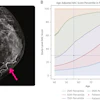
U.S. mammography centers are doing a moderate amount of double interpretation of images, and they're also charging double for their overall services, according to an industry snapshot published in the latest American Journal of Roentgenology.
This 10-month long survey was designed to "obtain a picture of the practice of mammography in the United States." "Facilities providing screening mammography services ... have changed dramatically in the past decade," wrote R. Edward Hendrick, Ph.D., and colleagues (AJR, February 2005, Vol. 184:2, pp. 433-438).
In addition to interpretation patterns and charges, the group also gleaned data on audit systems, volume, and the use of advanced imaging techniques.
In a second AJR paper, a group from Massachusetts studied whether relaxation techniques would reduce pain and anxiety during screening mammography. Discomfort and fear is often cited as a reason that women may not turn up at screening centers for their annual exams, the authors stated.
Monitoring mammo practice
The survey used in the first study was developed by a team of experts in breast imaging, medical physics, economics, biostatistics, and epidemiology. It included basic questions on breast imaging and clinical care services and charges, as well as diagnostic mammography, interpretation methods, and patient databases. The survey did not request data on revenues.
One of the strengths of this study was that "the facilities surveyed constitute a varied cross-section, both geographically and demographically," wrote Hendrick's group. Hendrick is from the Lynn Sage Comprehensive Breast Center at Northwestern University in Chicago. His co-authors are from institutions in Reno, NV; Hanover, NH; Atlanta; and Seattle.
The surveyed centers (both rural and urban) were part of three cancer surveillance programs: a nonprofit health plan in the Pacific Northwest, the New Hampshire Mammography Network, and the Colorado Mammography Advocacy Project. All the facilities are part of the National Breast Cancer Surveillance Consortium (NBCSC).
The response rate to the survey was 85% with lead technologists completing the questionnaire. Most facilities performed at a medium volume (between five to 15 exams per machine per day). The majority of facilities (53%) were nonhospital-based clinics or office-based practices.
The facilities offered a range of breast imaging services, including ultrasound, MRI, and scintigraphy, with most providing diagnostic mammography (76%). Cyst aspiration (53% of the centers) and needle localization were the most frequently performed interventions.
All the centers charged two times more than Medicare rates for screening (median total charge of $141) and nearly the same for diagnostic mammography (median total charge of $153.35 or 1.7 times more). The authors attributed this difference to the disparity between cost and reimbursement.
"These cost data reflect the continuing problems that facilities and radiologists face in providing mammography services," they said.
With regard to interpretation, 38% of survey respondents said same-day evaluation of screening mammograms with abnormal results was unavailable. However, 62% interpreted screening exams onsite, while 91% did diagnostic exams onsite. Batch reading was done at 84% of the centers, a significant increase from 2002 when only 20% reported batch interpretation.
"This striking change to batch interpretation ... reflects the fact that batch interpretation is more time-efficient and cost-effective than interpreting screening examinations while patients wait for results," the authors stated.
Eleven percent of the respondents reported double interpretation of all screening mammograms. Better than half (56%) of those surveyed said they performed some type of double reading on all diagnostic mammograms. But the fraction of cases that were read twice ranged from 1% to 80%, prompting the study authors to note a lack of standardization for double reading. Finally, very few facilities offered full-field digital mammography (FFDM) or computer-aided detection (CAD).
Overall, the survey results indicated that mammography centers have vastly improved their quality assurance and medical audit tools over the last 10 years, the authors concluded. The bulk of the facilities stated that they offered performance feedback to the radiologists at least once a year.
Mammo pain myth?
One way mammography centers could ramp up the volume would be to encourage compliance for annual screening. But past studies have indicated that the pain experienced during mammography is a reason why women do not follow screening guidelines. In a new study, researchers from Massachusetts offered relaxation techniques to women undergoing mammography to determine if the methods eased the women's pain and anxiety during the procedure.
"If a simple, inexpensive, noninvasive intervention could decrease distress during mammography ... it is hypothesized that compliance with screening guidelines would increase," wrote Alice Domar, Ph.D., and colleagues in their report (AJR, February 2005, Vol. 184:2, pp. 445-447).
Domar is the director of the Mind/Body Center for Women's Health at Boston IVF in Waltham, MA. One of her co-authors is Dr. Janet Baum, chief of breast imaging at Beth Israel Deaconess Medical Center in Boston. The other co-authors are from Brigham and Women's Hospital, also in Boston, and the Advanced Medical Research Foundation in Chestnut Hill, MA.
A total of 143 volunteers were placed into three different groups: 50 were in the relaxation group, and were asked to listen to a relaxation audiotape before and during the exam. Forty-seven were assigned to a music group and listened to either classical, jazz, or soft rock. Forty-six subjects in the control group listened to a blank tape.
The women also filled out the State-Trait Anxiety Inventory (STAI) and McGill Pain Questionnaire (MPQ). They assessed their distress levels on a Likert scale with 1 representing no pain and no anxiety, and 10 representing very painful as well as very anxious.
The surprising result of the experiment was that mean STAI and MPQ scores for all the groups were low, the authors stated. "Contrary to expectations, subjects who listened to a relaxation audiotape before and during their screening mammography did not report any benefits from the intervention when compared with subjects who listened to music or a control group."
The mean Likert pain scores were 3.4 for the relaxation group, 3.7 for the music group, and 3.8 for the control group. The mean Likert anxiety scores were 2.6, 3.2, and 2.8, respectively. The MPQ scores were 11.8, 12.5, and 13.7 for relaxation, music, and control, respectively, while the adjusted STAI was 29.8, 31.1, and 33.6.
Given the abundance of prior research that links pain and anxiety issues with screening compliance, Domar's group suggested that their unique results may have been because of a bias, i.e., the possibility that the anxious women opted not to take part in the study, leaving only volunteers who were already calm and confident.
This possibility inspired the group to take another tack: They have designed a similar study that will evaluate a more distressed population, such as women who have been called back for a repeat exam. Previous investigations have also shown a connection between fear of the exam and fear of abnormal results, they pointed out.
More immediately, the 143 women in the current study will be followed-up for 15 months to see if they return for screening.
By Shalmali Pal
AuntMinnie.com staff writer
February 2, 2005
Related Reading
Breast biopsy costs big bucks, but so does cancer screening, September 19, 2005
When push comes to shove: Addressing compression in mammography, October 5, 2005
Feeling down may prompt women to skip breast screening, August 31, 2004
Diligent coding means money in the bank for breast imaging, May 21, 2004
Investigators find x-ray dose reduction varies widely among digital mammo machines, December 3, 2003
Copyright © 2005 AuntMinnie.com