Dear AuntMinnie Member,
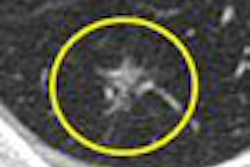
As CT slices get thinner, radiologists are encountering more and more ground-glass opacities (GGOs): hazy, granular-appearing lung nodules. What to make of them -- and which features increase the possibility that they are malignant -- is the subject of a feature article this week in our CT Digital Community.
As reported by staff writer Eric Barnes, ground-glass opacities have a variety of presentations, and while most are benign, others represent lung cancers. In a recent series of presentations in Europe, researchers examined different strategies for interpreting and managing GGOs.
A French group examined the frequency and growth rate of GGOs in a group of current and former smokers, and they also tracked suspicious regions that resolved over time. The group reported on which GGOs were more likely to be malignant, and discussed reading techniques that can help find them.
In other studies, a Korean group specifically looked at pure nodular GGOs that didn't disappear after six months. They found an age-based correlation between patients with pure nodular GGOs that were malignant and those that were benign.
Another Korean team discussed a five-year study that followed the clinical course of GGOs in patients who underwent thin-section CT screening for lung cancer. Their results offer guidance as to which types of GGOs might require short-term follow-up.
Get more details on this important clinical issue by clicking here, or visit our CT Digital Community at ct.auntminnie.com.