Automated breast ultrasound (ABUS) is useful as an adjunct to digital breast tomosynthesis (DBT) in opportunistic screening and diagnostic imaging, suggest findings published October 14 in Ultrasound in Medicine & Biology.
A team led by Kartini Rahmat, MBBS, from Universiti Malaya in Kuala Lumpur, Malaysia found that when ABUS and DBT were added to the screening population of its study, the biopsy rate was about 23%. The cancer detection yield from both modalities was just over 9% for both screening and diagnostic groups.
“The results from our study can be applied in countries with no population screening," the Rahmat team wrote.
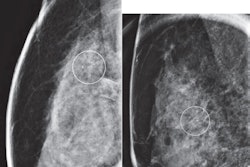
DBT continues to be studied as more breast imaging facilities adopt the technology. Previous studies suggest that using DBT over 2D mammography results in an overall reduction in recall rate and an increase in cancer detection rate. However, the technology still contends with the challenge of imaging dense breasts, with women having extremely dense breasts being at higher risk.
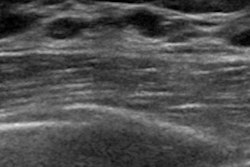
Previous studies have also highlighted the capabilities of ABUS to further identify additional invasive cancers, which tend to be small and node-negative. The researchers noted that ABUS overcomes conventional ultrasound’s weakness of being user-dependent while detecting breast cancers masked by dense breast tissue.
Rahmat and colleagues sought to assess the diagnostic performance of ABUS as an adjunct to DBT in both breast cancer screening and diagnostic imaging. In their cross-sectional study, the researchers included women who underwent DBT and ABUS from 2019 to 2022. These included opportunistic and targeted screening cases, as well as symptomatic women.
The team included 1,089 ABUS exams, with 909 being screening exams and 180 being diagnostic exams. It also noted that a total of 579 biopsies were performed on 407 women, with a biopsy rate of 53.2%. Of the total lesions, 100 (9.2%) were malignant, 30 (5.2%) were atypical/B3 lesions, and 414 (71.5%) were benign cases.
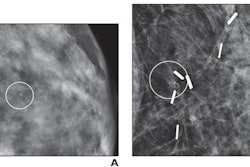
However, collection of the biopsied lesions found that several patients underwent more than one biopsy. The researchers reported that a total of 135 (23.3%) malignant lesions were detected in 579 biopsies. Of these, 75.8% were detected by ABUS plus DBT, 6.7% through ABUS alone, and 14.1% through DBT alone.
The researchers found that in nine cases (0.08%), ABUS alone detected malignancies. DBT alone meanwhile detected malignancies in 19 cases (1.7%).
The team also reported that the proportion of examinations with abnormal findings that resulted in a tissue diagnosis of cancer (PPV3) was 14.6% in the screening group. Additionally, the false-positive rate in the screening group was 62.7%.
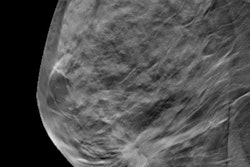
Of the 135 malignant lesions, 85.9% (116/135) were detected on the coronal view of ABUS, according to the researchers. They also found that in this group, 45.6% (54/116) were “black hole and retraction sign,” 43.1% (50/116) were “black hole without retraction sign,” 5.2% (6/116) were “black hole with white hole” and 5.2% (6/116) were “retraction sign” alone.
Study co-author Nazimah Ab Mumin, MBBS, said that the university hospital employs targeted and opportunistic screening, meaning the study population screened is skewed in the high- and higher-than-average population than general.
"Furthermore, we also included diagnostic cases in the study group," Ab Mumin told AuntMinnie.com. "Due to the inclusion criteria, this is then reflected in the results of the high biopsy rate and false positive rates."
Ab Mumin also noted that the study was performed in a single center and during the pandemic, meaning that patients who presented for screening and diagnostic cases during that period were "generally in the high-risk group than normal."
The study authors highlighted that their results show a positive effect on breast cancer detection for ABUS as an adjunct to DBT in an opportunistic and targeted screening program. They called for multicenter studies involving several ABUS applications to further test their hypothesis.
The full study can be found here.