For obtaining medialateral oblique views, Heinlein recommended the following method:
- Ask the patient to bend forward from the waist. However, "when she does this, do not pull the mound of the breast tissue first. Instead, you want to go for the axillary and upper-outer quadrant first and then displace the implant."
- After the patient has stood up, ask her to place her hand on the handlebar with the corner of the bucky in the posterior aspect of her armpit.
- The mammographer then places the edge of his or her fingers, holding the lateral tissue, on the edge of the bucky.
- "I ask the woman if she feels that the plate is pushing against her ribs or pushing against the edge of her breast. If she says her ribs, that means I do not have the implant sufficiently displaced." If she says the plate is against her ribs, start over.
- Place the edge of the spatula against the displaced implant and flip it vertically to hold it back. "Just before the exposure, I feel along the back because I want to make sure the implant is displaced posteriorly, both from the interior aspect of the breast, the medial aspect, and the lateral aspect," Heinlein said.
Implant abnormality or possible problem?
"The major problem that we face as imagers is that [implants] interfere with mammography," Monsees said. "The question that often arises is ‘Does it cause so much of a problem, it ends up delaying diagnosis for breast cancer?’ There’s no single scientific study that’s going to answer that question for us."
But knowing what kinds of pitfalls are associated with implant imaging can make the mammography process less daunting. Some of the most common abnormalities associated with implants include cosmetic problems, in which the implant rides too high or too low; the presence of infection, even after the implants have been removed; and the formation of fibrous tissue around the implant, which affects compressibility.
The latter is known as capsule contraction and occurs when the body walls off the implant by developing a fibrous tissue around it. It is estimated that about 50% of women with implants have capsule contraction, although the degree of severity varies from case to case, Monsees said.
Another imaging roadblock that mammographers might run into is the calcification of the fibrous capsule or hickory bark calcification. Even if implants have been removed, the fibrous capsule is not always taken out, Monsees said. Scars that are located against the chest wall may also hamper imaging.
"It really does obscure the breast tissue and it does interfere with photo-timing," she said. "You are going to have to use a manual exposure."
While the life expectancy of implants depends on the type, implant failure is something that mammographers should be on the lookout for. Intracapsular rupture, in which the capsule is intact but the implant envelope has ruptured, cannot be seen with mammography, Monsees said. However, extracapsular rupture, in which there is free silicone or saline outside the fibrous capsule and in the breast parenchyma, can sometimes be caught.
Focal pain, burning, implant softening, or a decrease in size is associated with failure. If the patient has any of the above complaints, mammographers should keep an eye out for free silicone lumps or granulomas, as well as silicone uptake in the lymph nodes.
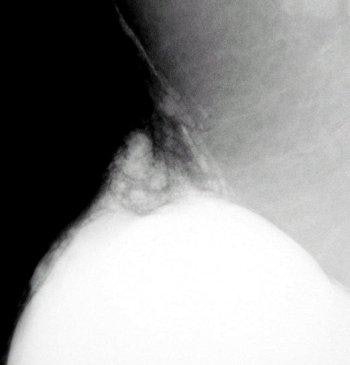
An extracapsular rupture of a silicone implant. Photo courtesy of Dr. Barbara Monsees.
"Contour abnormalities may be present and suggest rupture, but they are not specific to rupture," Monsees said. "Most implant ruptures go up and into the outer quadrants of the breast. So evaluate her and see how compressible she is. Take a single full view, including the implant, as a scout film and process it. Look at the film, and if there is silicone leaking, tell a radiologist and document it."
Finally, Monsees recommended that technologists ask a patient the following questions before starting the exam:
- How long has the woman had her implants?
- Are these the only set she has had, or did she previously have a set? Why were they removed?
- Are the implants saline or silicone? Are they located under or above the muscle?
- Have they been known to leak? Have they changed in size, contour, or compressibility?
- Are there any lumps in the breast?
Copyright © 2000 AuntMinnie.com