An international team of researchers created 3D-printed navigational templates that were just as accurate as CT at locating small lung nodules before surgery. The templates had the added benefits of shorter operating times and lower radiation exposure, according to an article recently published online in JAMA Surgery.
Small peripheral lung nodules are often difficult to find during minimally invasive surgical procedures. Failing to spot them is the most common reason for surgeons to call for a thoracotomy, a major surgical procedure that involves opening the chest, wrote corresponding author Dr. Chang Chen, PhD, from Shanghai Pulmonary Hospital in China and colleagues.
In response to this challenge, clinicians have developed several methods to home in on lung nodules both pre- and intraoperatively, minimizing the need for invasive surgery, the authors wrote. Perhaps the most widely used method involves having an interventional radiologist use CT to guide the measurement and manual placement of a localizer onto a patient. Though the localizer is effective at helping surgeons identify small lung nodules, CT guidance usually requires multiple attempts for accurate placement.
To improve upon lung nodule localization, Chen and colleagues created 3D-printed navigational templates based on data from patient CT scans as well as the operating surgeon's proposed insertion route for placing the localizer onto the patient. Manufacturing each 3D-printed template cost roughly $100 and took approximately six hours (JAMA Surg, December 26, 2018).
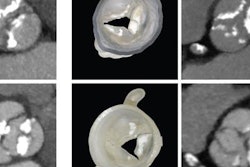
 3D-printed navigational template for localizing lung nodules. Image courtesy of Dr. Chang Chen, PhD.
3D-printed navigational template for localizing lung nodules. Image courtesy of Dr. Chang Chen, PhD."This navigational template-guided approach gives the operating surgeon full control over a patient's surgical strategy, as the insertion route of the localizer dictates the manipulation of the endostaplers during wedge resection," they wrote.
The researchers performed percutaneous lung nodule localization using conventional CT guidance or 3D-printed template navigation on 190 patients scheduled to undergo minimally invasive lung nodule resection.
While there was no statistically significant difference in deviation between using the 3D-printed templates or CT guidance, there were statistically significant reductions in average operating time and effective radiation dose with the templates. Also, the operating surgeon was also able to situate the localizer with fewer attempts using the 3D-printed template than he was able to with CT. There were no statistically significant differences in postsurgical complications between the two groups.
| CT vs. 3D-printed template for lung nodule localization | |||
| CT | 3D-printed template | p-value | |
| Deviation between localizer and targeted lung nodule | 9.6 mm | 8.7 mm | 0.36 |
| Average operating time | 9.5 minutes | 7.4 minutes | < 0.001 |
| Effective radiation dose | 4.4 mSv | 3.2 mSv | < 0.001 |
| Cases completed on 1st attempt | 6% | 89% | |
Though the authors successfully demonstrated the use of their 3D-printed template process, it is also important to "consider whether complicating the logistics and adding the expense of 3D printing to lung nodule localization are appropriate uses of resources in a healthcare economy that is actively working to cut costs and improve efficiency," wrote Dr. Douglas Wood and colleagues from the University of Washington in an accompanying editorial.
"Probably the most important point is that the majority of lesions examined in their study required no resection," they added.