The SARS-CoV-2 virus spreads primarily through respiratory droplets during close person-to-person contact. Given the close proximity of sonographers to patients during ultrasound exams, clinicians have had to implement special precautions, procedures, and protocols to ensure patient and personnel safety during the COVID-19 pandemic, while still providing the best patient care possible.
During the pandemic, ultrasound -- both point-of-care ultrasound (POCUS) and cart-based ultrasound -- has been widely used for diagnosing individuals suspected of having COVID-19. Clinicians have found that in addition to image quality which approaches that of stationary ultrasound scanners, POCUS and cart-based units are easy to transport to patients for scanning at bedside, which limits COVID-19 exposure.
 Dr. Jacques Abramowicz.
Dr. Jacques Abramowicz.Ultrasound has been useful during the pandemic in helping clinicians determine factors that contribute to respiratory failure in patients, often involving the cardiac and pulmonary systems. POCUS, particularly, has helped during the pandemic by offering clear signs of the way lungs are affected by COVID-19 and enabling emergency physicians to make a quick diagnosis, according to Dr. Jacques Abramowicz, president-elect of the World Federation for Ultrasound in Medicine and Biology, and professor and director of ultrasound quality assurance in the department of obstetrics and gynecology at the University of Chicago.
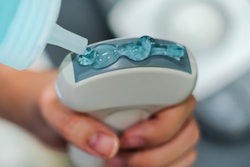
The virus has cast full light on some of ultrasound's major benefits, including its ease of disinfection and recent advances that have made the technology smaller, lighter, and more portable. But although ultrasound scanners are much easier to disinfect due to their small size than other imaging equipment, such as x-ray and CT systems, the unfamiliar nature of the pandemic means that many clinicians have been using ultrasound scanners without established guidelines that specifically address COVID-19. So there has been a need to establish clear protocols and training for using the modality in a health crisis, especially since operator skill can vary.
Putting protocols in place
As a result, many institutions and associations have created detailed guidance, protocols, and procedures to be applied when scanning COVID-19 patients or those suspected of having the virus. For example, Corinne Wessner, PhD, a research sonographer at Thomas Jefferson University, and colleagues published a step-by-step protocol developed at their institution for sonographers to use to prevent transmission of COVID-19 (Journal of Diagnostic Medical Sonography, September 17, 2020, Vol. 37:1, pp. 97-103).
The disinfecting and equipment management protocol explains the process involved in disinfecting ultrasound equipment when scanning patients who either are confirmed or suspected of having COVID-19. This protocol includes steps for disinfecting the equipment inside and outside the patient room. It also details the cleaning process for the equipment and transducer upon returning to the department, after the examination.
Additionally, the institution created distinct COVID-19 scanning protocols that were shortened to limit exposure to the sonographer and deliver images that answer precise clinical questions. Sonographers should only acquire specific clinical information needed for the appropriate treatment, the authors recommended.
In April, the American College of Emergency Physicians (ACEP) published several guidelines related to COVID-19:
- A guide to ultrasound transducer cleaning and disinfection
- Guidance specific to the disinfection of ultrasound transducers used for percutaneous procedures
- A general COVID-19 field guide covering work and home safety, personnel safety, triage, and ultrasound assessment, among other topics
In its publications, ACEP indicates when low-level disinfection (LLD) and high-level disinfection (HLD) should be used. When aerosolization or high-risk procedures occur, probes and machines should be covered, if possible, and disinfected with LLD after every use.
HLD is not required when using ultrasound probes on intact skin. There is no evidence that HLD offers benefits for disinfection from SARS-CoV-2. HLD is meant for cleaning instruments intended for contact with internal organs or mucous membranes, according to ACEP.
 Dr. Lori Mankowski Gettle.
Dr. Lori Mankowski Gettle.Additional guidelines on ultrasound infection control specific to COVID-19 were published in a recent paper in Ultrasound Quarterly by a team led by Dr. Lori Mankowski Gettle, chief of ultrasound in the division of abdominal imaging and intervention at the University of Wisconsin School of Medicine and Public Health.
Among the team's recommendations is to disinfect the machine, transducers, and cords after each use according to manufacturer and institutional guidelines, using approved cleaning solutions. The team noted that meticulous cleaning is required because the ultrasound gel can be easily caught in crevices or on a probe. Detailed instructions compliant with each institutional guideline should be distributed to all sonographers, according to Mankowski Gettle and colleagues (Ultrasound Q, September 2020, Vol. 36:3, pp. 200-205).
Working smarter and safer
The team put together a working group through the Society of Radiologists in Ultrasound to come up with general guidelines that could be useful in inpatient and outpatient settings.
"We tried to designate a single covered machine that would be used for the COVID-19 patients, which would be sanitized after each use," Mankowski Gettle told AuntMinnie.com. "We tried to be smarter about what you took in the room. You wouldn't take in any more probes than you needed. You wouldn't take in a bottle of ultrasound gel, instead just enough for the procedure, like a single-serving packet or a syringe. You would throw away all consumables. The objectives were to obtain images that answered the clinical question as quickly as possible and minimize exposure to sonographers and others," she explained.
Mankowski Gettle indicated that the pandemic challenged her hospital's sanitation practices.
"We wanted to make sure that our sonographers were protected and that they had the appropriate PPE [personal protective equipment]," she said.
Her institution never had any problems getting PPE, sanitizing solutions, or consumables.
"We also made sure that the sonographers were rotated because even bedside exams are challenging. So we wanted to make sure that no one sonographer was overtaxed and overexposed," she noted. "We checked with them periodically to make sure they were doing OK and that they weren't too overwhelmed because there was so much uncertainty at the time. They certainly were taxed to their limit."
To minimize exposure to COVID-19 among sonographers, Mankowski Gettle advises radiology departments to be certain of the following before beginning an exam:
- Ultrasound is the proper modality for answering the clinical question.
- The proper exam is being undertaken.
- The ultrasound was not done previously.
- Another study was not done previously which already answered the clinical question.
"You want to be sure that you're doing the right study at the right time for the right patient," she added.
Importance of portable ultrasound
Using portable ultrasound systems to scan patients at their bedside, without having to transport them to scanning rooms, was extremely helpful in minimizing exposure of the department to COVID-19, Mankowski Gettle noted. The portable systems also helped staff avoid closing the scanning rooms to sanitize them, which would take the rooms out of operation for a while.
Another advantage of ultrasound is how much easier the scanners are to clean than other equipment due to their smaller surface area, noted Mankowski Gettle and others interviewed.
"We use a probe cover when scanning COVID-19 patients and remove that before leaving the room. We perform low-level disinfection [on equipment] before we leave the floor, and high-level disinfection when we return to the department," Mankowski Gettle explained.
Abramowicz concurred on the simplicity of cleaning ultrasound equipment.
"These machines are essentially like tablets, easy to clean with wipes. The probes can be cleaned also with wipes since the vast majority of, if not all, point-of-care ultrasound [equipment] is external, which means no critical instruments," he noted.
Bedside ultrasound has also been important during the pandemic in helping healthcare providers make diagnoses, in some cases before results from polymerase chain reaction (PCR) tests were available, according to Dr. David Evans, chair of the division of clinical ultrasound and medical director of point-of-care ultrasound at Virginia Commonwealth University School of Medicine.
 Dr. David Evans.
Dr. David Evans."Obviously, this type of ultrasound has been invaluable during the current pandemic. When someone presented with undifferentiated shortness of breath, ultrasound was extremely valuable for evaluating this viral illness at bedside," Evans told AuntMinnie.com. "Before we'd get the PCR test results for COVID, from ultrasound images at bedside we noticed indications that were very specific to viral pneumonia."
Evans said their physicians adopted the same kind of diagnostic algorithm used in other centers, in which a quick evaluation with ultrasound would be performed in patients under investigation for COVID-19. Then the patient's heart would be examined.
"This would help guide our actions as to whether this was indeed what we thought was COVID and how much of the lung was actually affected," Evans added.
Modifying protocols
Evans says Virginia Commonwealth University modified its disinfection protocols after the pandemic hit, developing new protocols that covered equipment sanitation, including the cords and transducers, and using consumables only once.
"When getting ready to scan a patient, you'd take the cover off the ultrasound machine and wipe down the entire machine with gloves on. Then you would gown up, you'd have your N95 mask on, and your eye protection on," he explained.
Sonographers would then enter the room with the ultrasound machine, perform the exam, wipe it completely down in the room with the patient, and pull it out of the room. They would then remove their gown, gloves, masks, and eye protection; sanitize eye protection; put on new gloves; wipe the whole machine again; and put it back under a storage bag for its next use.
"We did not separate which machines would be used solely on COVID-19 patients and which would be used on non-COVID patients," he said. "We did separate the hospital into hot, warm, and cold zones. Most of the equipment was either in the warm zone or hot zone. There're 143 pieces of [ultrasound] equipment in the enterprise."
But a significant issue that presented a risk to sonographers was the fact that some COVID-19 patients would try to remove their facial coverings because they had difficulty breathing, placing sonographers at significant risk of contracting the virus, according to Evans.
"For this reason, we tried to be very cognizant of when it was necessary to bring in sonographers. We tried to be sparing of their contact with these extremely high-risk patients. We had to make sure that the studies were absolutely necessary at that time," he noted.
Evans is not aware of any sonographers becoming ill with the coronavirus because of their contact with ill patients. His institution did not have issues with getting enough PPE and used cloth gowns as well.
Evans says it is important to address the challenges presented by the COVID-19 pandemic on an institution-wide basis, with each department working closely with other departments to develop hospital-wide protocols, rather than having each department develop protocols independently.
Growing in utility
Physicians at Columbia University -- one of the epicenters for the first wave of the pandemic in New York City -- now know a lot more about the utility of ultrasound for COVID-19, according to Dr. Penelope Lema, vice chair of faculty affairs and director of the emergency ultrasound division at the university, which operates four emergency departments within the New York-Presbyterian hospital system.
 Dr. Penelope Lema.
Dr. Penelope Lema."It was unclear at the start of the pandemic because we did not know enough about COVID, and we were rapidly learning how to integrate ultrasound as well," Lema told AuntMinnie.com. "As we better understood COVID, and as COVID started mutating, we found ultrasound was useful to identify infections of the lung, but it was even more helpful to diagnose those who had cardiac involvement with COVID."
Ultrasound was helpful in differentiating which organ systems might be infected with COVID-19, Lema indicated -- not just the lungs, but particularly cardiac manifestations.
"COVID can affect the brain, the heart, the lungs, and other organs. We saw that it was affecting the gastrointestinal system or skin in some children who were diagnosed with MIS-C [multisystem inflammatory syndrome in children]. COVID is not discriminatory," she added. "Ultrasound helped us identify myocarditis, heart failure, and pulmonary emboli because some patients had variable presentations of the inflammatory response due to COVID."
During the height of the pandemic in New York City last year, ACEP published recommendations in its COVID-19 field guide that suggested providers remove all nonessential equipment and extraneous items from cart-based ultrasound machines due to possible contamination from aerosolized droplets. If a transducer touched a COVID-19 patient, LLD of the transducers was recommended.
"We removed any extra bags and storage devices off the cart-based machines and made sure everything was protected so that there wouldn't be any cross-contamination," Lema said. "As we all became more familiar with COVID, exposure to aerosolized droplets from a patient with COVID-19 was the primary concern for transmission."
Within the emergency departments of Columbia University Irving Medical Center, all patients are currently required to wear masks, and all staff must wear masks and show proof of vaccination, unless they have a medical or religious reason not to, according to Lema.
"We have always been provided with personal protective equipment when working in the emergency departments and wear goggles, hats, masks, gowns, and gloves. In addition, some physicians have their own postwork rituals when they go home to decrease the possible risk of transmission to their families," she said. "We offer access to hospital showers for our faculty after their shifts."
As with others interviewed for this article, Lema confirmed the value of ultrasound at the bedside.
"Any time you place a patient with active COVID infection in a CT suite for imaging, the entire room becomes contaminated for patients," she said. "By using ultrasound, either the cart-based or a handheld system, we could image patients at the bedside in negative pressure tents or isolation rooms, which would limit cross-contamination."
Self-tracking
Dr. Yale Tung Chen, currently a physician of internal medicine at Hospital Universitario Puerta de Hierro Majadahonda, in Madrid, was an emergency medicine physician at La Paz University Hospital in Madrid when the pandemic first struck. He contracted COVID-19 while caring for patients and used POCUS to help track his condition. Chen indicated he may have come down with the virus in his workplace.
 Dr. Yale Tung Chen.
Dr. Yale Tung Chen.After he received PCR test results that indicated he was infected with COVID-19, Chen used POCUS to find his lungs involved with the virus, as indicated by bilateral B-lines on ultrasound images, which is the typical sign for interstitial COVID-19 pneumonia. Continuing to use ultrasound, he was able to track his recovery, which took about two weeks, although there were lingering symptoms of weakness and headaches, he noted.
"Lung ultrasound was really useful for diagnosing my COVID-19 and for follow-up," he told AuntMinnie.com.
Initially, La Paz University Hospital used ultrasound to triage patients coming to the emergency department, but it later used ultrasound to help confirm any suspicions of COVID-19, explained Chen. The hospital put in place a detailed sanitation protocol, which involved thoroughly sanitizing and cleaning ultrasound equipment between patient scans and setting aside certain ultrasound machines for use only on COVID-19 patients. Single-use packages of gel and other consumables were used only once.
"It's relatively easy to clean ultrasound equipment, which is smaller than other imaging systems with more accessible areas. Of course, you need to be especially cautious with unconfirmed COVID cases, as we can't rule out the possibility of fomite transmission," he added.
Ultrasound's utility during the pandemic is expected to continue as another wave of COVID-19 affects the population.