Using artificial intelligence (AI) to mine body composition from CT scans can help clinicians predict the risk of adverse patient outcomes such as cardiovascular disease or even bone fractures, according to a study published September 27 in Radiology.
The findings underscore just how useful CT data can be when it comes to assessing patient health, wrote a team of researchers led by Dr. Matthew Lee of the University of Wisconsin in Madison.
"Abdominal CT examinations are a mainstay of general and abdominal subspecialty radiology practice and are rich in body composition data, much of which go unused in routing clinical practice," the group noted. "Beyond population-based prediction, CT-based AI body composition tools measuring muscle attenuation, abdominal fat, and abdominal aortic calcium provide an interesting opportunity for more personalized cardiometabolic opportunistic screening, risk stratification, and prediction of adverse clinical outcomes."
Lee and colleagues explored population and sex-specific markers for muscle, abdominal fat, and abdominal aortic calcium measures on abdominal CT and analyzed how useful they were in predicting risk of death, adverse cardiovascular events, and bone fractures using AI algorithms.
Body composition measures for muscle, abdominal fat, and atherosclerosis "have particular prognostic value for risk of death and [poor] clinical outcomes such as future adverse cardiovascular events and fragility fractures in generally healthy asymptomatic patient populations and populations of patients with disease," the team explained.
AI-based tools can easily extract this CT data and produce information that may be more useful than that generated by other frameworks such as the Framingham risk score, the body mass index (BMI), or the Fracture Risk Assessment Tool (FRAX).
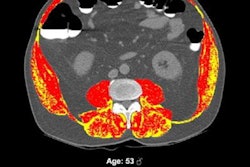
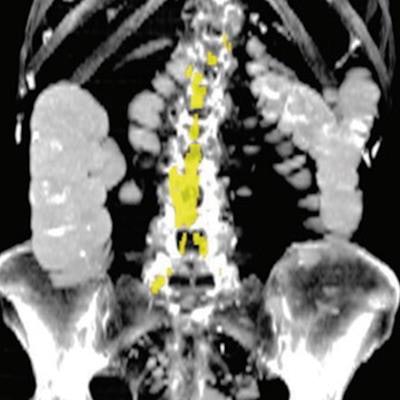
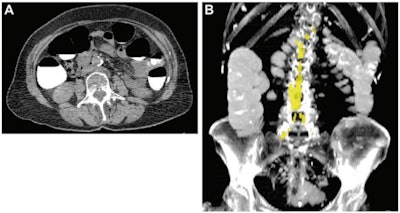 Abdominal aortic calcium in a 74-year-old woman who underwent CT colonography for colon cancer screening in 2008 and suffered a subsequent acute myocardial infarction one year later. (A) Axial noncontrast CT image at the L3 level. (B) Coronal maximum intensity projection CT image shows quantification of aortic calcium (yellow). The patient's aortic calcium Agatston score was 4137, while the 90% specificity threshold aortic calcium Agatston score was 735. Images and caption courtesy of the RSNA.
Abdominal aortic calcium in a 74-year-old woman who underwent CT colonography for colon cancer screening in 2008 and suffered a subsequent acute myocardial infarction one year later. (A) Axial noncontrast CT image at the L3 level. (B) Coronal maximum intensity projection CT image shows quantification of aortic calcium (yellow). The patient's aortic calcium Agatston score was 4137, while the 90% specificity threshold aortic calcium Agatston score was 735. Images and caption courtesy of the RSNA.Lee's group conducted a study that included 9,223 asymptomatic adults who underwent abdominal CT colonography as part of routine colon cancer screening between 2004 and 2016. The researchers used an automated deep learning and image processing algorithm that was developed, trained, and tested with muscle, abdominal fat, and atherosclerosis body composition data at the U.S. National Institutes of Health Clinical Center using information from another group of individuals, not Lee's study cohort.
Lee and colleagues used the AI algorithm to analyze CT data and segment and quantify abdominal muscle, visceral and subcutaneous fat, and aortic calcium, using a variety of tools to perform the following tasks:
- Deep-learning spine segmentation and labeling software was used to distinguish the last thoracic vertebra (T12) through the lowest lumbar vertebra (L5), and section and evaluate abdominal wall muscles and any aortic calcified atherosclerotic plaques.
- A U-Net neural network was used to identify and segment abdominal muscle at the L3 vertebra level, while feature-based image processing algorithms were used to segment and measure visceral and subcutaneous fat at that same vertebral level.
- A deep learning region-based convolutional neural network algorithm was used to section out abdominal aortic atherosclerotic calcification.
The researchers then reviewed follow-up results among the study cohort (mean follow-up time, nine years) and performed receiver operating characteristic (ROC) curve analysis to assess body composition measures and 10-year risk of adverse health outcomes such as death (549 patients), adverse cardiovascular events (1,831 patients), and fragility fractures (686 patients; of these 219 of these were hip fractures).
The authors found that muscle attenuation and aortic calcium levels were particularly strong body composition measures that were associated with these poor health outcomes among the study participants.
| Value of body composition markers on AI-aided CT for predicting risk of death among men and women | |||
| Marker | Specificity | Sensitivity | Area under the curve |
| Muscle attenuation (measured in Hounsfield units) -- men | 72% | 71% | 0.76 |
| Aortic calcium (measured in Agatston score) -- women | 70% | 70% | 0.74 |
The group found that using 23 Hounsfield units (HUs) of muscle attenuation for men and 13 HUs for women as the threshold for increased risk of death and fragility produced 90% specificity for these clinical outcomes.
For future risk of adverse cardiovascular events and/or death, using an Agatson score of 1,475 for men and 735 for women as the threshold produced a 90% specificity for these clinical outcomes. Agatson scores higher than 300 translate to moderate to severely increased risk.
The study further supports the benefits of mining CT images for a variety of data, according to the group.
"Fully-automated CT-based artificial intelligence body composition tools can be applied in routine abdominal CT to identify potentially important unsuspected or clinically silent 'presymptomatic' conditions that place patients at increased risk for death or other adverse clinical outcomes," the authors concluded.