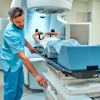
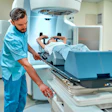
Squamous cell head and neck cancers -- predominantly diagnosed in inhabitants of low- and middle-income countries -- can be treated effectively with fewer, but higher, doses of radiation, according to research presented at the American Society for Radiation Oncology (ASTRO) annual meeting.
"Head and neck cancer caused by factors other than the human papillomavirus remains a significant burden especially in lower- and middle-income countries," said lead study author Søren Bentzen, PhD, DMSc, of the University of Maryland School of Medicine in Baltimore. "This is a trial that directly informs how you can effectively deliver radiation therapy to patients in a resource-scarce environment."
Squamous cell head and neck cancers are the seventh most common cancers around the world, Bentzen noted. They are associated with tobacco and alcohol use, and tend to appear in older people with comorbidities that may complicate treatment. incidence of these cancers is rising in low- and middle-income countries: For example, in India, they account for 30% of all cancer diagnoses (compared to 4% to 5% globally). Standard treatment consists of seven weeks of radiation therapy, and low- and middle-income countries often do not have enough to easily accessible therapy facilities.
Bentzen and colleagues conducted the HYPo- versus NOrmo-fractionated accelerated radiotherapy (HYPNO) trial, which was sponsored by the International Atomic Energy Agency in Vienna. The research included 792 patients from 10 countries (Argentina, Brazil, Cuba, India, Indonesia, Pakistan, the Philippines, South Africa, Thailand, and Uruguay). Participants had alcohol and tobacco-related advanced squamous cell head and neck cancer; the majority of tumors (50.5%) were in the oropharynx. Almost half (49%) had disease that had spread to the lymph nodes.
Study participants received either 33 radiation fractions over 5.5 weeks (66 Gy) or 20 fractions over four weeks (55 Gy). Most (76%) also underwent chemotherapy.
The researchers found that the shorter protocol was just as effective at controlling disease and did not increase treatment side effects: At three-year follow-up, those participants who had accelerated treatment had roughly the same level of locoregional tumor control and late-term side effects as those who received the longer treatment, as well as comparable overall survival and progression-free survival rates.
"There is actually a sweet spot where you get exactly the right balance between the total dose, the total treatment time and the dose you deliver in each fraction," Bentzen said in an ASTRO statement. "The net result is that you hit the tumor hard enough to get good control, but you don’t affect the normal tissue more than you would with the standard treatment."