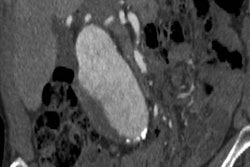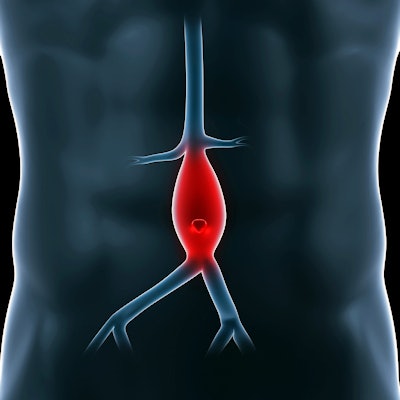
The U.S. Preventive Services Task Force (USPSTF) has reaffirmed with no major changes its 2014 recommendations on using ultrasound to screen for asymptomatic abdominal aortic aneurysm (AAA), in a new statement published online December 10 in the Journal of the American Medical Association.
After consideration of public comments on its draft recommendation statement, the USPSTF has finalized its guidance on AAA screening, which reaffirms the task force's 2014 recommendations with no substantial changes. The 2019 guidance for ultrasound AAA screening includes the following recommendations:
- One-time screening for male ever-smokers ages 65 to 75 (B grade)
- Selective screening for male nonsmokers ages 65 to 75 (C grade)
- No screening for female nonsmokers ages 65 to 75 without a family history of AAA (D grade)
- No recommendation for female smokers ages 65 to 75 with a family history of AAA due to insufficient evidence (I grade)
The group's evidence report was based on a review of 50 studies published through September 2018 that examined the potential harms and benefits of ultrasound AAA screening in roughly 320,000 individuals.
Collectively, results from the clinical trials showed that AAA screening in men 65 years or older was associated with reductions in AAA-related ruptures (odds ratio, 0.62), AAA-related death (odds ratio of 0.65), and emergency surgical procedures (odds ratio, 0.57) within the first 15 years after initial screening.
One-time screening also led to statistically significant increases in the total number of procedures performed per individual (odds ratio, 1.44). However, surgical treatment did not result in statistically significant reductions in AAA-related mortality or all-cause mortality within the first 12 years after initial screening, compared with surveillance alone.
Thus, although ultrasound AAA screening offered clear benefits for reducing AAA-related deaths in certain populations, the increase in elective surgeries in no way resolved the question of all-cause mortality, the task force noted.
The current USPSTF recommendations underscore a major gap in AAA screening -- a lack of evidence concerning the prevalence and potential benefits of screening among individuals, especially women and underserved populations, who smoke and have a family history of AAA, Dr. Julie Ann Freischlag from Wake Forest Baptist Medical Center noted in an accompanying editorial.
"More information is needed about the prevalence and growth rates of AAA in men and women with diverse backgrounds so that care -- including screening, follow-up, and treatment -- can be individualized, and outcomes for patients with AAA can be improved," she wrote.
In a separate editorial published in JAMA Network Open, Dr. Matthew Mell from the University of California, Davis pointed out that the Society for Vascular Surgery and other organizations recommend more liberal use of AAA screening to identify a broader group of individuals who may benefit from the exam.
"More research is needed to optimize diffusion of current recommendations and to identify other patient cohorts with a high pretest probability of AAA and who benefit from repair and therefore screening," he wrote.