Sunday, November 26 | 12:05 p.m.-12:15 p.m. | SSA15-09 | Room S406B
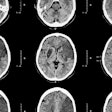
Integrating a temporal subtraction technique into CT scans improves the detection of sclerotic bone metastases in the spine, according to researchers from Japan."Although CT is a routine imaging modality to survey many types of cancer, bone metastases are often missed at CT because of their subtle findings," Dr. Takatoshi Aoki, PhD, told AuntMinnie.com.
As a means of accurately detecting as many sclerotic bone metastases in the spine as possible, the group developed a temporal subtraction method that reduces the number of artifacts on CT scans, according to Aoki, who is from the University of Occupational and Environmental Health School of Medicine.
The researchers applied their temporal subtraction technique to 20 CT scans in patients with sclerotic bone metastases and 20 CT scans in patients without metastases. Eight radiologists evaluated all of the CT scans both with and without temporal subtraction.
Aoki and colleagues found that the temporal subtraction method improved radiologists' accuracy in detecting sclerotic bone metastases to a statistically significant degree (p = 0.037). The method also increased average sensitivity by 11.8% and decreased average reading time by 15.9 seconds per scan (p = 0.004).
"The CT temporal subtraction method can sufficiently assist not only the radiologists' diagnostic accuracy but also their interpretation time for the detection of sclerotic bone metastasis in the thoracolumbar spine," Aoki said.















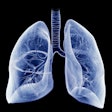

![Images show the pectoralis muscles of a healthy male individual who never smoked (age, 66 years; height, 178 cm; body mass index [BMI, calculated as weight in kilograms divided by height in meters squared], 28.4; number of cigarette pack-years, 0; forced expiratory volume in 1 second [FEV1], 97.6% predicted; FEV1: forced vital capacity [FVC] ratio, 0.71; pectoralis muscle area [PMA], 59.4 cm2; pectoralis muscle volume [PMV], 764 cm3) and a male individual with a smoking history and chronic obstructive pulmonary disorder (COPD) (age, 66 years; height, 178 cm; BMI, 27.5; number of cigarette pack-years, 43.2, FEV1, 48% predicted; FEV1:FVC, 0.56; PMA, 35 cm2; PMV, 480.8 cm3) from the Canadian Cohort Obstructive Lung Disease (i.e., CanCOLD) study. The CT image is shown in the axial plane. The PMV is automatically extracted using the developed deep learning model and overlayed onto the lungs for visual clarity.](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/03/genkin.25LqljVF0y.jpg?auto=format%2Ccompress&crop=focalpoint&fit=crop&h=112&q=70&w=112)