensitivity for spotting DCIS, January 12, 2007
Technology, guidelines cement role for breast MR in cancer screening, May 26, 2006
Copyright © 2007 AuntMinnie.com