MRI-guided transurethral ultrasound ablation (TULSA) is effective over surgery in men with prostate cancer, according to a study presented April 13 at the Society of Interventional Radiology (SIR) annual meeting in Toronto.
The finding is from a clinical trial comparing TULSA to robotic prostatectomy in 212 men at 23 medical centers between 2022 and 2025, noted principal investigator David Woodrum, MD, PhD, of the Mayo Clinic in Rochester, MN.
"These early results suggest that TULSA may allow patients to recover more quickly and maintain a better quality of life following treatment, while still effectively treating the cancer," Woodrum said, in a news release from SIR.
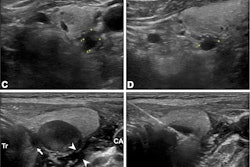
TULSA uses real-time MRI to guide the delivery of high-energy ultrasound through the urethra and into the prostate to heat and destroy cancer tissue without affecting surrounding organs, with the goal of preserving urinary and sexual function. Robotic prostatectomy, while effective for cancer control, can leave men with long-term effects including erectile dysfunction and urinary incontinence, Woodrum explained.
In the CAPTAIN trial, participants were randomly assigned to receive either TULSA or robotic prostatectomy. For TULSA versus surgery participants, the median age was 63 years old versus 65, median PSA was 6.5 ng/mL versus 7.2 ng/mL, and prostate volume was 41 cc versus 35 cc.
According to the results, men treated with TULSA had less blood loss during the procedure (zero mL versus 100 mL to 200 mL), had shorter stays (0.29 days versus 1.24 days), and reported less pain and faster return to normal activities one month after treatment.
"For many patients, how quickly they can get back to work, family life and everyday routines really matters," Woodrum said.
The researchers plan to follow participants over 10 years to compare longer-term outcomes, including urinary control, sexual function, and whether additional cancer treatment is needed.