In 2018, a Colorado sonographer received a $1 million jury award in a lawsuit against her former employer. She claimed that she was fired after drawing attention to what she said were deficient cleaning procedures for ultrasound probes that put women undergoing transvaginal ultrasound scans at risk for infection.
It was hardly an isolated incident. The same year, a Pittsburgh hospital was hit with a class-action lawsuit after the facility notified patients that probes used in internal prostate, obstetrical, and gynecological exams had not been properly cleaned. Affected patients were offered free blood and urine testing to screen for healthcare-acquired infections.
The cases illustrate that even before the COVID-19 pandemic, infection control was a topic of growing importance in ultrasound, which has historically been known as one of the safest diagnostic imaging modalities. But poor infection control procedures can undermine the technology's otherwise stellar safety profile.
Fortunately, new technologies and growing awareness of proper infection control protocols can keep your patients safe -- and your hospital out of the headlines.
Cause for concern
Cases such as the ones in Colorado and Pittsburgh are certainly not the norm, but they are a cause for concern given how commonly ultrasound is used.
"Ultrasound is a safe diagnostic tool, and technology is rapidly advancing," Jocelyne Basseal, PhD, an Australian microbiologist and consultant on world health emergencies for the World Health Organization, told AuntMinnie.com. "As such, reprocessing of these medical devices has gained much attention over the past decade."
 Jocelyne Basseal, PhD.
Jocelyne Basseal, PhD.Transvaginal and transrectal ultrasound are among the riskiest types of scans, as inadequately cleaned probes could result in the transmission of human papillomavirus (HPV), which causes cervical cancer, and other sexually transmitted infections.
Any patient scanning procedure involving blood, body fluids, open wounds, or mucous membranes poses the highest risk if the equipment used has not been cleaned and disinfected, Basseal said. These procedures include internal ultrasound examinations, ultrasound-guided and interventional procedures, and biopsies, she noted.
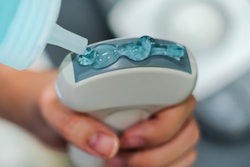
In addition to adequately cleaning probes, staff must ensure appropriate use of an ultrasound probe cover as well as ultrasound gel. In one recent study, the breakage rate for condoms ranged from 0.4% to 13%, while the breakage rate for commercial ultrasound probe covers ranged from 0% to 5% (Infection, Disease & Health, March 2020, Vol. 2, pp. 77-81).
 Breakage rates of probe covers and condoms have been analyzed in studies. Above, examples of breakages after ultrasound examinations. Image courtesy of Jocelyne Basseal and Infection, Disease & Health (Infect Dis Health, December 19, 2019, Vol. 19, pp. 30102-30106).
Breakage rates of probe covers and condoms have been analyzed in studies. Above, examples of breakages after ultrasound examinations. Image courtesy of Jocelyne Basseal and Infection, Disease & Health (Infect Dis Health, December 19, 2019, Vol. 19, pp. 30102-30106).Outbreaks caused by contaminated ultrasound gel on the manufacturers' end have also been reported. The U.S. Food and Drug Administration (FDA) and the Centers for Disease Control and Prevention (CDC) are currently investigating a multistate outbreak of Burkholderia cepacia infections after patients who underwent ultrasound-guided procedures developed bloodstream infections. The CDC reported that these bacteria were found in unopened ultrasound gel bottles.
Spaulding still leads the way
Dr. Earle Spaulding introduced disinfection protocols for reprocessing medical and surgical equipment more than 40 years ago, and those protocols are still at the core of infection control today. The Spaulding classification system breaks down equipment by risk level, with "critical" items presenting the greatest risk. Disinfection protocols are classified as low-, intermediate-, or high-level and are chosen according to the risk level of the procedure.
Low-level disinfection destroys most bacteria, some viruses, and some fungi. This level is appropriate for routine, noncritical ultrasound procedures performed with surface probes on intact skin. In contrast, high-level disinfection destroys all microorganisms except bacterial spores and is advised for probes scanning the inside of the body, for example during transvaginal and transrectal ultrasound.
| Risk associated with intended use | Spaulding classicifation | Disinfection/sterilization level required |
| Transducer contacts sterile tissues or a device (e.g., needle, catheter) inserted into sterile tissue during the procedure. | Critical | Cleaning followed by sterilization. If sterilization is not possible, then use high-level disinfection (HLD) and a sterile transducer cover and sterile gel. |
| Transducer contacts mucous membranes or nonintact skin or a device that contacts mucous membranes or nonintact skin during the procedure (i.e., no risk of contact with sterile tissues). | Semicritical | Cleaning followed by HLD. If not HLD compatible, disinfect to the highest level possible and use with a sterile transducer cover and sterile gel. |
| Transducer only contacts intact skin, or a device used during the procedure that contacts intact skin (i.e., no risk of contact with sterile tissues, mucous membranes, or nonintact skin). | Noncritical | Cleaning followed by low-level disinfection (LLD).‡ |
Source: The Society of Diagnostic Medical Sonography (SDMS) published guidelines for infection control in sonography in 2020. It incorporates Spaulding classification of equipment (critical, semicritical, and noncritical) and directs the appropriate type of disinfection. Image courtesy of SDMS.
But imaging facilities must do much more than follow the Spaulding guidelines to ensure their patients are safe. For example, they should provide training on how to clean and disinfect ultrasound probes and establish a traceability process for semicritical and critical procedures, Basseal said.
"It is also important for staff to work with machine manufacturers so approved products are used and instructions for use are followed," Basseal added. "Breaches in the cleaning and disinfection process will compromise patient safety."
Many different sets of guidelines on disinfection complement the Spaulding classification framework. The CDC published guidelines for disinfection and sterilization in healthcare facilities in 2008. The Society of Diagnostic Medical Sonography (SDMS) has also published ultrasound-specific guidelines.
 Jennifer Bagley.
Jennifer Bagley."It is really important when high level [disinfection] is indicated that we actually do high level," Jennifer Bagley, chair of the SDMS sonography disinfection and infection control task force, told AuntMinnie.com.
The American Institute of Ultrasound in Medicine (AIUM) has published guidelines and offers an accreditation program that includes assessment of infection control. The Joint Commission's audits of healthcare organizations also assess ultrasound infection control as part of accreditation and certification programs.
These various guidelines are fairly well-aligned, though there are some differences in the interpretation of the Spaulding classification, Bagley said. Ultimately, each facility has to come up with its own policies and procedures, using the available frameworks, said Bagley, who is also a professor of sonography at the University of Oklahoma.
Surveys flag noncompliance
Many surveys have shown there is a lot of room for improvement when it comes to procedures for disinfecting ultrasound transducers, including the following reports:
- A World Federation for Ultrasound in Medicine and Biology (WFUMB) survey found "a wide variance of understanding by respondents of the importance of adequate disinfection of ultrasound transducers and other equipment used to perform ultrasound examinations." Approved high-level disinfectants were not always used when indicated, and alcohol-based wipes were used by many respondents for cleaning endocavity transducers (Ultrasound in Medicine and Biology, February 2019, Vol. 45:2, pp. 344-352).
- A survey of U.S. healthcare facilities highlighted "extensive breaches of infection control guidelines" (American Journal of Infection Control, August 2018, Vol. 46, pp. 913-920).
- A large retrospective study conducted in Scotland linked low-level disinfection with poor outcomes. Among other findings, researchers reported that compared with controls, gynecology patients were at 41% greater risk of infection and at 26% greater risk of needing an antibiotic prescription in the 30 days after transvaginal ultrasound (Ultrasound, August 2018, Vol. 26:3, pp. 168-177).
- In a European Society of Radiology survey, only 14.7% of respondents reported using high-level disinfection for endocavity probes (Insights Into Imaging, December 2016, Vol. 7:6, pp. 841-847).
Factors behind noncompliance include lack of awareness of the risk for infection, lack of knowledge about disinfection, and lack of oversight by leadership.
 Raleigh White.
Raleigh White.Many U.S. facilities are not well-versed on best practices for ultrasound infection prevention and control, including understanding the Spaulding classification guidelines, commented Raleigh White, director of imaging services at the Hutchinson Regional Medical Center in Kansas. The Hutchinson facility has been proactive with developing its own rigorous protocols, with full support of hospital leadership.
Based on his experience giving presentations on infection control to hundreds in the sonography field, White said that leadership is often unaware of the infection risk associated with invasive procedures.
Sonographers are very conscientious, but providers may balk at the time and expense involved with high-level disinfection, Bob DeJong, retired technical manager of ultrasound at Johns Hopkins Hospital and now a consultant educator in ultrasound services, told AuntMinnie.com.
"Money is really a big concern with these products," DeJong said.
"To add to the challenges, specific disinfection products are validated for use on specific machines only, adding to the confusion on what product to use and how to use it," Basseal noted.
Risks for patients
What are the risks for patients? In some cases, it's pretty clear that a contaminated probe is the culprit behind a tragic outcome. The case of a patient in England who contracted hepatitis B and died after transesophageal echocardiography was widely reported.
 Dr. Jacques Abramowicz.
Dr. Jacques Abramowicz.But more often, cross-infection is difficult to study and difficult to prove, Dr. Jacques Abramowicz, president-elect of the WFUMB, explained to AuntMinnie.com.
"It's very difficult to show by numbers the risks of not following precautions," said Abramowicz, who is also director of ultrasound quality assurance at the University of Chicago.
Transmission of HPV via a contaminated probe might not cause cervical cancer until 20 years after an ultrasound scan, obscuring a bad outcome, Dr. C. Andrew Combs, a maternal-fetal medicine specialist at the Mednax National Medical Group, pointed out in conversation with AuntMinnie.com.
"Cervical cancer is common enough that no one would put two and two together," Combs said.
"People say, 'Well, do you have any evidence that this can happen?' " Combs explained. "We say, 'No, we don't, but do you have any evidence that it doesn't? Why would you do something that's intrinsically unsafe?' "
 Dr. C. Andrew Combs.
Dr. C. Andrew Combs.In September 2020, the Society for Maternal-Fetal Medicine (SMFM) published a statement warning of the risks associated with improperly disinfected transvaginal probes. Glutaraldehyde and ortho-phthalaldehyde are FDA-approved high-level disinfectants and are commonly used, but they have "virtually no efficacy against the human papillomavirus," Combs et al wrote in the SMFM statement.
According to the statement, providers should use "an agent with proven efficacy against the human papillomavirus, including hydrogen peroxide, hypochlorite, or peracetic acid," and they should not rely on sterile probe covers as these are prone to leakage.
Pushback on percutaneous procedures
For some procedures, however, debate remains about whether low-level disinfection is good enough. In February, the American College of Emergency Physicians, the AIUM, and three other medical associations published a position statement advocating for low-level disinfection of probes used to guide percutaneous sheathed procedures (Journal of Ultrasound in Medicine, February 2021, Vol. 40, pp. 895-897).
According to the statement, in some guidelines, disinfection protocols for endocavity transducers are being "misapplied to percutaneous and vascular-access applications."
"Recommendations for high-level disinfection of sheathed probes used for percutaneous procedures are not evidence-based and will result in unwarranted and unnecessary use of resources, increasing the possibility of safety events if percutaneous procedures are performed without ultrasound guidance," the associations maintained.
Furthermore, they called for greater disclosure of financial ties to manufacturers of ultrasound disinfection equipment.
Focusing more on ultrasound safety
Experts interviewed for this article said that much greater attention on ultrasound infection prevention and control in Joint Commission audits has been pushing facilities to be more mindful. The Patient Protection and Affordable Care Act has also heightened awareness; reimbursement may be withheld for patients who get healthcare-associated infections, Bagley noted.
Interviewees for this article also pointed out that infection prevention and control is actually very simple: Facilities need to follow guidelines, and then infection risk will be very low. Processes and procedures must be written down, and staff need to follow all the steps and not take any shortcuts, Bagley advised. Communication between the sonography lab and a hospital infection control department is also important, experts agreed.
One problem sonographers encounter is that their administrations and/or infection control departments do not understand how delicate and fragile ultrasound transducers are; they can be damaged easily in the cleaning and disinfecting processes if proper steps and agents are not used, Bagley explained.
"This kind of damage impacts transducer performance, image quality, and ultimately can impact the diagnostic outcome for the patient," Bagley warned. "Transducer repairs can be costly, especially when damage is caught late. Sometimes the damage is beyond repair, and the facility may have to buy a new transducer."
In 2017, the Hutchinson Regional Medical Center invested in an automated device that simplifies high-level disinfection of probes. The device takes about seven minutes to clean probes in a hydrogen peroxide mist solution, whereas previously, probes needed to be soaked for 20 minutes in a more caustic solution. The hydrogen peroxide solution is safer for technologists to be around and presents less risk for damaging expensive probes, commented Lindsay Turner, lead sonographer at Hutchinson Regional Medical Center.
There are pros and cons with each commercial option, and the choice of automated products depends on facility budget, resources, and time, Basseal said.
"The most important aspect is that staff are trained to use the technology properly -- whether it be concentration of solution and soaking time, wiping the probe properly, or checking indicator strips. All instructions must be followed as per the manufacturer recommendations," Basseal added.
COVID-19 raises awareness
The coronavirus has shone a bright light on infection control generally. During the COVID-19 pandemic, the Hutchinson center's practices for reprocessing probes stayed the same in that high-level or low-level disinfection was performed according to the Spaulding guidelines. SARS-CoV-2 is among the viruses that may be controlled with low-level disinfection.
However, the facility took many other new steps during the pandemic, including limiting scanning of nonemergent cases, disinfecting the entire ultrasound machine following scanning of COVID-19 patients, and donning personal protective equipment.
COVID-19 really brought to the forefront the need for ultrasound practices to include disinfecting equipment when scanning patients with infectious diseases more broadly, DeJong said. During the pandemic, staff really wanted to make sure they were following the guidelines of the CDC and their hospitals to avoid spreading the coronavirus, he noted.
The crisis underscored the importance of wiping down all of the equipment thoroughly and being mindful of areas touched by infected patients, as well as appropriately disinfecting the transducers.
"Medical imaging departments should prioritize basic infection prevention and control, and work with experts to identify gaps and ensure these have been addressed," Basseal said. "Infection prevention and control is important every time, for every patient -- not just during an outbreak."