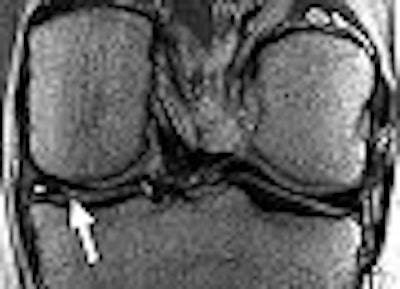
Knee MRI has become the most frequently ordered exam, but how accurate is it for diagnosing meniscal tears? Accurate enough to merit its acceptance in the orthopedic community, although MR interpretation must still be undertaken cautiously, according to a Belgian group that investigated the correlation between MR results and surgical findings.
For this retrospective study, radiologist Dr. Pieter Van Dyck and colleagues looked at 100 consecutive patients with clinical signs of internal knee joint derangement who underwent MR and arthroscopy. Findings from the latter served as the gold standard for the presence or absence of a meniscal tear.
Van Dyck is from the University Hospital Antwerp in Edegem. Other contributors are from the Antwerp department of orthopedics, as well as the radiology department at AZ St-Maarten in Duffel-Mechelen, all in Belgium.
Scanning was done on a 1.5-tesla scanner (Symphony, Siemens Medical Solutions, Erlangen, Germany) with a protocol that included axial turbo spin-echo (TSE) intermediate-weighted imaging with spectral fat saturation. MR images were first interpreted by Van Dyck, and all discrepancies were reviewed by co-authors Dr. Jan Gielen and Dr. Filip Vanhoenacker, both radiologists.
"Unavoidable errors were those in which the original MR diagnosis, with which all three observers agreed, did not agree with surgical findings," the group wrote (Archives of Orthopaedic and Trauma Surgery, April 14, 2007).
According to the results, of the 67 medial meniscal tears, 18% were missed. The accuracy of MRI for the medial meniscus was 88%. The sensitivity was 82%, specificity was 100%, positive predictive value (PPV) was 100%, and negative predictive value (NPV) was 73%. Out of 30 lateral meniscal tears, 40% were missed for an accuracy of 85%, sensitivity of 60%, specificity of 96%, PPV of 86%, and NPV of 85%.
Of the 27 total diagnostic errors made, 44% were deemed unavoidable and included 10 missed meniscal tears and three false-positive cases in which the menisci were considered torn on MRI but no tear was found on arthroscopy. Interpretation errors included four missed tears, one of which occurred when a stable tear was called a normal variant.
The authors stated that only 4% of the 67 medial meniscal tears could not be identified on MRI by all three reviewers. In contrast, 23% of lateral meniscal tears could not be identified, although the authors did not necessarily see this as a major problem. First, they pointed out that the high percentage of missed lateral meniscal tears were because of MR sequence limitations and not observer errors.
More important, confusion between fraying and tearing remains a common discrepancy between MR and surgical findings, they explained.
"(O)f 12 missed lateral tears, 11 (92%) should be considered as true or clinically significant meniscal tears and, thus, MR may be considered a highly accurate imaging method for detection of (lateral) meniscal tears," the authors wrote. "Whether meniscal fraying should be considered the cause of the patient's symptoms is controversial.... We recommend that radiologists ... be descriptive in reporting subtle MR findings, alerting the clinician of possible meniscal tear."
Rapid isotropic imaging
Van Dyck's group used FSE, which is the go-to MR sequence for evaluating internal derangements and meniscal tears. But as they mentioned, FSE MR does have technical limitations, including the lack of opportunity for reformation and structural blurring. Researchers from Stanford University and GE Healthcare have suggested using isotropic 3D FSE with an extended echo-train acquisition (XETA) instead.
"We have recently developed a fast-recovery 3D FSE method with (XETA) that uses variable flip angles to constrain T2 decay over a long echo train, allowing acquisition of T2-weighted images with minimal blurring," wrote Dr. Garry Gold and Dr. Christopher Beaulieu from the department of radiology at Stanford University in Stanford, CA. Their co-authors are from the university's department of electrical engineering and the GE Healthcare Global Applied Sciences Laboratory in Menlo Park, CA (American Journal of Roentgenology, May 2007, Vol. 188:5, pp. 1287-1293).
In their study, they compared this new sequence to 2D FSE MRI and 2D fast-recovery (FR) FSE MRI in the right knee of 10 healthy patients and one volunteer with knee pain, looking for differences in signal-to-noise ratio (SNR), contrast-to-noise-ratio (CNR), and accurate reformation of isotropic data.
Imaging was done on a 1.5-tesla scanner (Signa Excite HDx, GE Healthcare, Chalfont St. Giles, U.K.). Three-dimensional FSE XETA images were acquired in the coronal plane. In addition, the volunteer with knee pain underwent 3D FSE XETA MRI on a 3-tesla scanner.
"Partial Fourier acquisition and ARC (autocalibrating reconstruction for Cartesian sampling) parallel imaging reduced scanning time by a factor of 3.4, enabling an echo-train length of 78 to encode a 256 x 256 matrix for one section (slice encode) per shot. To cover the entire knee, 200 sections were acquired in just eight minutes," the authors explained.
 |
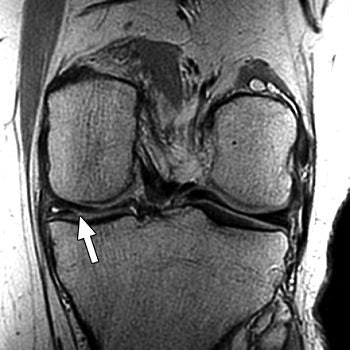 |
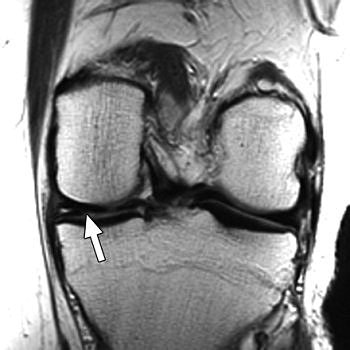
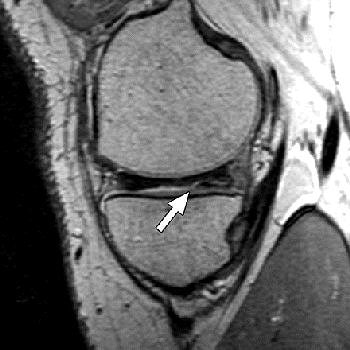
| Above, 27-year-old man with meniscal tear. Coronal 2D fast spin-echo (FSE) image (TR/TEeff, 4,000/38) shows tear (arrow). Middle, coronal 3D FSE extended echo-train acquisition (XETA) image (TR/TEeff, 2,500/38). Tear (arrow) was visible on two images of 2D FSE acquisition and 12 of coronal 3D FSE XETA images. Below, sagittal reformation of 3D FSE XETA dataset shows tear (arrow). |
 |
| Gold GE, Busse RF, Beehler C, Han E, Brau ACS, Beatty PJ, Beaulieu CF, "Isotropic MRI of the Knee with 3D Fast Spin-Echo Extended Echo-Train Acquisition (XETA): Initial Experience" (AJR 2007; 188:1287-1293). |
According to the results, cartilage, muscle, and fluid SNR were significantly higher with 3D FSE XETA MRI, in comparison to the other sequences. This was most likely due to the higher SNR that is inherent to 3D imaging and because of lower magnetization transfer effects in 2D imaging.
While fluid-cartilage CNR was higher for 2D FSE and 2D FR FSE MRI than for the experimental acquisition sequence, the authors pointed out that the ability to reformat may overcome this disadvantage.
Imaging at 3 tesla improved the resolution of 3D FSE XETA to 0.6-mm isotropic compared with 0.7-mm isotropic for 1.5-tesla images, the authors stated. In the volunteer with knee pain, 3D FSE XETA and 2D FSE revealed a meniscal tear in the posterior horn of the medial meniscus. Still, on the 3D FSE XETA, the tear was visible on a dozen images in the coronal plane versus two images from the 2D FSE acquisition.
Finally, the scan time for 3D FSE XETA MRI was longer than for the other two sequences, but again, the ability to reformat in multiple planes, should eliminate the need for multiple 2D acquisitions and reduce scan time.
"This study shows the potential for using 3D FSE XETA in normal volunteers," the group concluded. "Future studies are required to show the diagnostic accuracy of 3D FSE XETA compared with routine sequences for internal derangement."
By Shalmali Pal
AuntMinnie.com staff writer
May 16, 2007
Related Reading
Markers predict successful hyaluronan treatment for knee OA, January 25, 2007
From tears to TKA: The ins and outs of knee MRI, September 5, 2006
Four MRI signs diagnose radial meniscal tears preoperatively, December 23, 2005
Meniscal MRI studies highlight axial advantages, radial tear rates, August 28, 2004
Copyright © 2007 AuntMinnie.com




















