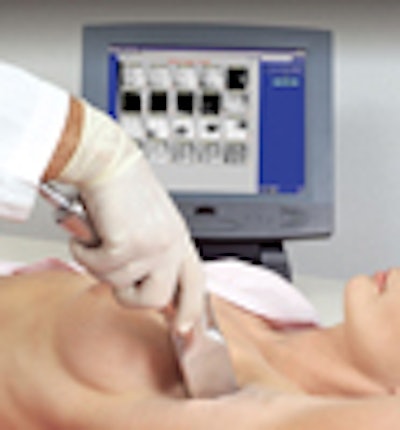
A company called Gamma Medica hopes to improve the efficacy of sentinel lymph node resection procedures with a new handheld gamma ray-detecting probe. While the California firm isn't the first to develop a gamma probe for surgical applications, the product is novel in that it's one of the first handheld probes that combines images with sound to localize malignant lymph nodes.
Gamma-detecting probes are being used increasingly as tools to assist surgeons during surgical procedures. They have become particularly useful in sentinel node biopsy procedures, in which the first node draining from a tumor is removed and examined for signs of metastasis.
Prior to surgery, patients are injected with a radiolabeled colloid that collects in lymph node tissue. The colloid enables surgeons using gamma probes to determine the exact location of the sentinel node, which is then removed and sent to a pathologist to look for signs of malignancy. The probes can help reduce patient morbidity and surgery time by enabling surgeons to remove just a few nodes, rather than conduct a total node dissection.
Handheld gamma probes currently on the market don't produce images, but rather create audible squelch tones to measure gamma ray emissions and alert surgeons to the presence of a lymph node. The Gamma Medica probe, called LumaGem Handheld Imaging System, differs in that it produces both tones and images of gamma ray emissions from lymph nodes, according to Bradley Patt, executive vice president of the Northridge, CA, company. Gamma Medica introduced the probe at the Society of Nuclear Medicine meeting in June.
The images are produced in real time and resemble video images, Patt said. If necessary, the probe can be held in place for 30 to 60 seconds to produce a higher quality image of gamma ray activity in the field of view.
The probe is particularly useful in differentiating between two lymph nodes that are located near each other, which might seem to be one area of activity with a non-imaging probe. "By using the sound and the images, you can locate the nodes more quickly, because you have more information at your fingertips," he said.
The LumaGem probe is based on a very-high-resolution scintillation camera with a 1 x 1-inch field of view. The camera produces images with intrinsic spatial resolution of 1.25 mm, three to four times better than conventional gamma cameras.
The higher resolution is due to the company's pixellated scintillation crystal design, which uses 1-mm crystal elements paired with very-high-resolution, position-sensitive photomultiplier tubes (PMTs). The discrete pixel elements restrict light to each crystal element, which reduces light spread and produces better spatial resolution.
The probe can be used as a stand-alone unit that can be placed on a cart and wheeled into a surgical suite. It can also be used as an add-on to the dedicated breast camera, Patt said. The price of the handheld probe alone should be about $35,000, he said, and the unit is now going into its first clinical sites.
In addition to lymph node procedures, the probe may also find use in breast cancer surgeries. It could be particularly useful in detecting malignant lymph nodes in the upper quadrant -- near the armpit -- which are difficult to detect using non-imaging probes because the gamma ray activity at the injection site interferes with that produced by the node, Patt said.
The probe is Gamma Medica's second product in development. The first, a dedicated scintimammography camera, was displayed at the company's corporate debut at the 1999 SNM meeting. Like the LumaGem handheld probe, the breast camera also features very-high-resolution detectors, although it uses sodium iodide crystals rather than the cesium iodide material used in the handheld probe.
The scintimammography system, also called LumaGem, received Food and Drug Administration clearance in January. That unit will be sold for about $150,000, with deliveries beginning at the end of the summer.
By Brian CaseyAuntMinnie.com staff writer
July 21, 2000
Let AuntMinnie.com know what you think about this story.
Copyright © 2000 AuntMinnie.com


















