Dobutamine stress MR, a workhorse modality for diagnosing regional cardiac wall motion abnormalities, can evaluate treatment response in patients with idiopathic dilated cardiomyopathy (IDCM), according to a study from the Netherlands.
IDCM is congestive cardiac failure secondary to dilatation and ventricular dysfunction, but without a known cause for the myocardial dysfunction. The primary myocardial disease is characterized by "ventricular dilatation and inferior contractility," noted lead researcher Dr. Daniel Lubbers from University Hospital Groningen, adding that IDCM patients have normal cardiac angiograms.
"It has been hypothesized that chronic sympathetic activation may be deleterious in patients with dilated cardiomyopathy," he said in a presentation at the 2007 European Congress of Radiology (ECR) in Vienna. "We have seen in the literature that beta-blocker treatment has shown improvement in symptoms, exercise capacity, LV (left ventricular) function and perhaps even improved survival, although the reports on that issue are not uniform."
The identification of an effective treatment has led to a search for ways to evaluate the treatment response of beta-blockers beyond clinical measures, he said, and the researchers hypothesized that dobutamine cardiac MR (CMR) would be able to discern the differences in before and after images.
The study examined 11 patients (mean age 50 years) who were diagnosed with IDCM. Dobutamine stress CMR images were acquired both before the initiation of beta-blocker treatment and at least a year (mean 520 days) later, using a 1.5-tesla MRI scanner (Magnetom Sonata, Siemens Medical Solutions, Erlangen, Germany).
The researchers acquired short-axis cine and/or grid series "at rest and at increasing doses of dobutamine up to 30 mg/kg of body weight with a six-minute time interval, acquiring three short-axis views and one long-axis view" of the left ventricle, Lubbers said.
Images were graded in random order by a single observer who did not know if the image was part of the baseline or follow-up study. Evaluations were based on a motion score index "calculated in each of 17 segments on a four-point scale" Lubbers said. "A comparison was made between the wall motion score index at baseline and at follow-up using the Friedman test."
The inducible wall motion abnormality was defined as a new or worsening wall motion abnormality in at least two segments at consecutive levels.
Dobutamine stress CMR showed improvement between baseline and follow-up in seven of 11 (73%) patients. Two patients had complete remission of wall motion abnormalities.
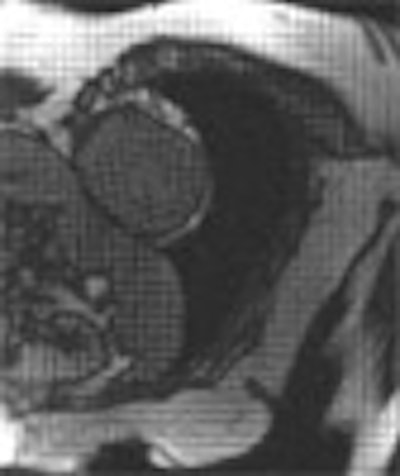
| Above: Baseline CMR cine image of a patient with idiopathic dilated cardiomyopathy (IDCM) depicts wall motion abnormalities, including ventricular dilatation and inferior contractility. Below: Following a year of beta-blocker therapy, CMR shows that normal wall motion is restored, corresponding to the patient's improved clinical presentation. Videos courtesy of Dr. Daniel Lubbers. |
| Having trouble viewing this clip? Click here to view full size clip or to change format. |
|
Having trouble viewing this clip? Click here to view full size clip or to change format. |
"Overall, you can say there was a significant improvement in the entire cohort between wall motion score index at baseline and the follow-up scan," Lubbers said. The wall motion score improvements corresponded to clinical improvements in most patients, "but we also saw two patients in which we could identify wall motion improvement but with a stable clinical response," he said.
"Changes in regional wall motion can be assessed with dobutamine stress cardiac MR in patients with idiopathic DCM after initiation of beta-blocker therapy, indicating that this (test) can be one of the objective measures we use in a larger prospective trial to identify the response to beta-blocker therapy," Lubbers said.
Some baseline studies have been completed since the March presentation, but the decision to move on to a larger trial has not yet been made, Lubbers told AuntMinnie.com by telephone this week. "If we are going to expand we are going to have to look at our protocol" to make sure it is optimized, he said.
By Eric Barnes
AuntMinnie.com staff writer
May 2, 2007
Related Reading
Myocardial viability after MI may be best assessed by 64-slice CT, March 15, 2007
MRI discriminates new myocardial infarction from old infarct scar, November 28, 2006
Stem cells reduce myocardial infarction size, November 21, 200606
Diabetics more likely to have silent myocardial ischemia, November 15, 2006
Coronary calcification linked to decreased coronary vasodilation, September 6, 2006
Copyright © 2007 AuntMinnie.com