Routine ultrasound can help reduce the risk of venipuncture and number of arterial puncture attempts, as well as improve first-pass success when it comes to interventional heart procedures, a Canadian study published September 19 in JAMA Cardiology found.
However, researchers led by Dr. Sanjit Jolly from the Population Health Research Institute in Hamilton, Ontario, also found that ultrasound for femoral access does not reduce bleeding or vascular complications.
"Ultrasonography does not appear to have any risks, facilitates access and is widely available," Jolly and co-authors wrote. "Therefore, it seems logical that physicians with required expertise and ready access to ultrasonography will use it to aid access."
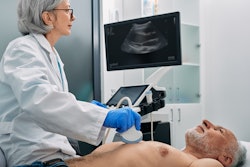
In heart procedures, femoral access is needed for large-bore procedures or when radial arteries are too small or blocked. Researchers over the years have tried to find ways to make femoral access safer, as it is prone to vascular complications.
Despite ultrasound being available to help with this at many practices, the majority of interventional cardiologists report not using it routinely.
Jolly and colleagues wanted to test ultrasound's effectiveness in safely guiding femoral access, using data from the Routine Ultrasound Guidance for Vascular Access for Cardiac Procedures (Universal) randomized clinical trial. The trial was designed to compare ultrasound guidance versus no such guidance for femoral arterial access on a background of fluoroscopy guidance for coronary angiography or intervention.
The team looked at data from a total of 621 patients who were randomly placed in ultrasound (n = 311) and no ultrasound (n = 310) groups. The patients had an average age of 71 years and 158 (25.4%) were female.
The researchers found that ultrasound was successful in some areas compared to not using its guidance.
| Ultrasound vs. no ultrasound guidance of femoral access | |||
| No ultrasound | Ultrasound | p-value | |
| First-pass success | 70% | 86.6% | < 0.001 |
| Average number of arterial puncture attempts | 1.4 | 1.2 | < 0.001 |
| Venipuncture occurrence | 11.7% | 3.1% | < 0.001 |
| Average times to access | 129 seconds | 114 seconds | 0.34 |
The researchers also wanted to look at the primary outcome for the groups. This included the composite of Bleeding Academic Research Consortium (BARC) 2, 3, and 5 bleeding or major vascular complications within 30 days.
The team found that the primary outcome occurred in 40 patients (12.9%) in the ultrasonography group compared with 50 patients (16.1%) without ultrasonography (p = 0.25). Out of these, the rates of BARC 2, 3, or 5 bleeding were 10.0% (n = 31) versus 10.7% (n = 33) (p = 0.78). Meanwhile, the rates of major vascular complications were 6.4% (n = 20) versus 9.4% (n = 29) (p = 0.18).
The study authors suggested that ultrasound could help reduce major bleeding and major vascular complications in patients receiving vascular closure devices. This is because ultrasound reduces the potential for multiple punctures, they wrote. However, the authors added that manual compression may compensate for multiple punctures, making it more difficult to view differences in groups for less serious complications.
"Furthermore, ultrasonography allows the operator to identify a puncture site free of calcium and disease making closure devices safer," the researchers wrote.
The team called for larger studies to show additional potential benefits of ultrasound-guided access.
In an accompanying editorial, Dr. Alexander Fanaroff and Dr. Jay Giri from the University of Pennsylvania wrote that this data, along with previous research, shows that ultrasound should be more routinely used in femoral access for coronary angiography and percutaneous coronary intervention.
"Any interventional cardiologist undergoing femoral access would request ultrasonography guidance from an operator well versed in the technique, just as they would refuse to jump out of an airplane without a parachute," they wrote. "Guidelines should reflect this reality, and more importantly, so should the care we offer patients."