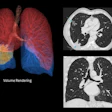
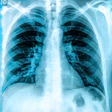
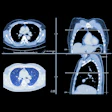
CT lung cancer screening may sound like a great idea, but the reality of nodule detection is nettlesome. The target population is huge, the scans are tedious to read, and screening studies can produce boatloads of suspicious nodules, all of which must be followed up in a systematic fashion.
Enter computer-aided detection (CAD). Pioneered for breast applications, CAD for chest CT is beginning to draw attention as a solution that could potentially make CT lung screening clinically and economically viable. Staff editor Eric Barnes delves into the topic in an article we’re featuring this week in our CT Digital Community.
Recent studies have produced intriguing results on the impact CAD can wield on the performance of radiologists reading CT lung exams. One group found that adding CAD as a backup to a radiologist increases sensitivity more than adding a second radiologist to double read the study. Sensitivity climbs even higher when the CAD system is allowed to produce more false positives.
Another study found that CAD’s impact was most dramatic on the performance of less-experienced readers -- these individuals saw their sensitivity ratings improve markedly, while reading times were simultaneously reduced.
The article also examines other recent advances in CAD software development, including a 3-D CAD algorithm that could represent an improvement over current 2-D techniques. Another group is pursuing the development of a nodule-matching scheme that could simplify the onerous task of nodule follow-up, automatically matching nodules in initial and follow-up studies to see if any have grown significantly.
Need more details? Just head to our CT Digital Community, at ct.auntminnie.com.