It may seem like an April Fools' Day joke, but it's a painful reality for users of the Gamma Knife radiation therapy system from Elekta. Starting today, they will be paid 58% less for procedures performed with the system.
The cut is the result of legislation passed last year by Congress, which reduced Gamma Knife payments for Medicare patients from approximately $8,100 per procedure to $3,400. Seniors covered by Medicare represent approximately half of the 15,000 patients who are treated annually with the cobalt-60-based stereotactic radiosurgery (SRS) delivered with a Gamma Knife. The system is primarily used for brain metastases, but it is also used for other brain tumors, arteriovenous malformations, pituitary adenomas, and trigeminal neuralgia.
The reimbursement came in the form of a line item that was added on December 31 to the legislation that resolved the "fiscal cliff" budget impasse. It reduced the reimbursement rate set only 45 days earlier by the U.S. Centers for Medicare and Medicaid Services (CMS) under the 2013 Medicare Outpatient Prospective Payment System (OPPS) rule. When the legislation was passed later that night and signed into law by President Barack Obama, it became Section 634 of the American Taxpayer Relief Act (ATRA).
Equal reimbursement
The goal of Section 634 was to equalize reimbursement for Gamma Knife cobalt-60 treatment with that of linear-accelerator-based radiation therapy. But proponents of Gamma Knife treatment strongly disagree that the treatments are comparable, as Gamma Knife is only used to treat certain types of brain tumors, and it does so with a single treatment of a high radiation dose in a process that takes most of a day.
Gamma Knife patients have bolts surgically inserted so that their heads can be attached to a rigid frame. This isn't the case for linear-accelerator patients, who wear a head mold. Linear-accelerator-based SRS is used to treat brain disease, but lower radiation dose is used and multiple treatments may be needed.
Because of differences in these two treatments, CMS created two different payment rates years ago and has reviewed the rates annually. In the fall of 2012, CMS specifically considered and rejected a proposal to establish payment parity, stating that identical reimbursement would be inappropriate because the costs for each procedure differed significantly. Members of Congress overruled the agency in the fiscal cliff legislation, however.
The exception to this rule is cobalt-60-based cranial radiosurgery treatment performed in a rural hospital. However, none of the 130 hospitals and cancer treatment centers in the U.S. that operate Gamma Knife equipment are categorized as rural hospitals.
In March, the American Association of Neurological Surgeons and the Congress of Neurological Surgeons sent letters to majority and minority leaders in the Senate and House of Representatives, asking that Gamma Knife reimbursement be restored. Their jointly signed letter expressed concern that patients with serious brain disorders who would benefit from this specific treatment would lose access to the therapy if hospitals decide to no longer offer the treatment.
Over the past few months, the International RadioSurgery Association, a professional society of cobalt-60-based stereotactic radiosurgery users, has been lobbying Congress to enact legislation to restore payment. The association is also circulating a petition to this effect, and it has garnered more than 1,000 signatures and statements of support.





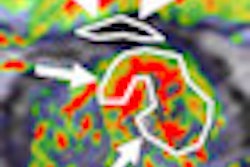





![A 53-year-old patient (patient number four) with a recurrent pituitary adenoma with extension of a cystic component of disease to the medial temporal lobe apparent on MRI (contoured in blue), and extension of disease to the left sphenoid bone and orbital apex apparent on [68Ga]Ga-DOTA-TATE (contoured in yellow).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/04/pituitary-tumor.QGsEnyB4bU.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)





