Wednesday, December 3 | 11:30 a.m.-11:40 a.m. | SSK18-07 | Room S505AB
Researchers at Lucile Packard Children's Hospital and Stanford University School of Medicine have found a way to streamline FDG-PET/MRI scans to make them more tolerable for children with lymphoma and sarcoma.In pediatric patients, the maximum tolerated MRI time is typically around one hour, said lead author and visiting scholar Dr. Maryam Aghighi. The group's study shows that FDG-PET fused with breath-hold spoiled gradient-recalled echo (SPGR) sequences with ferumoxytol contrast enhancement provides comparable diagnostic accuracy to FDG-PET short-tau inversion recovery (STIR) sequences. The FDG-PET/SPGR scans allow for significant reductions in scan time, making the exam more patient-friendly.
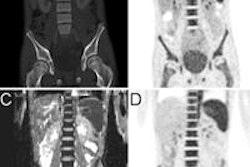
Aghighi and colleagues evaluated 31 children with malignant lymphoma and sarcoma who underwent a routine FDG-PET staging exam, followed by a ferumoxytol-enhanced whole-body MRI scan, using STIR and T1-weighted breath-hold SPGR sequences. FDG-PET images were then fused with STIR and SPGR results.
FDG-PET/SPGR detected 93% of malignant lesions at 2,077 anatomical regions, while FDG-PET/STIR detected 96% of malignant lesions. Sensitivity, specificity, and diagnostic accuracy of the two imaging techniques were all above 90% and within a few percentage points of each other, meaning there was no significant difference for staging pediatric lymphomas and sarcomas. FDG-PET/SPGR data were gathered with a "markedly accelerated" acquisition time compared with FDG-PET/STIR sequences.
"Our accelerated whole-body MR imaging protocol can be acquired in less than 30 minutes, which will help to combine local tumor staging and whole-body staging in one imaging session," Aghighi said.
Accurate staging of tumors in children and adolescents is critical to estimate prognosis and initiate appropriate treatment, she added. While FDG-PET/CT exams are the current staging procedure of choice for the majority of patients with malignant lymphomas and for some patients with sarcomas, they are associated with considerable radiation exposure.
"FDG-PET/MRI allows for whole-body staging of children with 80% reduced radiation exposure compared to CT scans," Aghighi said. "Therefore, FDG-PET/MR scans offer a compromise between the need for metabolic information and the need for reduced radiation exposure of pediatric patients."
Aghighi and colleagues plan to continue their research to compare the diagnostic value of integrated FDG-PET/MR imaging technologies with whole-body diffusion MRI techniques.