Dual-energy CT (DECT) is an effective tool for improving neuroimaging in the emergency room -- and making use of it can translate into a variety of benefits for patients, according to a recent presentation.
The advantages of using DECT for emergency room brain imaging are legion, said presenter Dr. Aaron Sodickson, PhD, of Brigham and Women's Hospital and Harvard Medical School, both in Boston. Sodickson spoke at the recent International Society of Computed Tomography (ISCT) meeting in San Diego.
"How can DECT help us to better take care of our patients? Through better detection [and] characterization [of disease], ease of interpretation, [better] prognostication, and reductions in length of stay, imaging use, and radiation dose," he said.
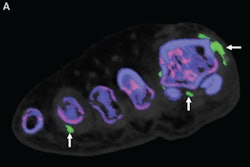
Dual-energy CT was introduced in 2006, and it can come in two forms, source-based or detector-based. Under the source-based DECT category are dual-source (two x-ray tubes), rapid tube voltage switching, split filter, and dual-spin devices, while detector-based CT may include dual-layer or photon-counting techniques. Over the years, the technology has shown promise for such indications as diagnosing hip prosthesis instability; gout workup; and assessing osteoporosis risk.
In his talk at ISCT 2022, Sodickson listed five ways DECT can improve patient care in the emergency department.
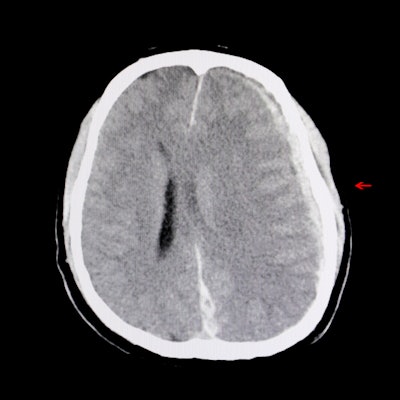
- Detection: "DECT identifies disease that may be otherwise invisible or challenging to see on conventional CT imaging," he said.
- Characterization: (for example, differentiating iodine staining from cerebral hemorrhage). "[The technique] provides additional information about material composition beyond traditional attenuation values, making it possible to further characterize findings without additional imaging," Sodickson said.
- Ease of interpretation: "DECT can make imaging easier to interpret, either by reducing interpretation time, or improving diagnostic confidence," he noted.
- Prognostication: "Dual-energy CT can provide prognostic information, particularly related to active hemorrhage," Sodickson explained.
- Reductions in length of stay, imaging use, and radiation dose: "DECT can reduce the need for follow-up imaging, particularly when differentiating intracranial calcification from potential hemorrhage," he said. "This can reduce emergency department length of stay, downstream imaging use, and associated radiation exposure."
"In addition to improving our accuracy, DECT improves reader confidence," Sodickson concluded. "[It helps] eliminate uncertainty ... [and] diagnostic certainty makes a real difference."