TORONTO - A dedicated PET mammography unit turned in good results in detecting ductal carcinoma in situ (DCIS) in symptomatic high-risk patients, according to research presented this week at the Society of Nuclear Medicine (SNM) meeting. The research indicates that the PEM scanner could help breast imagers detect cancer at an earlier stage, before it has metastasized.
DCIS represents one-third of all detected nonpalpable cancers, and catching cancer at such an early stage can have a major beneficial impact on a patient's prognosis, according to Deepa Narayanan of Naviscan PET Systems, the Rockville, MD-based company that manufactures the PEM Flex camera used in the study. Naviscan began shipping the camera 18 months ago and has six systems installed.
DCIS can be difficult to detect with existing imaging modalities, however, Narayanan said. X-ray mammography has a sensitivity of about 55%, she said, while ultrasound has a sensitivity of 47% and MRI clocks in at just 17% for detecting DCIS in high-risk patients.
Whole-body PET studies have demonstrated 25% sensitivity for DCIS, but the PEM Flex camera improves on that performance thanks to its dedicated design. The system has intrinsic spatial resolution of 1.5 mm, about the size of a duct, and 100 times the count sensitivity of a whole-body PET camera, Narayanan said.
The PEM Flex system was used in a prospective multicenter clinical study that involved two academic centers and two community hospitals. The researchers recruited 94 consecutive women who either had biopsy-proven cancer or suspicious breast cancer.
Patients were injected with an average of 12 mCi of FDG and were scanned 95 minutes after injection. Patients were scanned in both breasts in standard craniocaudal and mediolateral oblique mammography views, with each breast taking 10 minutes to scan.
Some 17 cases could not be evaluated, leaving the research group with 77 patients. The PEM scans were read by a panel of radiologists with clinical history and mammograms to mirror actual practice patterns, but they were blinded to pathology results, Narayanan said.
The group found 48 tumors in the 77 patients, with the PEM system detecting 10 of the 11 cases of pure DCIS, for a sensitivity of 91%. Narayanan said this compares to a sensitivity of 56% for conventional imaging, which she interpreted to be an aggregate of mammography, breast ultrasound, and clinical breast examination. PEM also detected four incidental lesions, picked up in addition to the original confirmed or suspicious lesion that had been detected on mammography.
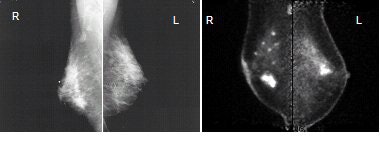 |
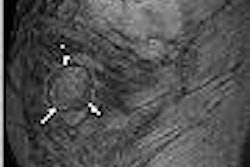
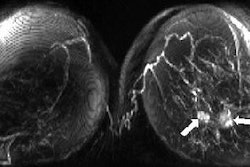
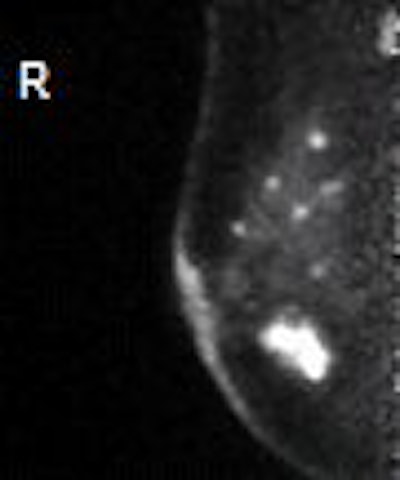
| Images of 50-year-old woman with bilateral breast masses, mammography on the left and PEM on the right. X-ray-guided biopsy showed invasive cancer in right breast, papilloma in the left breast. PEM findings: Left breast very suspicious for cancer. Surgery revealed DCIS. Images courtesy Dr. William Stein and Dr. Marybeth Lobrano, PET Fusion Center, East Jefferson General Hospital, Metairie, LA. |
PEM saw three cases of DCIS foci that were occult on mammography, and one case was missed by all modalities and was discovered only after prophylactic mastectomy. PEM was also able to determine an intraductal component to DCIS in 70% of cases, compared to only 40% for mammography, Narayanan said.
PEM's ability to detect intraductal extension is an important benefit in surgical planning, she said. Researchers in the study were able to use the technology to predict whether the patient would benefit from breast-conserving surgery. In 11 of 19 patients who received lumpectomy, PEM successfully predicted a lumpectomy with clean margins and correctly predicted an unsuccessful lumpectomy in six patients, for a specificity and positive predictive value of 100%.
Narayanan said that the results indicate that PEM could carve out a role in helping physicians decide what type of surgery to use in women with DCIS. Because DCIS is often found in high-risk women, PEM could also be used to screen women in this cohort, and the National Cancer Institute is funding prospective clinical trials to compare PEM with MRI, which has found increasing use as a screening modality for high-risk women.
In the discussion period after the presentation, an attendee queried Narayanan on the large number of patients who were excluded from the study -- nearly 20%. She said that five cases were excluded because the researchers didn't have surgical pathology due to the study's short 30-day follow-up period, two cases were lymphoma, one case was excluded because of a faulty image due to equipment failure. There were also two cases in which patients were imaged multiple times, and in other cases technologists entered incorrect data.
Breast density also affected image quality due to diffuse FDG uptake in those patients with dense breasts, but the phenomenon did not affect the accuracy of image interpretation, she said.
In comments after the presentation, Dr. Iraj Khalkhali of Harbor-UCLA Medical Center in Los Angeles said that as one of the readers in the study he was impressed with the system's image quality. The unit is capable of visualizing incidental DCIS that otherwise is underdiagnosed, and images are easier to read than breast MRI scans.
But scanning symptomatic women, as the current PEM study did, is of limited value, as these patients are already going to receive biopsy or some other surgical intervention. Future PEM clinical studies will examine the technology in asymptomatic women, and if it excels here it could have a real clinical role.
"If they can prove that this kind of technique has validity in picking up cancers that otherwise are not picked up in high-risk patients, I think that's a great contribution," Khalkhali said.
By Brian Casey
AuntMinnie.com staff writer
June 22, 2005
Related Reading
PEM development picks up pace, February 7, 2005
Road to RSNA, Naviscan PET Systems, November 8, 2004
FDA clears Naviscan PET scanner, September 9, 2003
PET outperforms CT in breast cancer staging, May 7, 2003
Pinhole technique abets dedicated breast SPECT imaging, April 24, 2003
Copyright © 2005 AuntMinnie.com