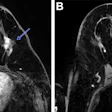
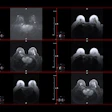
The American College of Physicians (ACP) released new guidelines this week suggesting that women ages 40-49 may not benefit from annual mammography screening. In this editorial, Dr. Daniel Kopans, professor of radiology at Boston-based Harvard Medical School and a senior radiologist at Massachusetts General Hospital, responds to the new ACP recommendations.
The ACP's professed reason for the new guidelines is to provide accurate information so that women can make informed decisions. But by reinforcing the myth that the parameters of screening change at the age of 50, they continue to mislead women and their physicians.
Unfortunately, the ACP committee that reviewed the data on mammography screening for women ages 40-49 did not appear to understand randomized, controlled trials, and clearly did not understand published breast cancer screening data.
The suggestion that participation in screening can be tailored by an individual's risk is scientifically unsupportable. Furthermore, screening women based on known risk factors will mean missing 75% to 80% of breast cancers.
As I have pointed out numerous times, none of the randomized, controlled trials was designed to permit the analysis -- in the early years of follow-up -- of women ages 40-49 as a separate subgroup. The trials lacked the statistical power to do so. As a result, the analyses that have been done violate a basic rule for analyzing trial data. The U.S. Food and Drug Administration (FDA) would never permit the use of unplanned subgroup analysis that lacked statistical power, so how can analysts make medical recommendations based on this kind of analysis?
The ACP committee members should be asked how they can base decisions on unplanned analysis of subgroups when statistical power is absent. If this were scientifically supported, then by looking at smaller and smaller subgroups, only two women would need to participate in trials! This is nonsense. In the early years of follow-up, published randomized, controlled trials have shown a benefit for screening, beginning at the age of 40, when the trials are analyzed properly -- the way they were designed.
With longer follow-up, and more deaths, the power of the trials increases, and when the data for women ages 40-49 are analyzed separately, the Gothenburg Breast Cancer Screening Trial shows a 44% statistically significant benefit for screening women before the age of 50. The Malmo Trial shows a statistically significant 35% benefit. All five Swedish trials show a significant 29% reduction in deaths, and the population-based trials demonstrate a 26% significant benefit. These are as good, or even better, when the data are analyzed for women ages 50 and older.
The ACP committee disparaged this "delayed" benefit. Actually, the committee should be asked to explain how periodic screening should be expected to result in an immediate benefit given the phenomenon of length bias sampling (periodic screening detects moderate and slower growing cancers).
It is only when the Canadian National Breast Screening Study is added that the benefit drops to 15%. But the Canadian trial violated the basic rules for randomized, controlled trials. In this study, women were examined before allocation and were allowed to participate in a screening trial even though they had breast masses and palpable axillary nodes (advanced cancer). They were assigned to be in the screened group or the control group on open lists so that women with advanced cancer were assigned to the screened group. This arrangement rendered undetectable the evidence of this randomization compromise.
Statistically, more women were assigned to the screened group with advanced cancers than the control group. This is why the control group had a better than 90% five-year survival (versus the expected 75%) while, not surprisingly, more deaths occurred in the screened group.
How does the ACP committee, made up of supposedly knowledgeable reviewers, overlook these major problems with the Canadian trial? A drug trial that was performed in this fashion would be thrown out by the FDA. Did the ACP committee even take into account the poor quality (proved by a review that I participated in and acknowledged by the trial's own physicist) of the mammograms in the trial?
None of the parameters of screening changes abruptly at the age of 50 or at any other age. The ACP neglected to inform women that the age of 50 is completely arbitrary. It is an artifact of performing analyses that repeatedly groups women ages 40-49 and compares them to the group of women ages 50-74.
This kind of dichotomous comparison will make any gradual changes that occur with increasing age appear to change abruptly at the age of 50 (or any other age that you wish to chose). My children understand this -- why didn't ACP committee members understand this simple concept?
The ACP committee suggests screening suddenly begins working for women once they reach age 50. This notion is based on a 1995 paper by Dr. Harry de Koning, "Quantitative interpretation of age-specific mortality reductions from the Swedish breast cancer-screening trials" (Journal of the National Cancer Institute, August 16, 1995, Vol. 87:16, pp. 1217-1223).
The ACP committee clearly did not know that de Koning repudiated his conclusions during the National Institutes of Health's Consensus Development Conference Statement in 1997, and reaffirmed the repudiation to me in 2004. For more on this topic, the ACP committee should read a paper that I authored, "Informed decision making: Age of 50 is arbitrary and has no demonstrated influence on breast cancer screening in women" (American Journal of Roentgenology, July 2005, Vol. 185:1, pp. 176-182).
Finally, the ACP committee states that radiation risk is a concern, yet they also acknowledge in the guidelines that no data exist to support the concern.
The bottom line
There is clear evidence from the randomized, controlled trials -- and from studies of mortality rates when screening is used in the general population -- that mammographic screening can reduce the death rate for women who begin screening by the age of 40. The mortality rate in the U.S. has decreased by 25% since 1990, primarily due to mammography screening.
The current controversy over the ACP guidelines is not a matter of experts disagreeing, but a matter of some analysts not understanding the trials and the data. There is no scientific support for recommending screening based on risk. Furthermore, the known risk factors only account for 20% to 25% of all cancers, so that screening based on risk will overlook 75% to 80% of cancers.
All women should be informed of the risks and benefits of any medical intervention -- not just those under the age of 50. Women should also be advised to follow the American Cancer Society guidelines. The ACP should cease misinforming the public.
By Dr. Daniel B. Kopans
AuntMinnie.com contributing writer
April 5, 2007
Dr. Kopans is a professor of radiology at Harvard Medical School and the director of the breast imaging division at Massachusetts General Hospital, both in Boston.
The opinions expressed in guest editorials are those of the author, and do not necessarily reflect the views of AuntMinnie.com.
Related Reading
Tailored approach best for breast cancer screening of women in their 40s, April 3, 2007
Mammographic screening reduces breast cancer mortality, March 14, 2007
What goes up must come down -- A new look at the 2003 drop in breast cancers, December 22, 2006
Cochrane update: Breast cancer screening curtails mortality, but at what cost?
Benefit of breast cancer screening small - study, July 20, 2005
Copyright © 2007 AuntMinnie.com