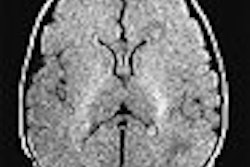
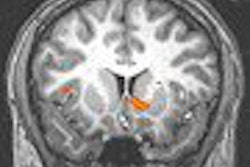
An intriguing new study from Stanford University pitted seven common diagnostic exams against each other to determine which test had the greatest impact on the management of subacute stroke patients. Diffusion-weighted MRI won out against a host of multimodality contenders in CT, ultrasound, and conventional MRI.
A noncontrast CT is usually the first exam for any acute stroke patient, since it can quickly detect hemorrhage that would preclude thrombolytic therapy. But for subacute patients -- those presenting three to six hours after onset -- the same scan is nearly worthless.
So which of the possible imaging options should be used at that point? A small but intriguing new study from Stanford University in California sought to answer this diagnostic dilemma, pitting seven imaging exams in a sort of free-for-all competition.
Over a 15-month period that ended in April 2003, a total of 171 subacute stroke patients each received seven consecutive exams at Stanford, generally in this order: non-contrast CT, conventional MRI using a T2-weighted FLAIR sequence, MR angiography, diffusion-weighted MR imaging (DWI), carotid ultrasound (CUS), transcranial Doppler ultrasound (TCD), and transesophageal echocardiography (TEE).
After each individual exam, clinicians recorded their diagnosis and their confidence in it. Those notes were then compiled and analyzed to determine the impact of each approach, according to Ralph Crisostomo, a Stanford medical student who presented the results at the 2004 American Association of Neurology meeting in San Francisco.
The clear winner among the imaging exams was DWI, which led clinicians to change their diagnoses in 14% of cases. Conventional MRI affected 10% of the diagnoses, MRA changed 6.7%, and TEE altered 4.7%.
The clinician's confidence in their diagnosis followed a similar pattern, with DWI boosting confidence levels in 42% of cases. Confidence was altered by conventional MRI, MRA and TEE in 25%, 18% and 14% of patients, respectively.
At the low end, CT altered just 1.8% of diagnoses, TCD changed 1.6%, and CUS influenced only 0.75%. These three exams also had less impact on clinician confidence, changing it in 7%, 5%, or 2% of cases, respectively.
Overall, DWI was significantly more useful than MRI, MRA, and TEE (p<0.001), and MRI, MRA, and TEE were significantly more useful than CT, CUS, or TCD (p<0.001).
"A strategy of early multimodal MRI in combination with TEE may be optimal for stroke assessment," the authors concluded in their abstract. Crisostomo noted that the research group's resulting protocol would recommend TEE imaging if even cardiac involvement is not suspected.
"The interesting thing is everyone does a CT and a carotid ultrasound -- they're easy to do and a lot of people do them at many institutions -- but if you have an MRI machine, you don't need to do them," said Crisostomo. "That's essentially what our results are concluding."
Emergency physicians have probably intuited the low yield of CT and CUS in subacute stroke from their own anecdotal experience. But will they feel uncomfortable skipping those exams?
It's a question that Crisostomo said he couldn't answer, as Stanford's emergency department had yet to be told about the study's findings.
By Tracie L. ThompsonAuntMinnie.com staff writer
May 17, 2004
Related Reading
Short MRI exam extends stroke tPA window, with good results, April 30, 2004
Active blood pressure lowering slows growth of brain lesion size after stroke, April 29, 2004
Carotid stenting safer than surgery for stroke prevention in diabetics, March 25, 2004
Transient ischemic attacks induce tolerance to stroke, March 15, 2004
FDG uptake may prove less stressful for pinpointing ischemia, March 9, 2004
Copyright © 2004 AuntMinnie.com