The hybrid OR suite, page 2
Interdisciplinary education and training
In commissioning hybrid operating rooms, it is important to identify and address knowledge gaps among clinical staff members as this is a joint function between two main groups. The fast pace of changing technology also contributes to the need for ongoing training. A good example is the need to address radiation exposure, a major safety concern in the use of interventional radiology procedures.
From experience with the prototype hybrid OR, it became evident that while our interventional radiologists and technologists had good awareness of potential radiation risks and good radiation safety practices, the operating room staff did not. To address this issue, the radiology clinical nurse specialist and interventional radiology director developed an instructional module that all team members were required to complete. Radiation monitoring of personnel with dosimeters continued as usual along with systematic preventive maintenance, lead quality-control programs, and calibration of x-ray equipment.
Another educational initiative involved teaching a large group of operating room nurses various point-of-care testing (POCT) methods for tests such as anticoagulation clotting time and renal function assessment. Previously, a very small group performed these tests, but this became infeasible in this larger scale. A training program commenced to ensure the entire hybrid OR team was proficient with POCT.
Once we had an occupancy permit, we began multidisciplinary training including unit tours, fire and life safety training, in-service training on new imaging and support technologies, and, perhaps most importantly, team training with case simulations. Multidisciplinary case simulations were designed and practiced well before moving into the new suites and using them clinically. These exercises involved all disciplines: surgeons, interventional radiologists, anesthesia providers, nurses, radiology technologists, and operating room assistants. These exercises helped the multidisciplinary team make decisions on where the morning huddle would occur, where the movable equipment would be placed, and how we would manage emergencies.
Role clarification
In addition to providing the appropriate training and education, the importance of clarifying roles and responsibilities of the surgical and radiology teams cannot be overstated. Initially, before the new hybrid OR build outs were complete, the vascular surgeons would schedule hybrid cases in the interventional unit with a primarily OR team. With the original retrofit hybrid OR, radiology staffed that suite with a single IR technologist who was supervised by the operating room nursing leadership.
It soon became obvious that this model had severe limitations: inflexible coverage, lack of understanding by OR personnel and surgeons about imaging capabilities, and lack of attention to detail about radiation issues. Once these limitations were identified and evaluated, the interventional radiology department began more comprehensive staffing of the prototype hybrid operating room. The goal was to offer adequate technologist coverage and backup coverage to support patient care on a 24/7 basis and to bring the full knowledge and capability present in the IR section for the imaging applications, equipment management, and radiation safety to bear.
The workflows for each of the disciplines sharing the hybrid ORs are different yet overlapping, and the harmonization of practices needed open communication. For the new facility, we decided to staff each interventional operating room with one registered nurse, one surgical technician, and one interventional radiology technologist along with the usual complement of radiology or surgical physician staff.
Going beyond vendor specification
Gathering a comprehensive equipment list is critical in determining the square footage requirement for hybrid suites or the feasibility of retrofitting an existing room. In our case, we began by having the end users generate an initial list of equipment options, and then passed this along to the full team for validation.
Once we had the list, in order to better understand the required square footage, we worked closely with the vendors to generate data sheets with all the detailed specifications for each component. We then modeled various configurations of equipment and table placement, from basic room setup to different intraoperative modes for both open and endovascular procedures.
The team then began working closely with various vendors to innovate and develop custom solutions for some of the key components, with particular attention to lessons learned from the prototype hybrid OR. In the following sections we give two examples of design outcomes beyond the original vendor specification.
Breakable and exchangeable hybrid OR table
Our decision to use a breakable/exchangeable tabletop that would interchange between a surgical tabletop and a traditional imaging/radiology table is a good example of a custom solution arrived at through a multidisciplinary design team. The table selected allows the lower and the upper regions to flex up and down for flexible surgical positioning.
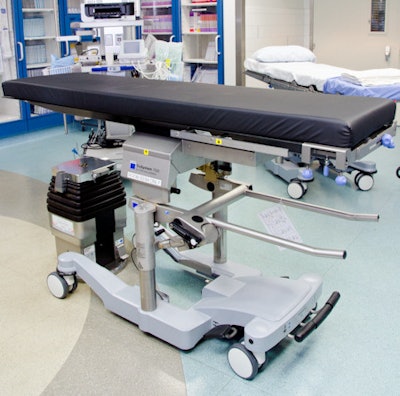 Figure 1: Breakable surgical tabletop on the left, interchangeable to an imaging/radiology table on the right. All images courtesy of the authors.
Figure 1: Breakable surgical tabletop on the left, interchangeable to an imaging/radiology table on the right. All images courtesy of the authors.A major challenge in selecting a functional table for hybrid ORs is when endovascular cases need to convert to open procedures. Because transferring an anesthetized patient is not ideal, a breakable/exchangeable table that still allows for some level of imaging is imperative in urgent situations. A breakable table allows you to break the table at the foot and head-end for the required surgical positioning of vascular patients.
The practice at MGH encompasses a substantial volume of open surgical cases, as well as a robust EVAR and TVAR practice. This calls for the functional capabilities of a breakable OR table for open cases or in the event of a conversion to open technique during EVAR or TVARs.
Specific fundamental requirements for an operating room table include the ability to attach retractors and arm boards with reliable stability. There are also specific requirements for an interventional imaging table, such as the use of radiolucent material to allow for imaging through the table. At the time of our design phase and even now, the products in the market for both of these specific requirements are limited.
In the end, we decided on a Trumpf 7500 fixed-pedestal system. The table has two configuration options enabled by a breakable and exchangeable tabletop trolley system (figure 2): an operative tabletop and a radiolucent-imaging tabletop. MGH is the first to install this table. The system involves specially designed clamps that the OR nurses use to place needed retractors when a conversion to open technique becomes inevitable. With this new design, the trolley exchange system can be operational within a minute.
However, as is the case with many decisions in the hybrid environment, the selection of a pedestal table required a trade-off that results in a limitation in the distal imaging of the lower extremity vasculature. This is directly related to the inability to extend the imaging device beyond the table's fixed pedestal and the limited travel of the tabletop itself. Surgeons, IR physicians, and the executive project team were aware of the compromise; ultimately, the decision was made to continue with the installation of the exchangeable tabletop system, as the benefits were felt to outweigh the limitations.
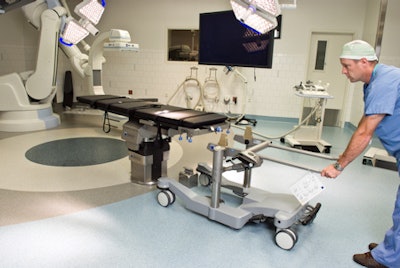 Figure 2: Trolley tabletop exchange system.
Figure 2: Trolley tabletop exchange system.Quick connect
Another challenge was to keep the cables off the floor; this related to the decision of using a pedestal table with the tableside C-arm controls. In traditional table setups, the cables supporting tableside controls run up through a conduit in the imaging table base. In two of the hybrid suites employing a table pedestal system, the fixed pedestal did not allow any space for cables to run through the pedestal. Moreover, the pedestal has a telescoping function which would subject the cables to friction, wear, and possible tearing.
In our original prototype hybrid OR, having tableside controls required a corrugated cable that sprawled across the floor from a wall outlet to the trolley unit housing the controls. The trolley unit was cumbersome in the surgical field.
Additionally, to optimize viewing in an imaging case, the room lights are often dimmed for a major portion of the procedure. Working in a dark operating room meant that team members were prone to trip over the large control cable. Therefore, we decided to provide an additional coring in the floor immediately adjacent to the pedestal table base to allow the cables for the imaging device controls to connect directly to the control trolley, avoiding the need to have cables running across the floor from the wall (figure 3).
With vendor support and input, we developed a custom solution we call the "quick-connect box" for the connection at floor level. This system has a set of push pins that guide the connection and can be clamped down to prevent liquid infiltration into the cable raceway. Cables from the quick-connect box next to the OR table base run up to the tableside, allowing for tableside control of the imaging device with the pedestal configuration.
This approach also solved a long-standing functionality challenge that presents when a pedestal table is installed with a fixed, floor-mounted C-arm. It allows the quick-connect box to be located under the OR bed should a provider desire tableside controls instead of having the interventional technologist controlling the C-arm from a remote trolley system, or having a trolley system in the surgical field.
To act in accordance with OR environmental standards, we had the box constructed from a single piece of stainless steel, allowing for easy cleaning and resistance to liquids. Initially, there was some concern that the box, which was raised above the floor, would be a tripping hazard, but placement under the table mitigated that concern.
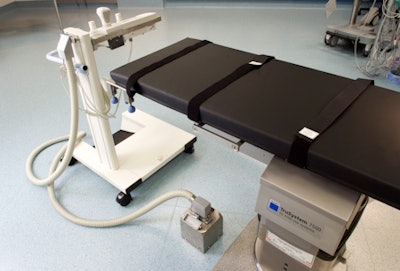 Figure 3: "Quick-connect" box to avoid having cables running across the floor from the wall.
Figure 3: "Quick-connect" box to avoid having cables running across the floor from the wall.Previous page | 1 | 2 | 3 | Next page