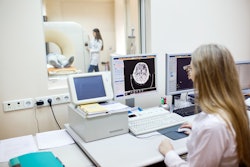
The most direct step every manager can take toward improving MRI safety is to designate individuals with responsibility for MRI safety best practices, according to an August 3 presentation at the 2021 AHRA meeting in Nashville, TN.
 Tobias Gilk.
Tobias Gilk.Presenter Tobias Gilk, senior vice president of Radiology-Planning, founder of Gilk Radiology Consultants, and an MRI safety advocate, noted that it has been 20 years since 6-year-old Michael Colombini died when a portable oxygen tank was brought into the MRI room (and was pulled from the anesthesiologist's hands, striking Michael in the face and head).
"In the 20 years since that accident, we've seen massive shifts in MRI technology, clinical application, reimbursement and revenue, new licensure and accreditation requirements, and safety training resources," Gilk said.
And yet, he asked, "Does your accreditation require MRI safety training for anesthesiologists? Have you ever heard of [American College of Radiology] accreditation being denied due to MRI safety lapses?"
Part of the problem is that we are still "drinking the Kool-Aid" as far as MRI safety is concerned, according to Gilk. A majority of the rules on radiology safety are geared toward ionizing radiation. And while there are rules for MRI machines and their safety, oversight of MRI exams at hospitals and outpatient imaging centers is almost nonexistent, he said.
Meanwhile, nearly 40 million MRI scans are performed per year. With a growing population, this number is expected to increase.
To help ensure safety at your site, Gilk recommended creating a safety "trifecta" -- three clearly established roles for individuals with designated responsibilities and authority, as follows:
- MR Medical Director (MRMD): The MRMD is the supervising radiologist, the chief clinical decision-maker, who is in fact ultimately legally liable for the safety in the MRI environment and the safe execution of MRI exams, whether they are clinical or research in nature. Gilk said many radiologists may not know the buck stops with them when they sign off on an exam.
- MR Safety Officers (MRSO): The MRSO usually is a radiologic technologist charged with executing the safety practices for the site based on orders by the MRMD or supervising physician. Importantly, one does not need to be certified to be designated as an MRSO, nor do sites need to hire someone new. Often, the MRSO can be recruited from the senior MR technologist staff, Gilk said.
- MR Safety Experts (MRSE): The MRSE can be a medical physicist or "super tech," Gilk suggested. The person in this role should understand at a root level why certain actions may be dangerous -- in other words, they can review safety based on an overall understanding that the laws of physics we're used to change in an MR environment.
Certification for these roles is available through the American Board of Magnetic Resonance Safety (ABMRS), which was launched in 2015 by Gilk and other MRI safety advocates to help standardize testing and certification for MR safety competence.
Ultimately, it might look good on paper for everyone to share responsibility for MRI safety, but when responsibility is diffused and an accident occurs, finger-pointing may begin, which leaves no one responsible. Technologists may feel obliged to step to the plate and accept responsibility, but essentially are "throwing themselves under the bus" because legally, that is not true, Gilk said.
Last year, the ACR updated its Manual on MR Safety to encourage sites to establish dedicated safety officer roles and more sites appear to be taking the advice, Gilk noted.
"We're making progress, just not fast enough," he said.
Thus, with a reminder that the shadow of the Michael Columbini tragedy still hangs over MR imaging 20 years after the incident, Gilk encouraged managers to make 2021 the "Year of MRI Safety" at their sites.