Photon-counting CT (PCCT) technology hit the clinical scene in 2021, when the U.S. Food and Drug Administration (FDA) cleared Siemens Healthineers Naeotom Alpha. Ever since, researchers have been investigating how to use the technology in clinical practice, and many studies have confirmed that it offers high-quality imaging at reduced contrast dose.
But since not every radiology department has a PCCT system, what can be done to reduce contrast dose anyway? There are some strategies, many of which aren't necessarily costly and can be implemented with relative ease.
AuntMinnie.com spoke to Mahmud Mossa-Basha, MD, chair of the department of radiology at the University of Alabama in Birmingham, regarding how departments can reduce CT contrast dose -- and why it's important to make the effort.
 Mahmud Mossa-Basha, MDUniversity of Alabama
Mahmud Mossa-Basha, MDUniversity of Alabama
Why reduce contrast dose?
The impetus to reduce contrast dose is multifactorial, Mossa-Basha said.
"One benefit of contrast dose reduction is reduced exposure to the patient, which lowers risk of kidney damage," he noted. "Other considerations are sustainability and financial efficiency. We want to reduce waste to mitigate environmental contamination and to save costs, and 'just' lowering patient contrast dose will not address these two issues."
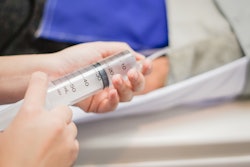
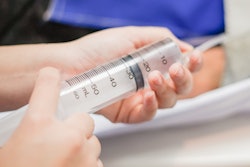
Mossa-Basha suggested that a key way to address the financial and sustainability concerns regarding contrast include right-sizing vials to the planned patient dose -- which requires carrying different sized vials and using syringeless contrast injectors. This tactic can be implemented no matter what kind of CT system a department has.
"The syringeless injectors allow for utilization of every mL of contrast for patient injection, thus reducing waste, cost, and environmental contamination," he said.
Techniques for conventional scanners
The most impactful change most departments can make is to switch from fixed-volume contrast protocols to weight-based dosing. Fixed-volume protocols -- typically 100–150 mL regardless of patient size -- were developed when the alternative was manual calculation, but it's been shown that body weight and lean body mass correlate more reliably with optimal contrast enhancement than a fixed volume protocol does.
Weight-based dosing combined with a low-kilovoltage technique further decreases radiation dose. At lower kVp settings -- 80 or 100 kV rather than the default 120 kV -- the imaging interaction with iodine increases, boosting iodine visibility without adding contrast volume. There is a tradeoff, however, in the form of increased image noise, which becomes more significant in larger patients.
"Weight-based protocols can be used to reduce contrast dose, and education on how to functionally perform this approach would be necessary to pursue this," Mossa-Basha said. He did concede that weight-based protocols "can be challenging for techs to implement, and in busy clinical CT environments, it might be best to use standard reduced dosing for specific types of exams."
Additionally, iterative reconstruction and AI-based denoising tools, which are now available on most scanners, help manage noise produced from lower kV and reduced contrast volumes. If a department is not routinely using these tools in conjunction with protocol optimization, that gap is worth closing before investing in anything else. Departments can assess their ten highest-volume contrast-enhanced protocols, tracking volumes, mapping against patient weight distributions, and identifying the most obvious over-dosing.
Techniques for dual energy or spectral CT
Virtual monoenergetic imaging at low keV settings -- typically 40 to 55 keV -- dramatically enhances iodine signal by exploiting the spectral properties of iodine near its K-edge. Studies using the "double low" technique -- low keV reconstruction combined with deep learning image reconstruction -- have shown contrast dose reductions of 30% or more while maintaining or improving image quality scores. If a department has dual-energy capability and is not using it to reduce contrast volumes, it's not taking advantage of the most accessible clinical and economic benefit of that technology, Mossa-Basha said.
"Dual-energy CT acquisitions can facilitate contrast dose reduction and is a functionality that should be leveraged further," he noted. "Monoenergetic low kEv maps can improve image contrast-to-noise, and when combined with AI denoising algorithms, the contrast dose can be further reduced or image quality further improved."
Supply chain disruption
In 2022, a CT contrast shortage forced protocol improvisation under pressure. Unfortunately, many radiology departments reverted to traditional protocols when supply normalized.
"What many of us discovered is for many exam protocols, lower contrast dose was sufficient, and some institutions maintained the lower contrast doses for particular exams," Mossa-Basha told AuntMinnie. "But others reverted to the original contrast dosing based on radiologist preference. I believe that iterative processes need to be further pursued to determine the lowest iodinated contrast dose that can be achieved while maintaining adequate image quality. I also believe that continuing to leverage AI to enable pathology visualization with lower contrast doses through denoising and also increased contrast conspicuity."







![Axial images from unenhanced calcium score cardiac CT (left) and curved planar reformation images from CT angiography (right) show that higher long-term exposure to air pollution is associated with greater coronary artery calcium and more obstructive coronary artery disease (CAD). Top row: Images in a 68-year-old male patient with higher 10-year mean ambient air pollution exposure (7.9 μg/m3 for particulate matter measuring ≤2.5 μm in diameter [PM2.5] and 17.4 parts per billion [ppb] for NO2) with extensive CAD (coronary artery calcium score [CACS] >1,000 and obstructive CAD [≥70% diameter stenosis]). Bottom row: Images in a 57-year-old female patient with lower 10-year mean ambient air pollution exposure (6.3 μg/m3 for PM2.5 and 4.6 ppb for NO2) with no CAD (CACS = 0 and no obstructive stenosis).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/06/hanneman.r6SMLzkezo.png?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)









