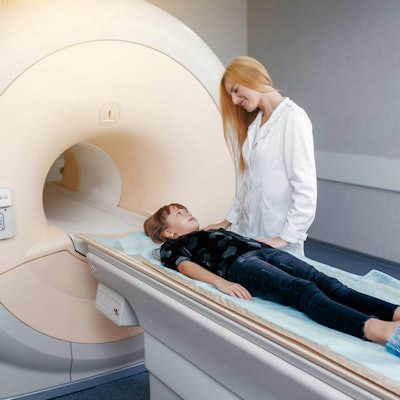
Reducing the use of sedation for pediatric brain MRI exams translates into "substantial cost savings" for the healthcare system, according to a study published December 21 in the American Journal of Roentgenology.
The findings could help radiology departments better manage their costs, especially in an era of alternative payment models (APMs), wrote a team led by Shireen Hayatghaibi, PhD, of Cincinnati Children's Hospital Medical Center in Ohio.
"The shift to alternative payment models, particularly those with capitated or bundled payments, necessitates understanding the cost for healthcare systems to produce covered care encounters," the group noted.
MRI is often used with children because it offers effective soft tissue contrast resolution and doesn't impart radiation. But MRI can be expensive compared to other imaging modalities, and when children have to be sedated, the complexity and cost of the exam increases, the authors noted. They cited a study that found that the use of sedation for pediatric brain MRI exams grew by seven percentage points between 2011 and 2014. Many radiology departments are trying to slow this growth, according to the investigators.
To assess the cost of pediatric brain MRI exams, Hayatghaibi and colleagues calculated pricing for 343 outpatient noncontrast brain MRI studies performed in 2019 at three academic children's hospitals, categorizing MRI exams as sedated or nonsedated. They calculated cost, including factors such as labor (cost rate for each type of staff involved in the exam process), equipment (total cost of MRI scanner and anesthesia monitoring machine), space (facility costs per square foot), supplies (sedatives), and exam duration.
| Cost for outpatient brain MRI across three pediatric institutions, sedated and nonsedated | ||
| Type of exam | Base cost | Range |
| Sedated MRI | $842 | $775 to $924 |
| Nonsedated MRI | $262 | $240 to $285 |
For both exam types, the largest cost category -- and the largest source of difference in cost among the three facilities -- was labor, Hayatghaibi and colleagues found. The factor with the most influence on overall cost was MRI exam duration.
"Health systems operating within alternative payment models can use this comparative cost information for purposes of cost reduction efforts and establishment of bundled prices," Hayatghaibi's team concluded in a statement released by the American Roentgen Ray Society (ARRS).
Of course, radiology departments still need to discern whether sedation is needed for pediatric patients undergoing brain MRI, Hayaghaibi told AuntMinnie.com.
"The necessity of sedation for MRI in children is complex and multifactorial," she said. "Certainly, sedation is [often] needed to reduce motion artifact in younger children, but the criteria for which child needs sedation is hospital-specific and varies across institutions."


















![Overview of the study design. (A) The fully automated deep learning framework was developed to estimate body composition (BC) (defined as subcutaneous adipose tissue [SAT] in liters; visceral adipose tissue [VAT] in liters; skeletal muscle [SM] in liters; SM fat fraction [SMFF] as a percentage; and intramuscular adipose tissue [IMAT] in deciliters) from MRI. The fully automated framework comprised one model (model 1) to quantify different BC measures (SAT, VAT, SM, SMFF, and IMAT) as three-dimensional (3D) measures from whole-body MRI scans. The second model (model 2) was trained to identify standardized anatomic landmarks along the craniocaudal body axis (z coordinate field), which allowed for subdividing the whole-body measures into different subregions typically examined on clinical routine MRI scans (chest, abdomen, and pelvis). (B) BC was quantified from whole-body MRI in over 66,000 individuals from two large population-based cohort studies, the UK Biobank (UKB) (36,317 individuals) and the German National Cohort (NAKO) (30,291 individuals). Bar graphs show age distribution by sex and cohort. BMI = body mass index. (C) After the performance assessment of the fully automated framework, the change in BC measures, distributions, and profiles across age decades were investigated. Age-, sex-, and height-adjusted body composition reference curves were calculated and made publicly available in a web-based z-score calculator (https://circ-ml.github.io).](https://img.auntminnie.com/mindful/smg/workspaces/default/uploads/2026/05/body-comp.XgAjTfPj1W.jpg?auto=format%2Ccompress&fit=crop&h=112&q=70&w=112)


