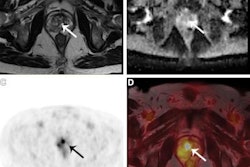
Black men are less likely to undergo MRI before prostate biopsy than their white counterparts, according to a study published June 23 in the American Journal of Roentgenology.
This discrepancy may translate into poorer patient outcomes, according to a team led by Dr. Christopher Gaffney of New York-Presbyterian Hospital in New York City. MRI before prostate biopsy has been associated with better results compared with a strategy that goes straight to biopsy.
Gaffney and colleagues conducted a study that used information from the Surveillance, Epidemiology, and End Results (SEER) program Medicare-linked database to identify men undergoing prostate biopsy who had an MRI exam within six months of diagnosis of prostate cancer. The men were categorized according to whether they had undergone prostate biopsy before or not.
The study included 82,483 men who had a prostate biopsy between 2008 and 2015; of these, 78,253 had never had a prostate biopsy before and 4,230 had known prior negative biopsy.
The team found that the percentage of patients who received an MRI before biopsy increased between 2008 to 2015 across a variety of categories: overall (from 0.5% to 9.2%); in men who had not had a prostate biopsy before (from 0.5% to 8.2%); and in men with a prior negative biopsy (from 1.4% to 25.5%).
But the odds of Black men undergoing MRI before biopsy was 0.4, half that of white men.
"The steady overall increase in the utilization of MRI before prostate biopsy since 2008 has been associated with significant racial and regional disparities in utilization," the team concluded.