British researchers recommend FDG-PET over perfusion SPECT to diagnose and differentiate Alzheimer's disease from dementia with Lewy bodies after the hybrid modality proved its "significant superiority" in a study published online November 5 in the Journal of Nuclear Medicine.
FDG-PET achieved greater sensitivity and specificity than SPECT on visual diagnostic reads of the two modalities in a comparison of patients with Alzheimer's disease, patients with dementia with Lewy bodies, and healthy control subjects.
"Our findings therefore strongly support [FDG-PET's] incorporation in imaging diagnostic guidelines and as a biomarker of degeneration in newly proposed diagnostic criteria for Alzheimer's," the authors wrote.
The study was led by Dr. John T. O'Brien from the department of psychiatry at the University of Cambridge School of Clinical Medicine (JNM, November 5, 2014).
Direct comparisons
FDG-PET and perfusion SPECT both have been used to diagnose dementia, but the modalities provide different image characteristics and are tolerated differently by patients, according to the authors. FDG-PET measures brain metabolism and generates greater spatial resolution than SPECT, while SPECT provides an indirect measure of brain perfusion and metabolism at the time of contrast agent injection.
"Despite the widespread clinical availability of both perfusion SPECT and F-18 FDG PET, there remains uncertainty regarding their relative diagnostic accuracy in a clinical setting," O'Brien and colleagues wrote, adding that "direct comparisons to clearly establish superiority of one method have not been undertaken."
This prospective study enrolled patients older than 60 years with mild to moderate dementia, along with a group of healthy control subjects, between June 2010 and June 2012. There were 38 patients with Alzheimer's, 30 people with dementia with Lewy bodies, and 30 controls with no symptoms of dementia. The groups were well-matched in terms of age, gender, and duration of dementia (in the two noncontrol groups).
The researchers alternated the order of the FDG-PET and SPECT scans between consecutive subjects within each group. SPECT head scans (Symbia S, Siemens Healthcare) began 30 minutes after intravenous injection of 500 MBq of technetium-99m, while FDG-PET head imaging (Biograph TruePoint, Siemens) was performed over 10 minutes, commencing 30 minutes after intravenous administration of 250 MBq of FDG. Subjects also received detailed neuropsychiatric testing.
A clinical diagnosis of dementia was made by consensus between two experienced clinicians. Neither FDG-PET nor SPECT scans were used to confirm the dementia diagnosis.
The FDG-PET and SPECT results were rated visually by three medical physicists who were blinded to diagnoses and clinical information. The images were rated for quality in several areas of the brain associated with Alzheimer's and dementia with Lewy bodies.
The physicists assessed radiopharmaceutical uptake in the precuneus and lateral parietal lobes in the Alzheimer's patients and those with dementia with Lewy bodies, in addition to the posterior cingulate in patients with dementia with Lewy bodies.
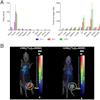
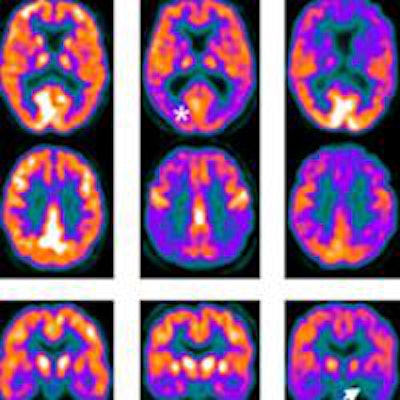
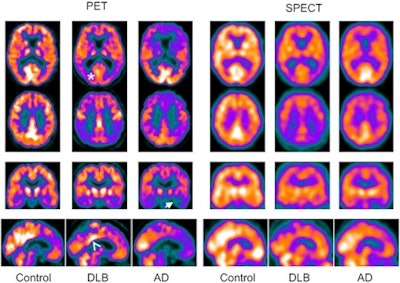 FDG-PET and SPECT scans for Alzheimer's disease (AD), dementia with Lewy bodies (DLB), and control subjects. The scans show medial temporal loss in Alzheimer's subjects (arrow) and occipital lobe reduction (asterisk) and posterior cingulate island sign (arrowhead) in DLB subjects. Image courtesy of JNM.
FDG-PET and SPECT scans for Alzheimer's disease (AD), dementia with Lewy bodies (DLB), and control subjects. The scans show medial temporal loss in Alzheimer's subjects (arrow) and occipital lobe reduction (asterisk) and posterior cingulate island sign (arrowhead) in DLB subjects. Image courtesy of JNM.In determining whether or not patients had dementia, FDG-PET achieved sensitivity of 85%, compared with 71% for SPECT. FDG-PET reached specificity of 90%, compared with 70% for SPECT.
Among the patients with dementia, the researchers examined the ability of FDG-PET and SEPCT to differentiate between Alzheimer's and Lewy body dementia. In this analysis, FDG-PET had 58 correct diagnoses, while SPECT had 48 correct diagnoses. FDG-PET showed 74% sensitivity for Alzheimer's, compared with 54% for SPECT. FDG-PET's specificity was 70%, compared with 67% for SPECT.
"There was a tendency for scan results correctly classified as dementia on F-18 FDG PET to be called normal on SPECT, and SPECT seemed to have better performance for dementia with Lewy bodies, with most Alzheimer's SPECT scans being rated unclear," the authors noted.
'Significant superiority'
The results show the "significant superiority" of FDG-PET over SPECT for differentiating patients with dementia from healthy controls, as well as for distinguishing Alzheimer's from Lewy body dementia, O'Brien and colleagues concluded.
"Our findings therefore strongly support [FDG-PET's] incorporation in imaging diagnostic guidelines and as a biomarker of degeneration in newly proposed diagnostic criteria for Alzheimer's," the authors wrote. "In contrast, the diagnostic accuracy of perfusion SPECT was significantly poorer."
They also mentioned several tangential factors, which, in some cases, could make SPECT a more practical option than FDG-PET for diagnosing dementia: SPECT may be more widely accessible to patients than FDG-PET, less expensive, and better tolerated.
"However, with the widespread use of F-18 FDG PET for oncology (responsible for more than 90% of F-18 FDG PET scans undertaken worldwide), costs of F-18 FDG PET have reduced considerably," they wrote.