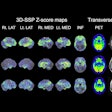
Initial findings from the ongoing National Oncologic PET Registry (NOPR) confirm that referring physicians often adjust their cancer treatment management based on PET imaging results.
The report, "The Impact of Position Emission Tomography on Expected Management of Patients with Cancer: Initial Results from the National Oncologic PET Registry (NOPR)," was presented at the 2007 RSNA meeting in Chicago by Dr. Bruce Hillner from the department of internal medicine at Virginia Commonwealth University in Richmond and Dr. R. Edward Coleman in the departments of radiology and nuclear medicine at Duke University Health System in North Carolina.
The conclusion comes from the latest details from the NOPR on how PET with F-18 fluorodeoxyglucose (F-18 FDG) often shifts a physician's intended management based on PET.
As of October 31, 2007, 1,629 PET facilities nationwide had participated in the NOPR, with some 67,135 patients registered. Of that total, 2,881 patients were deemed ineligible to participate. Data entry was completed on 54,553 patients. Approximately 92% of patients and 96% of referring physicians consented to research use of the data.
The report analyzed data for 16,292 PET studies. The total included cases in which both the patient and referring physicians consented to use of the data for research (86% of all cases). A nearly equal distribution of PET studies was obtained for cancer diagnosis, initial staging, restaging, suspected cancer recurrence, and treatment monitoring (ranging from 18% to 23%).
Treatment strategy
According to the findings, when intended cancer treatment management was classified as either treatment or nontreatment, physicians changed their management in 38% of cases after PET scans were conducted, the researchers noted in their RSNA presentation. The range was 31% to 46%, depending on indication. A change from nontreatment to treatment was much more common than vice versa -- 29.6% compared with 8.4%.
"If PET were not available, we asked them (physicians) what they would do if we broadly categorized choices as being nontreatment -- for example, watching and waiting, additional imaging, or biopsy -- versus initiating treatment," Hillner said. "The major finding is that much more commonly physicians moved from nontreatment to treatment three to four times as often as from treatment to nontreatment. The most common nontreatment was for watching and waiting. It provided sufficient diagnostic power to act."
In 39% of patients whose pre-PET plan was treatment, the post-PET plan had a change in therapeutic intent -- such as curative to palliative -- or to a nontreatment strategy. The NOPR also found that in patients switching from nontreatment to treatment after PET, the revised treatment goal was about equally divided between curative and palliative intent in cases of cancer diagnosis or initial staging.
In addition, in cases of restaging, suspected recurrence, or treatment monitoring, a palliative goal as 2 to 2.5 times more common. PET also was associated much more frequently (23.8%) with modifications in nontreatment plans than with minor (7.9%) or major (2.9%) alterations in treatment mode.
Complementary research
The data collected by the NOPR were also compared to studies in Europe and Australia, which reviewed physician treatment plans before and after PET imaging for common cancers that currently are approved for reimbursement coverage. The relative impact on changing management for relatively uncommon cancers and unapproved cancers was very similar in order of magnitude.
"A 30% to 40% association with a change in management was commonly seen across studies from other parts of the world," Hillner said. "In our study, it was the 30% [range], too, so it reinforces the message."
Additional details of the NOPR study to date have been accepted for publication in peer review literature. When it is published, Hillner said there will be ongoing discussions between the research team, PET advocates, and the U.S. Centers for Medicare and Medicaid Services (CMS) for consideration of revising CMS' "coverage position from one where payment is only available under the grounds of the registry to available with some codifications of specific clinical situations. How broadly that revision of Medicare guidance will be is to be determined."
Hillner declined to speculate what results may come from the discussions or what steps CMS may take in response to the NOPR.
Hillner said one important note to take from the project is to "make the distinction between when PET is valuable in the management of cancer care patients versus when should PET be done in relationship to other forms of imaging."
"This project does not address the question if PET should be used in lieu of other things or as a complement to other things. I think that is the key next generation of work," he said.
By Wayne Forrest
AuntMinnie.com staff writer
January 11, 2008
Related Reading
PET changes oncology management, study shows, July 19, 2007
NOPR opens, with modifications, May 9, 2006
ACR and ACRIN to launch PET registry in May, April 27, 2006
PET registry primed for takeoff, March 27, 2006
CMS, NOPR to collect PET data, February 10, 2006
Copyright © 2008 AuntMinnie.com