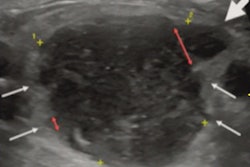
Ultrasound appears to be an effective point-of-care alternative to MRI for the evaluation of bone stress injury, according to a study published March 22 in the Journal of Ultrasound in Medicine.
MRI is typically used to assess bone injuries, but the study results suggest that clinicians may have a more easily accessible tool for this application, wrote a team led by Dr. Isaac Syrop of Columbia University in New York City and Dr. Yaeko Fukushima, PhD, of Kansai Medical University in Osaka, Japan.
"There are many advantages to ultrasound imaging over MRI, including its dynamic practicality, which provides the treating clinician with an opportunity to evaluate local soft tissue sites in real-time," the group wrote. "Ultrasound imaging takes significantly less time than MRI to perform ... and can be done as part of the clinical evaluation."
Bone stress injuries are common in young adult athletes, and can negatively affect performance over the long term, the investigators noted. It's crucial to diagnose these injuries early so that athletes can be treated effectively and return to play.
X-ray and CT aren't very effective for early diagnosis of bone stress injuries and expose patients to radiation; since the 1980s, MRI has been used as the diagnostic standard. But MRI is expensive and time-consuming.
"There is good reason to believe that the more affordable and accessible diagnostic option of musculoskeletal ultrasound imaging may help to address the shortcomings of MRI," the authors noted.
The researchers sought to compare the sensitivity and specificity of ultrasound to MRI in the diagnosis of bone stress injury through a study that included 37 young adult athletes presenting in an academic sports medicine clinic between 2016 and 2020 with suspected lower extremity bone stress injury. Sports included everything from crew, field hockey, gymnastics, and running to soccer, tennis, track, and volleyball. All patients underwent MRI and ultrasound exams.
Of the 37 study participants, 30 (81%) had bone stress injuries. The most common injuries were in the metatarsal bones (54%) and the tibia (32%).
Ultrasound scored relatively high across a range of performance measures relative to the gold standard of diagnosis on MRI scans, the group found.
| Performance of ultrasound for diagnosing bone stress injuries compared with baseline assessment MRI | |
| Measure | Performance |
| Sensitivity | 80% |
| Specificity | 71% |
| Positive predictive value | 92% |
| Negative predictive value | 45% |
"In summary, ultrasound imaging may be a point-of-care tool for the current practicing sports medicine provider to combine with their clinical evaluation in the diagnosis of bone stress injuries of the lower extremity," the team concluded.